September 4, 2025
Toe deformities can cause discomfort, affect your balance, and limit your footwear options. Among the most common conditions are clawed toes, hammertoes, and crossover toes. While they may sound similar, each has distinct characteristics, causes, and treatment approaches. Understanding the differences can help you identify symptoms early and seek appropriate care.
What Are Clawed Toes?
View this post on Instagram A post shared by Feet First Clinic (@feetfirstclinic_)
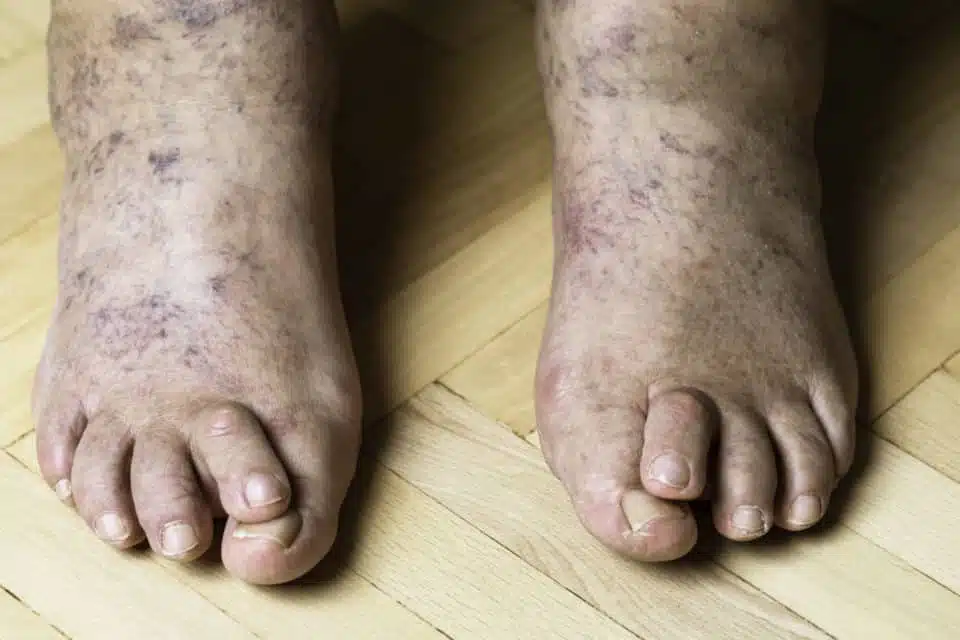
Clawed toes are characterized by an abnormal bending of the toe joints, causing the toe to curl downward like a claw. Typically, the toes bend upward at the joint where they meet the foot (the metatarsophalangeal joint), and then downward at the middle (proximal interphalangeal) and end joints (distal interphalangeal).
Causes of Clawed Toes
Neurological conditions such as diabetes, stroke, or multiple sclerosis that affect muscle control.
Muscle imbalances caused by arthritis or injury.
Wearing poorly fitting shoes that crowd the toes.
Symptoms of Clawed Toes
Toes curl downward permanently.
Pain or discomfort in toes or ball of the foot.
Calluses or corns on the top or tip of the toes due to friction.
Difficulty fitting into shoes comfortably.
What Are Hammertoes?
Hammertoes involve an abnormal bend in the middle joint of the toe, causing it to resemble a hammer. Unlike clawed toes, the bending mainly occurs at the proximal interphalangeal joint.
Causes of Hammertoes
Wearing tight or ill-fitting shoes that force toes into a bent position.
Muscle imbalance or weakness.
Injury or trauma to the toe.
Arthritis or other joint conditions.
Symptoms of Hammertoes
Toe bent downward at the middle joint.
Pain or irritation on the top of the bent toe.
Corns or calluses forming on the affected toe.
Limited toe movement.
What Are Crossover Toes?
Crossover toes occur when the second toe moves sideways, crossing over the big toe. This deformity often causes crowding and pressure between the toes.
Causes of Crossover Toes
Tight or narrow footwear.
Muscle imbalances or ligament laxity.
Structural foot issues like bunions.
Arthritis or prior injuries.
Symptoms of Crossover Toes
Second toe overlapping or crossing the big toe.
Pain between toes or on the side of the foot.
Corns or calluses where toes rub together.
Difficulty wearing certain shoes.
Treatment Options for Toe Deformities
Conservative Treatments
Proper footwear: Shoes with a wide toe box and good support can relieve pressure.
Orthotics: Custom shoe inserts can help correct foot mechanics.
