October 16, 2025
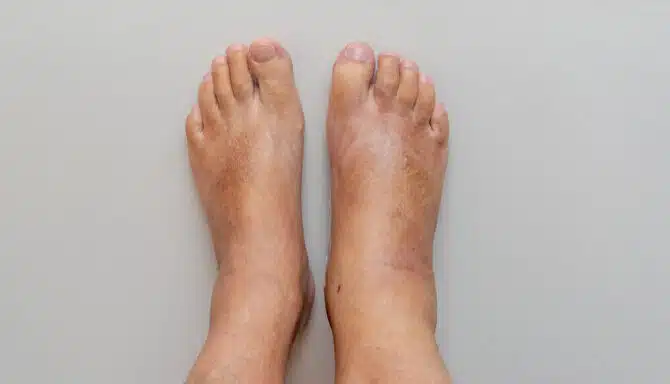
Diabetes is a chronic condition that affects many parts of the body, including your feet and toenails. Proper foot care is especially important for people with diabetes because they are at a higher risk of developing complications that can impact mobility and overall health. Understanding how diabetes affects toenails can help you prevent problems and maintain healthy feet.
Why Diabetes Impacts Toenail Health
People with diabetes often experience poor circulation and nerve damage (neuropathy) in their feet. These issues make it harder for wounds and infections to heal and can reduce sensation, so small injuries or infections may go unnoticed. Toenails can also become more vulnerable to damage, infections, and deformities.
Common Toenail Problems in People with Diabetes
1. Fungal Infections
Diabetes can weaken the immune system, making it easier for fungal infections like athlete’s foot or toenail fungus to develop. Fungal toenails may become thickened, discolored, brittle, and painful.
In addition, good circulation is required for the natural moisturization processes in the toenails and feet. Diabetes disrupts blood flow to the feet, which means they can't properly moisturize themselves. This dries out the toenails and causes them to become brittle. It also dries out the skin, which can cause small cracks and abrasions. Fungus can then more easily penetrate through brittle cracked toenails and abrasions. Once it does, it's harder for your body to fight the infection due to diabetes' affect on the immune system.
2. Ingrown Toenails
Reduced sensation means small cuts or ingrown toenails might not be felt immediately, increasing the risk of infection. Ingrown toenails can cause redness, swelling, and pain if left untreated.
3. Toenail Discoloration and Deformities
Poor circulation and infections may cause toenails to change color, thicken, or become deformed. This is because circulation is required to facilitate the toenail growth process. When this process is disrupted, it causes nail cells to build up on top of each other rather than beside each other, which causes thickening and an irregular toenail shape. This can make nail trimming difficult and increase the risk of injury.
4. Delayed Healing
Any cuts or injuries around the toenails heal more slowly in people with diabetes, increasing the chance of complications like ulcers or infections.
Tips for Preventing Toenail Problems with Diabetes
Practice Good Foot Hygiene
Wash your feet daily with warm water and mild soap.
Dry your feet thoroughly, especially between the toes.
Keep Toenails Trimmed and Clean
Cut nails straight across to prevent ingrown toenails.
Avoid cutting nails too short or rounding the corners.
Wear Proper Footwear
Choose shoes with a wide toe box and good support.
Avoid tight or narrow shoes that can cause pressure and injury.
Regular Foot and Toenail Checks
Inspect your feet daily for cuts, blisters, redness, or swelling.
Have a healthcare professional, like a chiropodist, examine your feet regularly.
Manage Blood Sugar Levels
Keeping blood glucose under control supports overall foot health and healing.
When to See a Foot Specialist
It is recommended that people with diabetes include a chiropodist in their healthcare team and see them on a routine, ongoing basis for diabetic foot care. When it comes to diabetes, prevention is the best treatment.
If you notice any signs of infection, persistent pain, changes in nail appearance, or wounds that don’t heal, it’s essential to seek professional care promptly. Early intervention can prevent serious complications, including foot ulcers and infections that may lead to amputation.
April 3, 2025
Healthy toenails need healthy circulation, but when blood flow is compromised, they can become brittle, discoloured, or grow slowly. Additional toenail conditions can also develop. Poor circulation and toenail problems are closely linked, especially for those with health problems like diabetes or peripheral artery disease. Understanding why poor blood flow affects toenails can help you take the right steps to protect your foot health and prevent complications.
https://www.youtube.com/shorts/3JAUqiqJfus
The Importance of Blood Circulation
In order to understand the link between poor circulation and toenail issues, we have to start by understanding what blood flow is and what it does. The circulatory system, comprising the heart, blood vessels, and blood, serves as the body's transportation network. Its primary function is to deliver oxygen and essential nutrients to cells while removing waste products like carbon dioxide.
The heart pumps oxygen-rich blood through arteries, which branch into smaller arterioles and capillaries, reaching every tissue and organ. This process ensures that each cell receives the necessary components for energy production, growth, and repair.
Efficient blood circulation is vital for overall health. Oxygen transported by red blood cells is crucial for cellular respiration, the process by which cells generate energy. Nutrients absorbed from digested food are distributed via the bloodstream to support various bodily functions.
Key nutrients delivered by the bloodstream include:
Glucose: A simple sugar derived from carbohydrates in our diet, glucose serves as the primary energy source for cells, fueling various physiological processes.
