May 21, 2026
Nothing will dampen your spirits during a beautiful summer like a foot infection. You won’t feel like taking a long stroll by the beach when you have a painful plantar wart on your sole. You won’t want to head to a pool party when you have a bad toenail fungus. And you won’t want to go for a hike through a national park when the itch of your athlete’s foot is driving you up the wall.
If you don’t want to deal with a foot infection for the entire season, you should follow these simple rules:
1. Don’t Go Barefoot at the Pool
The best method of prevention of foot problems in the summer is to cover up your feet with high-quality shoes because the ground is covered with bacteria, fungi and viruses that can infect your feet. Areas that are warm, wet and have lots of visitors will be especially risky. So, you should sport protective footwear when you’re walking across the deck of the community swimming pool or using the locker room showers at the gym.
Get a pair of waterproof shoes that you can wear to the swimming pool deck, public showers and locker room. After every use, you should rinse your shoes with warm water and dry them. You should also start washing your feet and drying them with a towel after going to these locations in case any contaminants got onto your feet. Then, put on a clean pair of socks and outdoor shoes.
2. Don’t Go Barefoot at Home
You should break the habit of walking around barefoot, even at home. Other residents in your home could unknowingly transfer a contagious infection like athlete’s foot to the floor that you’re walking on every day. Wearing a pair of comfortable slippers or socks will protect your feet and prevent a frustrating cycle of infection.
3. Change Your Shoes and Socks Often
You should change your shoes and socks often if you want to avoid problems like toenail fungus and athlete’s foot. As previously stated, bacteria and fungus thrive in warm, moist conditions — this includes inside of your sweaty shoes and socks.
Whenever your socks get sweaty, change them and put on a cleaner pair. Don’t wear one pair of shoes every single day, especially if you’re exercising in them. Give them a chance to air out.
If your shoes are starting to smell like foot odour, let them dry in the sunshine to kill off the bacteria. You may also want to try an antibacterial foot and shoe deodorant spray. In addition to killing bacteria, some products also contain mild anti-fungal properties, which are great for preventing fungal growth in your footwear.
4. Don’t Share Your Shoes
Do you remember being told never to share hats in school because one of the other children could have lice and give it to you? You should give your shoes a similar treatment because sharing shoes with other people puts you at risks of contracting a toenail fungal infection or a bad case of athlete’s foot. Keep your shoes, boots, inserts, socks and everything else you put on your feet to yourself.
When you follow these essential rules, your feet will stay healthy and infection-free all summer long. You can go back to enjoying your favourite activities, whether it’s going for a walk through the neighbourhood park or taking a quick dip in the community swimming pool.
5. Moisturize Your Feet
There's good kinds of moisture, and bad kinds of moisture. The moisture from sweat-buildup on the feet would be considered "bad" because it causes bacteria buildup, which can lead to foot odour and infection. However, if the skin on your feet is too dry, they can get small cracks. These cracks are an open portal for fungus and bacteria to penetrate and set up shop - that's how infections start. That's why it's important to moisturize your feet daily with a foot cream. Moisturizing strengthens your skin barrier, which will prevent cracks that can form due to dehydration.
6. Avoid Shellac
Many people like to sport a nice pedicure to show off their feet during the summer. When doing so, it's recommended to avoid shellac. Shellac traps in moisture, which allows fungus to thrive. Even worse, you won't even know you have toenail fungus until you remove the shellac (and given how long shellac lasts, that could give the fungal infection a big head start). Instead, opt for regular nail polish and remove it regularly so you can inspect and monitor for any potential infection.
7. Avoid Pedicures at Salons
Did you know nail salons are one of the top breeding grounds for fungal infections? Fungal infections are relatively common at nail salons because the warm, moist environment and shared tools can allow fungi to spread if strict hygiene practices are not followed. Instruments such as nail clippers, files, and cuticle pushers can transmit fungi between clients if they are not properly sterilized, potentially leading to infections like Onychomycosis. Pedicure foot baths can also harbor microorganisms when they are not thoroughly disinfected between uses. Additionally, aggressive cuticle trimming or minor skin injuries during a pedicure can create small openings that allow fungi to enter the skin, increasing the risk of infections such as Athlete's Foot.