Padding and taping: To protect affected toes from friction.
Physical therapy: Exercises to strengthen foot muscles and improve flexibility.
When Surgery May Be Needed
If conservative treatments don’t relieve symptoms or deformities worsen, surgical options may be considered. Procedures vary depending on the deformity but may include tendon release, joint fusion, or bone realignment.
When to See a Specialist
If you experience persistent toe pain, difficulty walking, or notice changes in toe shape, it’s important to consult a foot specialist. Early intervention can prevent complications and improve your foot health.
June 12, 2020
If you've experienced foot pain for some time or have a trauma injury, surgery has likely come to mind.
Surgery is a treatment of injuries or disorders of the body by incision or manipulation. Surgery is quite common for foot injuries and is done as a restorative measure.
Because of its invasive nature, considering the positives and negatives of surgery is important. You should not only weigh the direct impact of surgery but also the long-term effects.
There are several factors to consider when deciding on foot surgery:
Necessity
Success rate
Cost
Recovery time
Long-term effectiveness
With these in mind, you should take into account the positives and negatives of both. Does the recovery time justify getting surgery, for example? How about the long-term effectiveness of the surgery?
Below, we get into the case for, and against, foot surgery.
When is Foot Surgery Necessary?
Some foot conditions require surgery. You should explore all non-surgical options and physical therapy before foot surgery.
Certain foot conditions are progressive and are unlikely to get better without surgery. In these instances, one can consider surgery to improve their quality of life. A few examples of progressive foot conditions include severe bunions, rigid hammertoes, advanced arthritis (hallux rigidus). However, long before surgery is even considered, there are several conservative treatments that can slow down the progress and relieve pain.
That doesn't mean you can't live comfortably with the condition. Investing in proper shoes, doing physical therapy, and avoiding certain activities may relieve pain.
In the instance of hallux rigidus, you can maintain a high quality of life through physical therapy, proper orthotics, avoiding high-impact exercise, and working on flexibility. It's important to work on maintaining the range of motion in the toe. You can't get back more flexibility, but you can work to maintain the flexibility that you have. The bone spur will only continue to grow over time if excessive force or impact is placed upon the joint. However, since the osteoarthritis that breaks down the cartilage won't be able to recover, the resulting bone spur will likely grow over time, further limiting the range of motion.
Some people opt for a cheilectomy, which is an incision along the top of the toe to shave down a Bone Spur. In other cases, people opt for a fusion, which connects the first metatarsal with the phalanx. The connecting of the two bones fuses the area of the first metatarsophalangeal joint (MTP joints).
For those with a bunion, you'll want to explore all non-invasive measures before deciding on surgery. If you have explored all options, surgery may be an option. Typically, those who experience significant pain, have severe toe deformities, and have chronic inflammation are the likely candidates for surgery. Bunion surgery (of which there are a few) can include several correct measures:
Realigning the metatarsophalangeal (MTP) joint at the base of the big toe.
Pain relief.
Correcting the deformity of the bones, especially if your big toe is drifting inwards towards your second metatarsal.
Another example is rigid hammertoes. When the toes start to drift, grip or claw because of excessive misalignment of the big toe (bunion) or the entire foot itself (flat feet). It is always imperative to start with conservative treatment options such as silicone toe crutches, orthotics, metatarsal pads, and wearing the proper sized shoes width and length. If pain persists and the hammer toes progress and further deviate, then surgery is recommended. For flexible hammertoes, the most common surgery is Tendon lengthening which releases the pull under the toe. For more rigid hammertoes, joint resection is recommended, which is the removal of the end of the bone to allow for more range of motion. If the joints have too much arthritis, joint fusion is recommended to fuse the bones together and create a straight toe.
When is Foot Surgery Not Necessary?
Generally, you can treat foot conditions without operational procedures. The body is incredibly resilient when it comes to injuries, and many foot conditions can be treated with a proper plan.
Surgery is usually seen as a last resort because there is significant rest needed afterwards, the occasional complication, and sometimes nerve damage. Surgery can also be expensive if it's not covered under provincial or private insurance. Finally, surgery might fix the obvious problem, but may not solve the underlying issue. This means that the foot condition may return in the future.
For the examples mentioned above - hallux rigidus, bunions, and hammertoes - all have recommended treatment options that don't involve surgery. Working with a foot professional to determine the underlying cause, like a muscle imbalance, for example, can help treat the resulting condition, and can be better for your body in the long run. This can be done through a foot assessment by a chiropodist, complete with a biomechanical and gait analysis.