Amino Acids: These are the building blocks of proteins, obtained from the digestion of dietary proteins. Amino acids are crucial for tissue growth, repair, and the synthesis of enzymes and hormones.
Fatty Acids and Lipids: Essential components of cell membranes and energy storage molecules, fatty acids and lipids are transported to cells for incorporation into cellular structures and for energy production.
Vitamins and Minerals: These micronutrients support a range of cellular functions, including maintaining bone health and facilitating nerve transmission.
Hormones: Although not nutrients in the traditional sense, hormones are vital signaling molecules transported by the circulatory system to regulate various physiological activities, such as metabolism, growth, and mood.
Impaired circulation can slow down healing processes—even for seemingly innocent and minor problems like cuts and scrapes. Likewise, organs and tissues deprived of adequate circulation can suffer damage over time, increasing the risk of conditions such as peripheral artery disease, stroke, and heart attacks.
Toenail Health and Circulation: The Connection
The circulatory system delivers oxygen and essential nutrients to the nail beds, supporting the growth and maintenance of strong, clear nails. When blood flow is compromised, the nails may not receive adequate nourishment, leading to various issues such as brittleness, discoloration, and slowed growth. In some cases, poor circulation can cause nails to develop ridges, indicating underlying vascular problems.
Reduced blood flow can also increase the risk of infections like toenail fungus (onychomycosis). A weakened circulatory system impairs the body's ability to combat pathogens, making the toenail environment more susceptible to fungal overgrowth. This often results in yellowed, thickened nails that you can’t treat without the help of a chiropodist or podiatrist. They must remove the infected portion of the nail so they can apply the correct medicine.
Poor blood flow on its own may not cause a problem with your foot health, but it can contribute to the following toenail conditions:
Slow or halted nail growth: Inadequate blood flow deprives the nail matrix of essential nutrients and oxygen, resulting in reduced or ceased toenail growth. This can be very frustrating if your toenail falls off or cracks and you’re waiting for it to grow back, leaving your feet vulnerable.
Brittle and discolored nails: Insufficient circulation can cause nails to become brittle and change color, often appearing yellowed or darkened.
Thickened nails: Poor blood flow may contribute to the thickening of toenails, often via toenail fungus, making them difficult to trim and maintain. Poor blood flow also affects the nail growth process, which can cause nail cells to pile on top of each other and lead to thicker toenails.
Ingrown toenails: While not directly caused by poor circulation, individuals with compromised blood flow, such as those with diabetes, are at higher risk for complications from ingrown toenails, including infections and delayed healing.
Diabetes, Toenail Health and Circulation
Diabetes can lead to two significant complications affecting foot health: diabetic neuropathy and peripheral artery disease (PAD). Diabetic neuropathy results from prolonged high blood sugar levels damaging the nerves, particularly in the legs and feet, causing numbness, tingling, or a loss of sensation.
This diminished sensitivity means that innocent injuries, such as cuts or blisters, may go unnoticed, increasing the risk of infections and complications like ulcers, or in severe cases, life threatening problems like gangrene, which require amputation. This is also the case for seemingly minor problems with the toenails. Simultaneously, PAD causes blood vessels to narrow and harden, reducing blood flow to the extremities. This impaired circulation hampers the delivery of oxygen and essential nutrients needed for healing, making the feet and toenails even more susceptible.
Regular foot inspections and nail care with a chiropodist or podiatrist, maintaining proper hygiene, and promptly addressing any abnormalities are crucial steps for diabetics to prevent toenail-related complications stemming from poor blood flow.
https://www.youtube.com/shorts/QFWBwM6mGqM?feature=share
Foot and Nail Care for Poor Circulation
Maintaining proper foot and nail care is essential for individuals experiencing poor circulation, as reduced blood flow can lead to various complications. Here are some recommended practices and treatments:
https://youtu.be/5PCZuM5E6RU
Regular Exercise: Maintaining good circulatory health through regular exercise, a balanced diet, and avoiding smoking is essential for ensuring that the body's systems function as well as possible. One of the best circulation maintenance tips for foot health is working the muscles in the lower extremities. Exercises like toe splays, toe flexes and raises, massage ball rolls, pen pick-ups and seated toe pulls can work wonders. Click here to learn the five best foot exercises to improve blood circulation. They’re particularly helpful in the winter, but are useful all year round.
Regular Self Inspections: Conduct daily checks for cuts, sores, or changes in nail color and texture to detect issues early.
Moisturizing: Keep feet hydrated to prevent cracks and fissures that can lead to infections. Learn how to moisturize properly here.
OnyFix Nail Correction System: For those with ingrown or involuted toenails, the OnyFix system offers a non-invasive, pain-free solution. This innovative treatment involves applying a composite material to the nail, which helps guide it back to its natural shape as it grows, without the need for surgery. It's suitable for various nail shapes.
Medical Pedicures: Unlike traditional cosmetic pedicures, medical pedicures are performed by trained foot care professionals, such as chiropodists or podiatrists, in a sterile environment in a foot clinic. They focus on health, addressing issues like nail trimming, callus reduction, and infection prevention. They are especially helpful for dealing with irregular shaped toenails caused by poor circulation - cutting and maintaining these on your own can be very difficult. For people with diabetes, who are at higher risk for foot complications due to poor circulation and neuropathy, medical pedicures are a common and recommended treatment. These specialized pedicures help prevent complications like infections or ulcers by ensuring meticulous foot care.