Instead, to keep your feet and toenails in tiptop shape, opt for a medical pedicure. A medical pedicure at a foot clinic is performed by a licensed chiropodist using equipment and tools sterilized according to Health Canada standards and regulated by both Health Canada and the College of Chiropodists of Ontario. This ensures the risk of infection is practically eliminated, while giving you the added benefit of having a professional monitor your overall foot health.
April 9, 2026
There are several reasons why your toe may be painful. The important thing to do is not ignore it, especially if the pain is accompanied with redness and swelling. Keep reading to find out what your next steps should be to find out the culprit to your pain.
1. Ingrown toenail
An ingrown toenail is when the sides of your toenail grow into the surrounding skin. Once the nail pierces the skin, your body reacts by creating an inflammatory response to this, which leads to redness, swelling, warmth, and pain in the area. The longer the toe is left in this condition, the higher the risk of infection. How can you tell if you have an infection? The signs of an infection are somewhat similar to those of the body’s natural inflammatory response to a cut or wound, but greater in a sense. For instance, an infected ingrown toenail will increase in redness, swelling, pain, and warmth in addition to being accompanied by any of the following: a foul odor, maceration (moisture), pus (cloudy, creamy liquid), blood.
If you have an ingrown toenail, it is best to see a chiropodist for treatment - especially if it's showing signs of infection. A chiropodist can remove the ingrown portion of the toenail, prescribe antibiotics, and properly trim and file the toenails to ensure they grow back healthy. To find out more about ingrown toenails, such as what causes them and how they can be managed, click the link here.
2. Paronychia
Paronychia is the medical term to describe an infection of the hand or the foot at the location where the skin meets the nail, either on the sides of the nail or along its base. This infection can be bacterial or fungal in nature and is usually the result of damage to the skin (via biting or picking or any other physical trauma). Excessive and chronic moisture can also make the skin more vulnerable to these infections.
Similar to an ingrown toenail, paronychia will also present as a red, swollen, warm, and tender digit. If you have a red, swollen, painful toe, regardless of the cause, book an appointment with a chiropodist at the first signs! They'll be able to properly diagnose and treat the condition.
3. Tinea Pedis
Although Tinea pedis also known as Athlete’s Foot, usually presents as itchy, dry, and flaky skin on the bottom of the foot, it can also be localized between the digits or along the sides of a single or multiple digit(s). Sometimes, Tinea Pedis features a cluster of small red vesicles along a digit and may spread to adjacent digits. When left untreated, the toe may become red, swollen, and tender to the touch. The infection can also spread under the toenail. When this happens, treatment can become very difficult and take a long time to resolve.
Fungal infections can spread very quickly, and the earlier you start treatment, the easier it is to treat. Therefore it's best to be proactive and see a professional at the first signs of infection. Treatment includes a topical prescription antifungal medication and debriding the areas of fungal growth. Fungal infections most often cannot be treated without professional intervention, and over-the-counter treatments rarely work.
4. Onychophosis
Onychophosis is a buildup of callus that forms between the nail and the surrounding skin (sulcus). It can become irritated and mimic the discomfort of an ingrown nail due to pressure, but it’s not a true ingrown nail—the nail itself remains healthy and does not grow into the skin.
5. Reynaud's Disease
This condition causes toes to turn stark white and then bright red, often after moving from a cold environment to a warm one. While usually asymptomatic, it can cause numbness, tingling, and alarm due to the dramatic color changes. It’s a vasospastic response, where the blood vessels temporarily spasm and restrict proper blood flow.
6. Chilblains
These are small, painful, or itchy bumps that develop on the toes after exposure to extreme cold followed by rapid warming. They are usually harmless and tend to resolve on their own within a few weeks.
All the above conditions require medical attention. In the meantime, as you wait for your appointment, try soaking your feet in an Epsom salt water bath for 10-15 minutes a day. Use half a cup of Epsom salts to a gallon of lukewarm water - not hot as hot water will cause more swelling.
When you’re not soaking your feet, practice good hygiene and keep your feet clean and dry. Wear a new pair of clean socks everyday and let your feet breathe at home. Most microorganisms thrive in moist, dark environments.