Surgery also can take weeks, if not months to recover from. Make sure to incorporate several weeks of recovery into the discussion when considering foot surgery. Recovery time may otherwise be used to build a habit of incorporating physical therapy into your routine. Consider the opportunity cost of the severity of the surgery as well as the recovery time.
For most foot conditions, there are a number of treatment options you should consider including:
Rest
Icing/compression
Strength-training
Custom orthotics
Proper footwear
Physiotherapy
Over-the-counter footwear products like Bunion Socks
Any number of these treatment options may be able to provide the relief you need. Remember, you might not see results right away. In some cases, incorporating these treatments may take weeks, if not months, to result in meaningful change. However, those habits will continue to benefit you for the rest of your life.
There's no hard and fast rule for in cases for and against surgery. Always consult a medical professional when deciding upon the best course of action, and see if foot surgery is recommended.
February 27, 2019
Whether it’s a pair of black patent leather pumps, sky-high ruby red stilettos or strappy sandals, high heels are considered wardrobe staples that belong in a woman’s closet. They’re used for special occasions and everyday work-life, going out dancing or going for an important interview. Sadly, these beloved fashion statements can damage parts of your body over time.
Anyone who has ever worn a pair of high heels knows that after a few hours of standing and walking, your feet are throbbing. It’s a relief just to slip them off, sit down and let your pulsing toes have a little bit of a rest. These aches and pains come after only a few hours of wearing the shoes — the long-term effects are much worse. There are many different ways that high heels can harm not just your feet, but your entire body.
Bunions
One of the health problems that people can get from wearing high heels is developing large bumps called bunions on the outsides of their big toes. A bunion is a permanent, progressive side-effect. The only way to reverse it is corrective surgery to remove part of the bone and adding screws to keep the foot in an appropriate position.
While bunions cannot be reversed, the progression can be managed. One way is to avoid high heels, which will aggravate the issue. It's also important to get a foot assessment with a chiropodist: bunions are usually caused or contributed to by an underlying biomechanical issue, so addressing that is the first step.
Hammertoes
Another one of the distressing things that high heels do to your feet is create hammertoes, which is when your little toes bend and buckle from the pressure of standing on them. Hammertoes are awkward and sometimes painful. Flexible hammertoes can be reversed through physiotherapy, orthopedic shoe replacements or corrective surgery.
Joint Damage
Other than foot problems, high heels prematurely age your joints because they don't allow your knee to straighten to accommodate for the additional weight placed on your legs. The reflex changes your gait (how you walk) and wears down your knees over time.
Achilles' Tendonitis & Haglund's Deformity
Regular use of high heels can lead to shortened Achilles' tendons, which can create tendinitis issues - and with that comes a lot of ankle pain. The Achilles tendon is the tendon at the back of our heel that connects our heel to our knee. A shortened Achilles tendon will also cause rubbing and pressure on the back of the heel creating a bump known as a Haglund's deformity, which is permanent spurring and deformation of the heel bone. For those who wear high heels because they want their feet to look nice, a deformity on the heel can be quite counter-productive.
Back Pain
You’ll also find that high heels cause lower back pain by forcing your lower back to arch to compensate for the fact that you’re balancing your body weight on the balls of your feet. High heels induce a forward pelvic tilt, which forces the lower back into a more exaggerated curve. The shoes force your body weight to pull forward, so you lean back when you stand. The position puts a lot of stress on your spinal discs. Sticking with the shoes can lead to poor posture, persistent aches and muscle spasms. It can also lead to chronic lower back, hip and knee pain.
Skin & Toenail Issues
High heels place excess pressure on the forefoot. With pressure, comes friction, which can lead to painful corns, calluses and blisters. The increased pressure on the big toe, especially if your high heels are also narrow, can also lead to ingrown toenails.
Alternatives to High Heels
Sometimes it's hard to avoid high heels altogether, but there are alternatives:
Reduce the frequency with which you wear high heels
Invest in orthopaedic high heels with a wider toebox, cushioned forefoot, and thick heel.
Try supportive insoles for high-heels.
Try dress flats instead.
While not a perfect solutions, these suggestions will give your feet a little extra support and mitigate the damage from wearing high heels.
It’s clear that high heels are not worth the aches and pains that they put you through. These fashion fundamentals damage your feet, your knees and your back much more than you think. Push those sandals, stilettos and pumps to the back of the closet — it’s time to change up your footwear.