Proper Footwear: Wear well-fitting shoes that provide adequate support and reduce pressure points to promote better circulation.
Proper Nail Trimming: Trim nails straight across and avoid cutting them too short to prevent ingrown toenails. And if your toenails are too thick or difficult to cut on your own, book an appointment with a foot specialist.
February 6, 2025
The HOKA trend is the rise in popularity of HOKA's high-stack running shoes, or running shoes with extra cushioning, extra height, a high heel stack and a rocker sole. They aren’t the first popular running shoes trend, and they certainly won’t be the last. Although people exclusively associate this type of trendy running footwear with HOKA, many other brands like ASICS and Saucony make footwear with the same high-stack shoe technology. Today, we’re diving into why these shoes offer more than just style—they come with real benefits. But they’re not for everyone, so we’ll also cover who should steer clear of this particular design.
https://www.youtube.com/shorts/ySn158c143c
What are High-Stack Running Shoes?
High-stack running shoes, often called “super cushioned” or even “chunky,” by those who don’t know the terminology. They have transformed modern footwear design for many high-quality brands. Often attributed to HOKA for “starting the craze," these shoes feature thick midsoles packed with advanced cushioning foam technologies that enhance energy return, provide sufficient shock absorption, and improve comfort over long distances.
Despite their benefits, high-stack shoes aren’t without controversy. Some runners prefer lower-profile shoes for better ground feel and stability, while others find high-stacks beneficial for injury prevention and endurance. Their chunky aesthetic has also sparked mixed opinions—some love the bold look and the added height without having to wear a true high heel while others see them as clunky.
High-Stack Shoe Technology
The defining feature of high-stack shoes is their thick midsole, which can measure over 40mm in some models. These midsoles use lightweight, resilient foams such as Pebax or EVA blends that provide exceptional cushioning while maintaining responsiveness. The goal is to reduce muscle fatigue by absorbing more impact, allowing runners to maintain performance with less strain on joints and soft tissues.
Another key factor in their performance is the rocker geometry, rocker bottom shoe or rocker sole—curved soles designed to promote a smooth heel-to-toe transition. This feature helps conserve energy, particularly during long runs, by reducing the work done by the calves and ankles.
ASICS Gel Nimbus 27
The Benefits of High Stack Shoes
High-stack running shoes offer several benefits for foot health, especially for individuals dealing with arthritis, diabetes, and metatarsalgia. Here's a breakdown of their advantages:
Enhanced Cushioning: High-stack running shoes feature extra cushioning, which absorbs shock and reduces impact on the feet during movement. This is particularly beneficial for people with conditions like arthritis, where joints are sensitive to pressure and movement.
Pressure Redistribution: The additional cushioning and rocker sole work together to redistribute pressure across the foot. In the case of diabetes or metatarsalgia, this can help alleviate excess pressure on specific areas of the foot, such as the forefoot or metatarsal heads. For those with diabetes, reducing pressure can help prevent the skin damage that leads to ulceration, as it lowers the risk of tissue damage and enhances comfort. (However, people with diabetes and balance issues may wish to avoid rocker soles - more on that later).
Joint Protection: The rocker sole limits the motion of foot joints. This helps manage conditions like osteoarthritis and hallux limitus (big toe arthritis). By restricting unnecessary movements, it prevents excessive strain on the joints, protecting them from further damage. This is especially useful for the big toe joint, where excessive motion can lead to increased pain and discomfort. It's also highly beneficial for people with high arches. People with high arches tend to experience joint rigidity (particularly hallux limitus) and lack of shock absorption. The rocker sole offsets the restricted mobility.
Improved Biomechanics: The curved design of the rocker sole encourages a smoother, more efficient gait. The shape propels the foot forward with each step, facilitating a natural walking motion and reducing strain on the joints. This is particularly beneficial for those with ankle, midfoot, or big toe arthritis, as it helps maintain normal walking patterns without overloading the affected areas.
Pain Reduction: Rocker soles are especially effective in reducing pain associated with conditions like hallux limitus and metatarsalgia. By minimizing motion at the big toe joint and redistributing pressure under the ball of the foot, these shoes can significantly reduce the discomfort felt during daily activities like walking or standing.
https://www.youtube.com/shorts/qByZ0GRFoaQ
When to Avoid High Stack Shoes
Here are some individuals who might want to avoid them or consult a foot care professional, like a Chiropodist or a Podiatrist, before wearing them:
People with Balance Issues
The rocker sole on high-stack shoes can make them less stable for individuals who struggle with balance or proprioception (awareness of body position). Those at a high risk of falls, such as elderly individuals or those with severe neuropathy, may find that the rocker sole from stacked heels throws off their balance.
People with Diabetes
Complications from diabetic neuropathy can lead to balance issues. Therefore, while the cushioning of a stacked heel is great for addressing joint issues, the "rolling" effect of the rocker sole is not suitable for people with diabetes.