February 5, 2026
If you are like most people, you want your feet to stay healthy and pain free. However, even with the best intentions, many people unknowingly develop habits that can damage their feet over time.
From improper nail trimming to walking barefoot in public spaces, foot care mistakes are more common than you might think. The good news is that most of these issues can be prevented with proper education and routine care.
Below, our team of experienced chiropodists at Feet First Clinic outlines the top five most common foot care mistakes and how to avoid them. We specialize in preventive foot care and the treatment of both common and complex conditions, offering services such as routine care, assessments, and custom orthotics.
1. Cutting Your Toenails Incorrectly
Toenail trimming may seem simple, but doing it improperly can lead to painful ingrown toenails and infections. Cutting nails too short, rounding the edges, or cutting into the cuticle increases the risk of the nail growing into the surrounding skin.
To reduce this risk, soften your nails by soaking them in warm water before trimming. Always cut straight across and avoid cutting too close to the skin. If you develop a painful or infected ingrown toenail, it is important to seek professional care promptly.
Another common mistake when it comes to ingrown toenails: trying to treat them yourself or at a salon. Some of the worst ingrown toenails we've seen at the clinic are due to botched DIY attempts. If your toenail is ingrown, especially if it's irritated, it's recommended that you book an appointment immediately with a chiropodist; they're trained to treat ingrown toenails properly and prevent them from getting worse. A chiropodist will also trim your toenails so that they grow back properly and straight.
2. Walking Barefoot in Damp Areas
Many people walk barefoot in public locker rooms and showers. Although this may not seem like a huge issue to some people, doing this can seriously harm your feet. It's recommended to wear some sort of protective footwear while you’re walking in moist areas.
Some examples of reliable footwear include:
Sandals
Flip-flops (just for those public spaces)
Water shoes
Shower shoes
Doing this is important for preventing issues like toenail fungus. This will cause your nails to become yellow, thick and foul-smelling; they may even fall off! Men tend to have a higher chance of developing foot fungus, along with elderly people and individuals that suffer from athlete’s foot. Once fungus gets underneath the toenail, it becomes very difficult to treat; at-home treatment is typically ineffective. This is because the toenail blocks anti-fungal medication from penetrating and reaching the fungus. That's why it's important to see a chiropodist at the first sign of toenail fungus. They can debride the toenail to make it easier for anti-fungal medication to penetrate to the fungus living in the nailbed.
Walking barefoot in public places can also cause warts. Warts are a contagious virus that spreads when bare skin comes into contact with an infected surface. The wart-causing virus especially thrives in warm, damp places, like locker room floors and the puddles on pool decks. Left untreated, warts can multiply and spread to other people. Sometimes you can treat warts in the early stages with over-the-counter treatments. However, if those are ineffective, it's recommended to see a chiropodist to eradicate your warts once and for all. Unlike family doctors and dermatologists, chiropodists can debride the dead skin and callus that forms over the wart, which helps the treatment penetrate through the wart tissue and treat the warts faster.
3. Ignoring Early Signs of Foot Problems
Many people dismiss early symptoms such as redness, thickened nails, calluses, or mild discomfort. Unfortunately, delaying treatment often allows minor issues to develop into more serious foot conditions.
Addressing concerns early can prevent pain, reduce complications, and keep your feet healthy long term.
4. Wearing Poorly Fitting Footwear
Did you know that between 63% to 72% of the population are wearing shoes that don't fit correctly? Shoes that are too tight, too loose, or lacking proper support can contribute to problems such as blisters, corns, bunions, and heel pain. While style may be important, proper fit and support should always be the priority.
Well fitted footwear helps support proper foot function and reduces strain on the feet, ankles, knees, and lower back. It's also important to make sure your shoes accommodate your foot type and gait pattern. If you don't know your foot type, you can get a biomechanical assessment with a chiropodist to find out.
5. Skipping Preventive Foot Care
Many people only think about foot care when pain develops. Regular foot assessments, proper hygiene, and preventive treatment are essential for maintaining healthy feet, especially for individuals with diabetes or circulation concerns.
Routine visits to a chiropodist can help identify potential problems early and keep your feet comfortable and functional. Something as simple as a medical pedicure can go a long way.