Individuals with Ankle Instability
The increased midsole height and curved design can reduce ground feel and make it easier to roll an ankle, especially on uneven surfaces. People prone to ankle sprains or with a history of ankle instability might be better suited to lower-profile shoes with more lateral stability, or stability shoes with posting in the midsole (like the ASICS Gel-Kayano), which is constructed to cradle the foot and control ankle movement. In shoes like the ASICS Gel-Kayano, even though there is a stacked heel, the foot actually sits below the sole to provide stability.
https://www.youtube.com/shorts/osC-UmBtgNk
December 19, 2024
As the colder months roll in, it's important to pay extra attention to your feet. Studies show that foot exercises in the winter can help prevent stiffness and pain by improving blood flow, and keep your feet feeling warm and energized. This is especially important for people with certain foot conditions. By incorporating simple exercises into your routine, you can keep your feet in better shape, even as the temperature drops. Keep reading for five of the best foot exercises to boost circulation and keep your feet healthy throughout the winter.
Today We'll Learn
How Foot Exercises Can Improve Blood Circulation in Cold Winter Months
What foot conditions benefit the most from improved circulation
The 5 best foot exercises to improve circulation in winter
How these foot exercises improve blood flow
How Foot Exercises Can Improve Blood Circulation in Cold Winter Months
The circulatory system, also called the cardiovascular system, is responsible for delivering nutrients and oxygen to every part of our bodies. Sufficient blood circulation is very important to the lower extremities, like the feet, ankles and legs, because it helps reduce the risk of muscle cramps and fatigue by removing waste products like carbon dioxide and lactic acid, while also supporting cell repair and overall function.
Poor circulation can lead to swelling, numbness, and cold sensations in your limbs, hands and feet. It can also be connected to serious issues, like diabetes, which can lead to slow-healing wounds, infections, or even ulcers.
Maintaining good blood flow in the legs, ankles, and feet is even more important during the winter because cold temperatures cause blood vessels to constrict, which reduces blood flow to the extremities even more than usual. This can make feet and ankles more prone to stiffness, pain, numbness, and feeling cold.
Maintaining healthy blood flow via foot exercises helps improve mobility, soothes pain, and ensures the feet and lower limbs remain as strong as possible during the cold winter months. They also help people who simply want to keep their feet healthy and stay on top of their winter foot care.
Blood Circulation Exercises for Feet: Conditions Treated
Foot exercises and stretches that boost blood flow can help a wide range of conditions, including:
Diabetic Neuropathy: Improved circulation might help your body’s circulatory system deliver oxygen and nutrients to nerve tissues. This can help with tingling, numbness and nerve damage.
Edema (Swelling): Foot exercises stimulate the muscles that help the veins pump blood from your feet back up to your heart. This helps prevent fluid accumulation in the feet and ankles, which in turn reduces swelling in the lower limbs.
Peripheral Artery Disease (PAD): A common condition that narrows the arteries that restricts blood flow. Foot exercises may alleviate pain and cramping while improving mobility and making walking easier.
Raynaud’s Phenomenon: A condition in which extremities, like the hands and feet, are particularly sensitive to cold weather, causing the blood vessels to narrow (which then leads to poor circulation and all the other things we mentioned). Stretching and exercising the feet encourages blood flow, which can counteract the effects of Reynaud's.
Varicose Veins: These are enlarged, twisted and sometimes painful veins. Exercises that strengthen calf and foot muscles may reduce blood pooling in the veins, while minimizing discomfort and clot risks.
Plantar fasciitis: An overuse injury that causes inflammation in the plantar fascia and heel pain that comes and goes. Good circulation is essential to help your body heal injuries, so activities that boost circulation may decrease inflammation and speed up the recovery process.
Arthritis: Increased blood flow delivers oxygen and nutrients to joint tissues, reducing stiffness and improving joint mobility.
1. Foot Massage with Tennis Ball
https://www.youtube.com/shorts/cyHPLNoTPwQ
How to do it:
While standing, place one foot on the tennis ball and press down gently. Roll the bottle back and forth under your foot, starting from the heel and moving to the toes. Use your body weight to adjust the pressure, ensuring it's comfortable but effective.
Roll each foot for about 1–2 minutes. Focus on different areas, such as the arch and ball of the foot, to help relieve tension and boost circulation.
You can also use a lacrosse or golf ball, or a therapeutic massage ball.
2. Toe Splays
https://www.youtube.com/shorts/gOwgyrmU6hM
How to do it:
While seated, plant your feet flat on the ground.
Bunch your toes together by scrunching them inward, keeping the movement controlled.
Press your big toe firmly into the ground while spreading the other toes as far apart as possible, holding before relaxing.
Perform on both feet at the same time, or one foot at a time.
3. Toe Flex and Raises
https://www.youtube.com/shorts/n46k32OZgco
How to do it:
Start in a seated position with your feet flat on the floor.
Flex your toes upward towards the sky before flexing them downwards towards the floor.
Repeat 10-15 times on each foot.
4. Pen Pick-Ups
https://www.youtube.com/shorts/5PCZuM5E6RU
How to do it:
Stay seated.
Lay three pens, or similarly shaped objects, in front of you--spaced apart evenly.
Using your toes, pick up each pen and place it in a bowl.
5. Seated Toe Pulls
https://www.youtube.com/shorts/7-XrzvpxETc
How to do it:
While sitting on a chair and cross one foot over the opposite knee.
Pull your toes toward you and hold them in that position for 30-50 seconds.
Repeat 2-3 times on each foot.
How These Foot Exercises Improve Blood Flow
Exercises like the tennis ball massage boost blood flow by stimulating the muscles on the bottom of the foot. In more scientific terms, they target the plantar aspect (sole of the foot), which stabilizes the arch. It also releases tension in the plantar fascia, improving its elasticity and promoting better circulation in the surrounding tissues. This enhanced blood flow helps deliver oxygen and essential nutrients to the area, aiding in healing and reducing inflammation. Additionally, as the blood vessels dilate, the foot’s tissues become more flexible and less prone to tension.
Toe splays, toe flexes and raises, and similar exercises activate the intrinsic muscles of the foot. These muscles are located within the foot itself, as opposed to the extrinsic muscles that originate in the lower leg and insert into the foot.
These intrinsic muscles help control fine movements of the toes, stabilize the arch, and support balance. When they're activated during toe exercises, they stimulate the foot's blood vessels and promote better circulation. More specifically, working the toes can enhance venous return, which is the process by which blood is pumped back to the heart. The activation of these foot muscles also helps compress the veins, aiding in the movement of blood against gravity.
By targeting the small, intrinsic muscles, these exercises help to balance the workload between the foot’s various structures, preventing overuse injuries in the larger, more externally located muscles. Strengthening these muscles can also improve overall posture and movement patterns, reducing the risk of misalignments or discomfort that may radiate through the legs and lower back. When the foot muscles are conditioned and have good range of motion, they allow for better shock absorption and energy transfer during activities like walking, running, and standing. This reduces strain on other parts of the body, contributing to overall musculoskeletal health.
Furthermore, foot exercises like toe flexes, raises, and splays support better sensory feedback from the ground, enhancing proprioception—the body's ability to sense its position and movement. Improved proprioception helps with balance and stability, particularly in individuals who may be recovering from an injury or who experience frequent falls due to weakened muscles or poor circulation. By exercising the foot muscles, the brain receives clearer signals from the feet, which can enhance coordination and response times during daily movement. This can be particularly helpful for older adults or individuals with conditions that affect motor skills.
December 5, 2024
Seasonal changes can significantly impact diabetic foot health. In the summer, heat and sweating can create challenges, while cold temperatures and wet weather during the winter present other risks. That's why diabetic winter foot care is so important. Today we'll talk about:
You'll learn all about:
The connection between diabetes and foot health
The importance of diabetic foot care in the winter
Our Foot Specialists' top tips for diabetic winter foot care
The Connection Between Diabetes and Foot Health
https://www.youtube.com/shorts/4P3UiDSFzr4
Approximately 800 million adults worldwide have diabetes. It isn’t often immediately recognized as a foot condition on its own, but a serious issue called diabetic foot (a broad term encompassing a wide range of problems) can occur. As a result, foot care should be a top health priority for people with diabetes.
Reduced Blood Flow
People with Diabetes are at risk of developing neuropathy. There are four types, with peripheral symmetric neuropathy (which affects the feet and hands) being the most relevant for diabetes patients.
This condition develops when elevated glucose levels lead to a series of metabolic and vascular changes that impair nerve function. Over time, excess glucose triggers oxidative stress and inflammation, damaging the small blood vessels (microvasculature) that supply the nerves. Without adequate blood flow, nerves are deprived of oxygen and essential nutrients, resulting in their gradual deterioration.
Reduced Sensation
This damage primarily affects sensory nerves, which are responsible for transmitting pain, temperature, and pressure signals to the brain. This progressive loss of sensation makes it difficult for individuals to detect injuries or changes in their feet, such as cuts, blisters, or pressure points. These minor skin issues can turn to diabetic ulcers (open sores or wounds) when ignored.
Reduced Immune Function
Diabetes can also contribute to ulcer formation due to its impact on the immune system. High blood sugar levels over time impair the function of white blood cells, which are essential for fighting infections and promoting wound healing. When blood glucose levels are consistently elevated, it reduces the ability of these immune cells to properly respond to bacteria or other pathogens. This makes it more difficult for the body to prevent wounds that may develop on the feet - including minor cuts, blisters, pressure sores or even calluses - from getting infected. As a result, these small injuries are more likely to become infected, and ultimately lead to diabetic ulcers.
The impaired immune function, combined with poor circulation and reduced sensation, creates a perfect environment for these infections and ulcers to progress, further delaying healing and increasing the risk of severe complications, such as deep tissue infections or gangrene.
Why is Diabetic Foot Care Important in the Winter?
Cold and wet weather can impact everyone's feet, but winter can have a more severe effect on people with diabetes.
Cold Weather and Diabetes: Risk Factors
Low temperatures: Cold air can reduce circulation by constricting blood vessels, particularly in the lower extremities, making it even more difficult for already-compromised vessels to supply the feet with sufficient oxygen and nutrients. This further impairs the body’s ability to heal wounds.
Wet conditions: Snow, rain and sleet getting into your shoes and socks is a recipe for disaster for diabetics. You can develop blisters, sores and infections (which are all ulcer risks) when you let moisture build for too long.
Dry skin: On the other hand, it is also not ideal for your skin to be too dry. By nature, cold air is very dry. Indoor heating makes the air even dryer by extracting humidity. The lack of moisture in the air dries out the skin - including the skin on our feet. This makes calluses form faster and can lead to issues like cracked heels. And since diabetes impairs the body's ability to heal dry skin and cracked heels, the cracks can easily split open, get infected and turn into a diabetic ulcer.
Winter Foot Care for Diabetics
Podiatrists and chiropodists strongly advise individuals with diabetes to take extra care of their feet during the winter months due to the increased risks posed by the elements. If you have diabetes, keep reading to learn the best tips for winter foot care - all recommended by the foot specialists at our Toronto foot clinic.