October 28, 2024
Taking care of your feet during winter might require a little extra effort, but it’s essential for preventing discomfort and long-term issues. The cold weather can impact your feet in its own unique ways, just like hot weather can. Whether you’re dealing with dry, cracked skin or trying to avoid slippery conditions, being mindful of your foot health will keep you a step ahead of the cold.
5 Ways Cold and Wet Weather Can Impact Your Feet
Dry, cracked skin
Skin conditions
Reduced circulation
Stiffness and joint pain
Winter-related foot conditions
1. Dry, Cracked Skin
https://www.youtube.com/watch?v=1-Sf43woLLE
One of the first things you may notice during the winter is dry, cracked skin on your feet, especially your heels.
The chilly air and low humidity can quickly sap the moisture from your skin, leaving your feet feeling rough and sore. Heating indoors doesn’t help either, as it dries out the air, exacerbating the issue.
This is where cold weather foot care enters the picture! Since cracked skin can cause pain and even bleed, it becomes essential to protect your feet. This dryness isn’t just unsightly—if the cracks open up, it creates an easy pathway for infections. This can lead to debilitating pain and bleeding that makes walking difficult.
Regular moisturizing with a medical-grade foot cream is a straightforward way to combat dry feet and cracked heels. Look for products that contains a high urea concentration, which will help your skin replenish and retain lost moisture. It's important to use a foot cream instead of a regular moisturizer for your feet because the skin on your feet is thicker than the skin elsewhere on our body. Therefore, a regular body or facial moisturizer won't cut it - especially during the dry, colder months.
While you're at it, take your hydration to the next level by always remembering to drink your eight glasses of water per day. This advice still holds up today!
2. Reduced Circulation
Cold weather can mess with your blood flow, which can pose a problematic obstacle for foot health. When temperatures drop, blood vessels constrict to preserve heat, meaning less blood flows to your extremities. This is called vasoconstriction.
As a result, your feet may feel cold, numb, or even tingly. Poor circulation can also lead to prolonged healing times for cuts or blisters. This is concerning for diabetes patients with neuropathy who are already struggling with wound healing issues. That's why cold weather diabetic foot care should always include steps to monitor and improve blood flow— including daily foot inspections and easy foot exercises.
Wearing thermal socks and ensuring your feet are properly insulated can help combat the impact of reduced circulation. Just make sure your thermal socks fit comfortably with your fall and winter footwear: if your shoes or boots are too tight, it will reduce circulation and make your feet more susceptible to cold-weather complications (more on that below).
If you experience slippery conditions during winter, circulation issues can also increase your risk of falling or slipping. When your feet are numb, it’s harder to get a good sense of balance, so be cautious and wear shoes with good grip for FALL prevention.
Moving around can also help keep your blood flowing. So, if you’re out and about, take small breaks to wiggle your toes and stretch to maintain circulation. There are even targeted foot exercises you can try to help trigger healthy blood flow. In fact, you should do these more often in the winter than the summer.
3. Skin Conditions
https://www.youtube.com/shorts/xZ4RQwPmCzg
It might seem strange to consider blisters a winter problem, but they can definitely crop up due to cold weather foot care challenges.
Wearing heavy boots and thick socks can cause friction, leading to blisters on your heels or toes. This is why it’s extremely important for boots to fit snugly, but not be too tight. So if the socks you like to wear in the winter are causing your boots to constrict your feet, they don’t fit!
And if your feet are already dry, cracked, or dealing with reduced circulation, they’re even more susceptible to developing painful blisters. Combat this by ensuring your boots and sock combo always fit perfectly together, and opt for moisture wicking socks to go the extra mile.
Another common winter foot problem is athlete's foot. Though often associated with the hot summer months and public swimming pools, athlete's foot is no stranger to winter either. Athlete's foot thrives in wet, damp areas, so instead of crowded public summer pools, fungal infections change their habitat to the wet-from-the-snow environment inside your boots. And keep in mind, you can get athlete’s foot simply by coming into contact with someone who already has it.