Practice Skin Care
https://www.youtube.com/shorts/1-Sf43woLLE
Moisturizing your feet regularly is one of the most important steps to combat dry, cracked skin. However, our foot specialists also caution against using harsh creams full of chemicals and fragrances - especially if you have diabetes. Opt for medically respected products with natural ingredients, like Gehwol’s Lipidro and Dermal Therapy Heel Care, that replenish the natural amount of moisture in the skin while also healing cracks.
Only moisturize your feet after thoroughly cleaning and drying. Check out this ultimate guide to moisturizing your feet to master four easy steps. While you're at it, check out the best foot hygiene routine.
Perform Foot Stretches and Exercises
Movement is one of the most effective ways to manage diabetic foot concerns and counteract the impact of cold weather on blood flow. Low-impact cardio exercises such as swimming and walking can assist people in managing blood flow and sensation loss, respectively. Removing the elements of competition and high strain exertion found in other sports, and focusing solely on safety and motion, is a great way to encourage activity.
There are also targeted, low-impact and easy-to-perform foot stretches and exercises designed for people with diabetes. The goal is to stimulate blood circulation as much as possible while still considering any physical limitations. Below are three light exercises you can try from home, and while they may be hard to perform at first, practice makes perfect!
Toe Curls: Sit with your back straight, feet planted, and use a towel to scrunch your toes and pull it toward you, repeating five times per foot.
Figure Eights: Lift one foot while keeping the heel on the floor, move your foot in a "figure eight" motion, repeating five to 10 times per foot in each direction.
Single Leg Lifts: Stand with feet shoulder-width apart, hands on hips, and lift your left foot straight out in front, keeping your leg straight and foot flexed, repeating five times per foot.
To learn more about these exercises, check out the best stretches and exercises for diabetes.
Practice Moisture Control
Keep your feet reasonably dry as much as possible. This may mean changing your socks and shoes several times per day, and thoroughly drying your feet with a towel intermittently. While this can be annoying and easy to forget during the busy winter season, it’s important to stay on top of this with snow, sleet and rain posing an extra risk.
It’s important to not go overboard with too much direct heat penetrating your feet. While cozying up by the fire is safe on occasion, excessive heat can cause even more damage to the nerves. This is due to reduced sensation in diabetic individuals, which makes it harder to notice high heat and burns.
Below are the best ways to manage excessive moisture during the winter:
Wear moisture-wicking socks.
Change socks regularly, especially if they get wet.
Use foot powders and deodorants.
Choose breathable, well-ventilated shoes.
Choose shoes made with waterproof fabrics, like GORE-TEX. This fabric uses a membrane with pores small enough to block water but large enough to allow sweat vapor to escape. This creates a waterproof yet breathable barrier, keeping feet dry and comfortable.
Dry feet thoroughly with a towel after washing, especially between toes.
Avoid tight shoes that trap moisture.
Consider insoles with moisture-absorbing qualities.
Keep feet clean and dry before bed.
Perform Foot Inspections
At-home foot inspections are a good diabetic foot care measure in the winter (and in general) because they help identify potential issues like cuts, blisters, or signs of infection early, when they're easier to treat.
Check for cuts, blisters, or sores: Examine the entire surface of your feet for any visible signs of injury and skin perforation.
Look for changes in skin color or temperature: Check for any redness, swelling, or areas that feel unusually warm or cold.
Check your toenails and between toes: Look for ingrown toenails, cracked toenails and fungal infections,
Try Diabetic Socks
Compression stockings are a great way to enhance blood flow to the legs and feet, but they are not recommended for people with diabetes since they can do the opposite and restrict blood flow too much in the arteries. Instead, ask a podiatrist or chiropodist about diabetic socks and if they might work for you. They have several benefits, which are especially useful in the winter, including:
Antimicrobial treatment which prevents bacterial and fungal growth.
Slightly cushioned footbed for extra comfort and protection.
Loose, non-binding top band which rests comfortably around the ankles or calves, allowing more circulation.
Moisture-wicking and stretchy material.
Smooth toe area to prevent blisters and other skin irritation.
Choose the Right Footwear
https://www.youtube.com/shorts/R7GV0GbKhvQ
For diabetes patients, wearing proper footwear in the winter is essential for maintaining foot health.
Orthopedic shoes are an excellent choice, as they offer extra cushioning, arch support, depth, elasticity, adjustable straps and ample room to reduce pressure points and prevent blisters or sores.
High-quality winter footwear can also be effective, provided it offers warmth, water resistance, and moisture control properties to keep feet dry and comfortable. Here is what you should pay attention to:
Waterproof materials: As you already know, materials like GORE-TEX help maintain dryness by utilizing a membrane with microscopic pores. These pores are small enough to block water molecules, but large enough to allow vapor from sweat to escape. This technology effectively prevents external moisture, like snow or rain, from penetrating the footwear, keeping feet dry. The breathability of GORE-TEX also ensures that perspiration from the feet can escape, which prevents a buildup of moisture inside the shoe. This combination of waterproofing and breathability is essential for preventing cold and damp feet
Adequate insulation: This is crucial for maintaining warmth in winter footwear as insulation helps lock in warm air and retain body heat. Look for insulated winter shoes and boots that also let you maintain moisture control. And remember to let your feet air out after sweating in your boots all day to avoid excessive dampness.
Non-slip soles: For better traction on icy or slippery surfaces to avoid falls.
Cushioning and arch support: To provide comfort and reduce strain on the feet, especially when walking for extended periods.
Roomy toe box: To avoid friction and pressure on the toes, preventing blisters or sores.
Breathable lining: To allow moisture to escape and keep feet dry, reducing the risk of infections.
Adjustable closures: To ensure a secure fit without restricting circulation, particularly important for those with swelling or neuropathy.
In addition, custom orthotics can provide personalized support, improving foot alignment and alleviating pressure, further reducing the risk of diabetic foot complications.
Visit a Foot Specialist
https://www.youtube.com/shorts/qR3s05lUwyc
Our top tip for managing diabetic feet in winter? Book an appointment with a foot care provider, like a podiatrist or chiropodist, at a foot clinic.
At Feet First Clinic, our chiropodists are trained to:
Offer comprehensive education on how cold weather can affect diabetic feet.
Provide skin and nail care.
Provide wound care.
Offer custom orthotics services: assessments, casting, fittings and follow-up guidance.
Thoroughly inspect your feet and pinpoint potential issues (this can be difficult to fully achieve at home, since diabetes also affects eyesight).
Help you understand what winter boots or shoes you should wear, which you can then browse for at our store. A member of our staff can guide you through our options with a complimentary shoe fitting.
Discuss the benefits of products like diabetic socks, orthopedic slippers, moisturizers, and more, which you can then purchase at our store.
Contact our Toronto foot clinic to learn how a foot assessment can be your first step toward healthier, happier feet this winter!
November 28, 2024
Whether caused by an injury, circulation problems, or a chronic condition, foot and ankle swelling shouldn't be ignored. In this blog, we'll explore potential causes of swelling, when it might be a sign of something more serious, and how seeing a foot specialist at a Toronto foot clinic can help you get back on your feet.
What is Foot Swelling?
https://www.youtube.com/shorts/dFZVG-2ymxY
The medical term for foot and ankle swelling is called edema. This term can also be used for swelling in other body parts. It is an accumulation of fluid leaking from small blood vessels into the tissues of the foot and ankle. This causes the area to appear puffy or enlarged.
Swelling in the feet often occurs because of circulation issues, injuries, infections, or underlying health conditions. The lower extremities are especially vulnerable to swelling because gravity naturally pulls fluids downwards.
The body’s circulatory and lymphatic systems typically manage this fluid, but when they’re not functioning optimally, fluid retention can occur. Your body’s inflamatory response to foot and ankle injuries, hormonal changes (pregnancy, etc.) and increased blood volume can also lead to swelling.
Edema in the feet can range from a mild inconvenience to extremely distressing and debilitating. It can affect your gait pattern (the way you walk), make buying shoes that fit almost impossible, and coincide with other uncomfortable symptoms. You shouldn’t ignore foot and ankle swelling, even if you think you know the cause. This is because:
It can get progressively worse
It can signal a health condition you weren’t aware you had
It can be a sign that a foot injury is more serious than you thought
It can lead to other complications
It may require prompt treatment
Causes of Swollen Feet and Ankles
There are numerous causes of swollen feet and ankles. Some are mild and going away over time, while others are more severe and debilitating and may require consistent assessments and check-ups with either a physician or a foot specialist, like a chiropodist or podiatrist. If you notice swelling within your feet that is new then discuss with with you physician. Common causes of foot and ankle swelling include:
Injury. Sprains, fractures, and strains can cause localized swelling due to inflammation in the injured tissues. To protect yourself, check out the best ways to prevent foot injuries.
Infections. Conditions like cellulitis, a bacterial skin infection, can lead to swelling, redness, and warmth in the affected area.
Venous insufficiency. This is a term for damaged vein valves and in some circumstances be caused by deep vein thrombosis (DVT) or malformation in the leg veins. General venous insufficiency is common especially as we age. Poor blood flow from the legs back to the heart causes fluid buildup, leading to swelling in the lower legs and feet.
Lymphedema. Blocked or damaged lymphatic vessels prevent fluid drainage, causing chronic swelling, often in one leg or foot.
Heart, kidney, or liver disease. These conditions can disrupt fluid balance in the body, leading to retention in the feet and ankles.
Pregnancy: Increased blood volume and pressure from the growing uterus can cause fluid accumulation, especially in the lower extremities.
Prolonged standing or sitting. Sitting in one position OR standing for extended periods can cause fluid to pool in the legs and feet due to gravity. Office workers, restaurant servers, cooks, flight attendants, and more can experience mild swelling simply due to their occupation.
Gout. Gout is a type of arthritis caused by high levels of uric acid in the blood, leading to the formation of urate crystals in joints. The result is intense burning pain, redness, and swelling, particularly in the big toe. Improving your diet may be able to help with flair ups.
Diabetes: The top of the feet and ankles can swell due to nerve damage caused by diabetic neuropathy.
Diet. High sodium diets can cause excessive swelling in the legs.
Signs Your Swollen Feet and Ankles May be Serious
https://www.youtube.com/shorts/dD0T2wUUFdQ
Below are some coinciding symptoms that may be tell-tale sign of a health condition. As always, if anything is new, then to see your physician rather than to leave it:
Burning sensation. Persistent burning in the feet along with swelling could indicate nerve damage.