When you’re tackling wet feet, whether it’s from snow or rain, you need to dry them thoroughly before putting on warm socks. Athlete’s foot loves moist environments, so making sure your feet are dry is key. If you start to notice itchy or peeling skin between your toes, it’s a sign that athlete's foot might be setting in. Treat it promptly with your Toronto chiropodist, who can provide the right antifungal products. Make sure you also keep your feet clean and dry and avoid sharing shoes and socks to protect your feet from a future infection.
4. Stiffness and Joint Pain
https://www.youtube.com/shorts/n46k32OZgco
Cold weather tightens your muscles, which in turn can lead to stiff joints. This discomfort can be particularly noticeable if you already have arthritis or any other joint-related issues. Without the right cold weather foot care, your feet can end up feeling stiff, which can affect your overall mobility. To help counteract this, regular stretching and low-impact exercises, such as foot rotations, can keep your joints limber.
This season also requires some extra attention to footwear. Choose shoes with ample support to keep your feet cushioned against the impact of walking on hard, cold surfaces. Slippery conditions can further aggravate joint pain because your body works overtime to stay balanced, putting extra pressure on your feet. Adding orthotics or insoles that provide added arch support can also reduce some of this strain and make your steps feel more cushioned and less jarring.
5. Winter Related Foot Conditions
Winter brings its own set of unique foot problems, including chilblains, frostbite, and Raynaud’s disease, all of which can make cold weather foot care a bit trickier.
Chilblains occur when your feet are exposed to cold, damp environments, causing painful, itchy red patches. This is particularly common in teenagers, or people who quickly reheat their feet after being in the cold, so it’s best to warm up slowly.
Frostbite is another concern in extreme cold, as it can severely damage your skin and tissues. Frostbite can occur more quickly than you might expect, especially if you don't protect your feet from the weather. Signs of frostbite include numbness, skin discolouration, and a hard, waxy texture. If you think you may be experiencing frostbite, it’s essential to seek medical help immediately. To prevent frostbite, be sure to layer up and wear weatherproof boots that keep your feet dry and warm.
Lastly, Raynaud’s disease can be exacerbated by cold weather. People with Raynaud’s experience an exaggerated response to cold, which restricts blood flow to the toes, leading to reduced circulation and making your feet even more vulnerable. Keeping your feet constantly warm and avoiding sudden temperature changes can help manage Raynaud’s symptoms, but if you experience persistent pain or numbness, you should consult a healthcare provider.
October 24, 2024
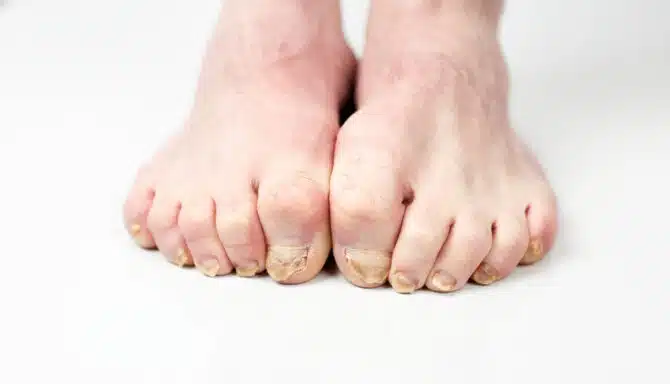
There are two common fungal infections that can target your feet. For your skin, it’s athlete’s foot (tinea pedis), and for your nails, it’s fungal toenail (onychomycosis). Fun fact: Onychomycosis is the name for nail anatomy changes caused by contagious fungus, while dystrophic is the term for any other abnormalities that affect how your nails look or grow. Today’s blog will focus solely on toenail fungus. You’ll learn what it is and how to treat it, as well as some top fungal toenail prevention tips recommended by our Toronto chiropodists.
Toenail Fungus Symptoms
Sometimes toenail fungus is mild and barely noticeable. But fungal toenail can present more severely if you’re immunocompromised, such as if you have diabetes, or a senior. Keep an eye out for these common symptoms:
Drastic changes in the nail’s appearance: it can look much thicker, have a yellowish, brown colour, and be very brittle and prone to cracks, despite thickening.
Unpleasant odour coming from the nail: the smell is often reported to be sour or like cheese.
The nail starts lifting off the nail bed: this is because debris starts to accumulate and lifts the nail up so it can’t reattach.