Redness and warmth. Swelling accompanied by redness, warmth, and tenderness may signal an infection, such as cellulitis, that needs attention.
Sudden onset of swelling. Rapid or sudden swelling in one leg could indicate a blood clot or deep vein thrombosis (DVT)s. This condition requires urgent care.
Pain: Severe pain along with swelling, especially after an injury, may point to a fracture or ligament damage.
Swelling in one foot only: Sometimes localized issues can indicate a more severe and specific problem.
Shortness of breath or chest pain. These symptoms can indicate heart or lung issues, like congestive heart failure, and requires immediate medical help.
Skin Changes: Discolored, tight, or shiny skin over swollen areas may suggest lymphatic or circulatory issues needing evaluation. Red toes or dark blue skin can signify peripheral artery disease, coronary heart disease, high blood pressure and more.
Persistent or worsening swelling. Swelling that doesn’t improve or worsens over time could be a sign of an underlying health condition that needs treatment.
When to See a Podiatrist or Chiropodist: Treatment
https://www.youtube.com/shorts/IryRcL4JPjI
You should always see a physician or foot specialist if you’re experiencing discomfort in any capacity. Remember: foot issues are not “normal.”
Because foot and ankle swelling is usually caused by an underlying medical condition, you should first see your family doctor. They can refer you to the appropriate specialists and run the necessary testing to determine what is causing the swelling. Your treatment options may target edema directly, or they may target the underlying health condition.
Once you determine the underlying cause of the foot swelling, a foot specialist or foot clinic can provide solutions to manage and accommodate the condition, so you can live your life as comfortably as possible. Below are some services a foot clinic can offer to help foot and ankle swelling:
Compression Socks
Compression stockings are a great option for venous insufficiency, pregnancy, fatigue-related swelling, and sometimes even underlying health conditions like lymphadema. They reduce swelling by promoting blood flow and limiting fluid buildup in the lower extremities. A common myth is that they are clunky, noticeable medical devices that clash with your clothing, but they are actually quite fashionable and sleek. Most people will not even realize you are wearing them.
You can get standard knee-high socks or even pantyhose, depending on how your activities and how you want to dress them up. You can get a prescription from a physician, and then stop by our Toronto foot clinic, where our certified fitters can measure you and help you select the best stockings for you.
As compression stockings can be contraindicated for some conditions (like diabetes and periphery artery disease), it's strongly recommended that you first visit discuss compression stockings with your family doctor if you have any underlying health concerns.
Orthopedic Footwear
Orthopedic shoes can accommodate swelling by offering several key features designed to provide comfort and support:
Adjustable straps and laces. Many orthopedic shoes come with adjustable fastenings that allow for a customizable fit, accommodating changes in foot size due to swelling.
Wide toe boxes. These shoes often have a wider, more spacious toe area, which helps to prevent pressure on swollen feet and allows room for expansion.
Elastic materials. Some orthopedic shoes are made with elastic or stretchable fabrics, allowing them to gently conform to the shape of the foot and adjust to fluctuations in swelling throughout the day.
Extra depth. Orthopedic shoes often have a deeper design, providing more room for foot swelling and preventing tightness that could worsen discomfort.
By combining these features, orthopedic shoes can help manage swelling while providing the support needed for optimal foot health.
Diabetic Foot Care
https://www.youtube.com/shorts/4P3UiDSFzr4
If your edema is caused by diabetic neuropathy or periphery artery disease, diabetic foot care at a foot clinic should be a part of your monthly routine. At a diabetic foot care appointment, your chiropodist will monitor your foot health. They'll examine your feet to check for sensation, circulation, and check for any potential causes for concerns - like disease progression and worsening circulation issues. Routine diabetic foot care also involves wound and nail care, diabetic foot education, and more. While these practices don’t directly target swelling, they are all interconnected and help reduce the risk of complications that can worsen swelling.
Biomechanical Assessment
If your swelling coincides with an injury and other chronic foot pain, a biomechanical assessment and gait analysis with a chiropodist can help. A chiropodist can then diagnose any underlying muscular or biomechanical issues that are causing or contributing to the foot pain, and make treatment recommendations like custom orthotics.
Additional Swollen Foot and Ankle Treatments
RICE Method
The RICE method is an acronym for a popular at-home treatment routine for acute foot injuries: rest (avoiding activities that strain the foot), ice (applying cold packs to reduce swelling and pain), compression (using bandages, tape, compression socks, and more to limit swelling), and elevation (raising the foot above heart level to help drain excess fluid). If you're
Treatments That Target Underlying Health Conditions
When foot swelling is linked to serious underlying health conditions, treatments aim to address the root cause and prevent further complications.
For example, conditions like heart failure, managing the condition with medications can help reduce fluid retention and ease swelling. In cases of kidney disease, doctors may adjust medications and recommend dietary changes to help the kidneys function more effectively, reducing the build-up of excess fluid in the body.
In some lymphatic conditions, such as lymphedema, may be treated with specialized therapy, including manual lymph drainage to help encourage the movement of fluid away from the swollen areas. Compression therapy is also helpful for lymph conditions.
Each treatment is tailored to the specific health condition causing the swelling, and addressing the underlying issue can significantly reduce or even prevent the recurrence of swelling. Regular monitoring and early intervention are key to managing these conditions effectively.
https://youtube.com/shorts/2mS-9D7LHq4?si=bOOBryZI6ne5VrtP