Pain, swelling and bleeding in severe cases.
Toenail Fungus Prevention: Foot Specialist Advice
The most important fact to remember about fungal toenail is that it’s contagious. Since fungal infections spread easily in damp, shared spaces like pools, gyms, and shower rooms, the best defense is keeping your feet clean and protected! Here are some top, Toronto-chiropodist-recommended tips to remember:
Follow a strict, yet fun and relaxing, foot hygiene routine. It’s a part of self care, after all!
Wear breathable footwear. Opt for shoes made from materials that allow airflow to keep your feet dry.
Change socks daily. Fresh socks prevent moisture buildup, which fungi love.
Avoid going barefoot in public places. Use flip-flops or shower shoes to protect your feet in shared spaces.
Keep your toenails trimmed and clean. Regular maintenance helps prevent infections from taking hold. Get a professional medical pedicure if you don’t have time to focus on nail care.
How to Treat Toenail Fungus
Once fungus has gotten a hold of your nails, it’s time to think about treatment and eradicating the problem. Unfortunately, you can’t do much to treat toenail fungus yourself at home, and you often need a chiropodist’s help. Luckily, treatments are easy to follow and non-invasive. Here’s what a foot specialist can do:
Perform nail debridement to remove infected parts of the nail.
Use prescription-strength topical antifungal medicine on the nail (it penetrates the actual fungus)
Educate you on products you can use going forward to prevent re-infection, like the best moisture-wicking socks, shoes, foot creams, deodorants and more.
October 10, 2024
Toronto's summer is behind us and the warm days of sandals won’t return until next year. But fall brings its own charm and many folks are excited for a new chapter. At the same time, you may also be looking to prevent foot issues this fall in as many ways as possible, and luckily, you’ve come to the right place! For top tips on blisters and dry skin prevention, as well as how you can fight some other common fall foot problems, keep reading today’s article!
Cracked Heels
As summer’s humid air is replaced with dryness, the skin on your feet may dehydrate and over time, cracked heels can form.
One of the best fall foot care tips to prevent this is regular moisturizing. Use a nutrient-dense product like Gehwol’s Lipidro Cream, available at Toronto’s Feet First Clinic.
It helps lock in moisture and prevent further damage. Containing high-quality ingredients like avocado oil and urea, this cream helps your skin absorb water into its layers and supplies dry skin with the lipids it needs. Properties like allantoin can also soothe irritation sometimes associated with cracked heels.
Fungal Infections
You may have heard how fungal infections like athlete’s foot are easy to contract during the summertime. Public pools, shared locker rooms and showers, and other communal spaces are all summer hot spots where this foot fungus can breed. But did you know that foot fungi is still a threat in the fall?
It can thrive when people wear closed shoes for longer periods, trapping moisture and warmth. To prevent this, keep feet clean and dry, wear breathable socks, and choose shoes that allow proper ventilation. Shoes should also be waterproof to prevent extra water getting into your shoe’s environment. To find the right pair for fall, visit your local Toronto foot clinic for a shoe fitting.
While you’re at it, learn all about the best foot hygiene here!
Musculoskeletal Foot Conditions
Musculoskeletal foot conditions can flare up as the fall chill starts to bite, making each step feel a little extra uncomfortable.
Cold temperatures cause the tissues in your joints to contract, putting pressure on nerve endings and leading to more foot pain and aggravated osteoarthritis. The cold can also worsen foot conditions like plantar fasciitis and other sources of arch and heel pain.
Get ahead of this issue by wearing boots with solid insulation that traps warmth. Also, keep your feet extra cozy with warm socks — a Toronto chiropodist may even suggest a pair of compression stockings (like Sigvaris' Thermoregulating Wool or Merino Wool compression stockings).
Blisters
Autumn foot health often involves managing painful blisters. As new footwear makes its debut, a tight squeeze can slowly wreak havoc and cause discomfort.
To keep your feet happy and blisters at bay, make sure your shoes fit securely and snugly (but not tight!) to prevent excessive friction rubbing against your skin. Wear your boots with other products like moisture control socks, foot powders, blister bandages and insoles to prevent this frustrating issue.