December 11, 2025
Our feet are pretty amazing structures.
With over 52 bones, over 250,000 glands and nerves, they're certainly a complex parts of our bodies, and so they deserve a dedicated specialist to keep them in peak condition. How exactly do these specialists work? And why might you need to see one? Read on and find out.
What's A Chiropodist?
A Chiropodist (pronounced "kerr-op-o-dist") works to support the prevention and management of acute and chronic conditions that affect our feet and lower limbs. Think: skin conditions like warts and calluses, nail conditions like ingrowns or fungus, and musculoskeletal conditions like Plantar Fasciitis and Gout. These are just a few examples of the foot conditions a chiropodist can treat. Click to learn more about other Common Foot Conditions.
Is a Chiropodist Different than a Podiatrist?
It depends on where you live.
ChatGPT said:
In Ontario, both chiropodists and podiatrists are regulated foot care professionals, but their training and scope of practice differ slightly. Chiropodists are the most commonly licensed foot specialists in the province and provide comprehensive care including assessments, routine and advanced treatments, custom orthotics, minor procedures, and certain injections. Podiatrists are less common and were grandfathered into practice prior to 1993, when Ontario transitioned to licensing only chiropodists. A podiatrist can perform bone surgeries like bunion or hammertoe corrections, whereas a chiropodist cannot (they can still do other surgeries). Regardless of the title, both professionals are highly qualified to help you manage foot pain and keep you moving comfortably.
What Do Chiropodists Check For?
When a chiropodist sits down to assesses your feet, they'll be able to spot and treat minor problems right away, like hard skin, Warts, and Ingrown Toenails.
For people with diabetes, the chiropodist will check the sensation and circulation in the feet, as well as examine the feet for any potential irregularities or cause for concern. If you have foot pain, a chiropodist can do a biomechanical assessment and gait analysis. They'll check your alignment when you walk, and will then be able to recommend or prescribe solutions including, but not limited to, Orthotics or Insoles, to get the feet working in peak condition. Either way, you'll leave your first visit knowing your feet are being properly cared for.
As you can see, foot health isn't just about feet! When feet are in good condition, the whole body can be properly supported. When they're not, you'll likely notice problems elsewhere. Foot health is every bit as much about your legs, hips, and spine as it is about the way your toes look in sandals. Chiropodists are trained to see the bigger picture of your physical health and the role your feet play in it.
Even if you don't have foot pain, we urge you to visit a chiropodist. Your feet, after all, are your body's foundation, and having them assessed could save you aches and pains later on. Foot problems affect well over half the population. Don't be one of those people who finds themselves at risk of long-term consequences.
April 17, 2025
If you're wondering why your plantar warts keep returning, you're not alone. But the good news is, you have options! Today’s article delves into the reasons behind recurrent plantar warts and effective prevention and treatment strategies. Keep reading to learn more!
What is a Plantar Wart?
A plantar wart is a non-cancerous skin growth that appears on the soles of the feet, caused by specific strains of the human papillomavirus (HPV), notably types 1, 2, 4, 60, and 63. The virus infiltrates the skin through tiny cuts or abrasions, often occurring in communal areas like public showers or swimming pools where the virus thrives. This is also the same type of communal environment that breeds athlete’s foot and fungal toenail, although those are fungal infections and not caused by HPV.
Once inside, HPV infects the basal layer of the epidermis, leading to the proliferation of keratinocytes and the formation of a wart. Due to the pressure from walking or standing, plantar warts often grow inward beneath a hard, thick layer of skin, which can cause discomfort or pain during weight-bearing activities.
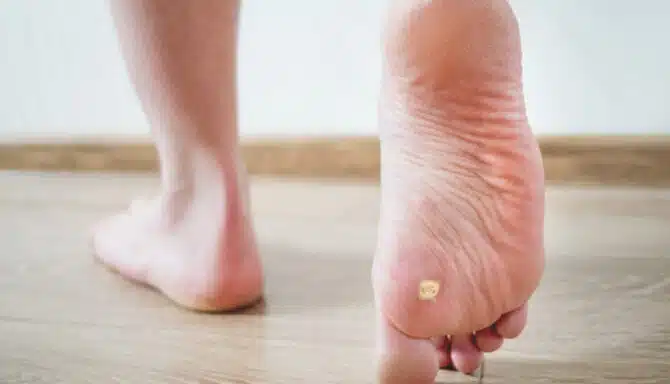
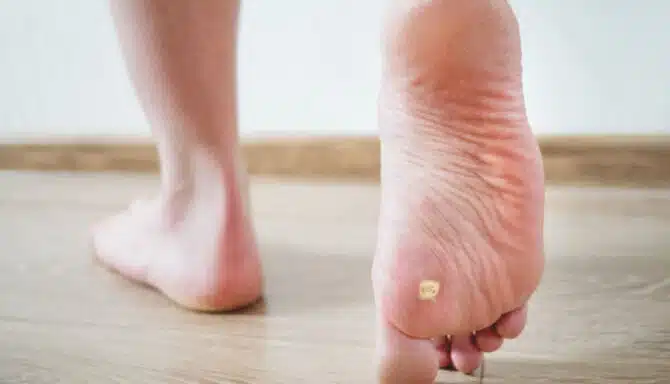
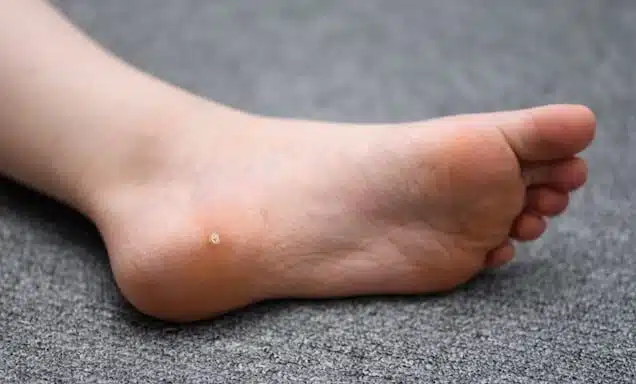
Plantar warts are characterized by their rough, grainy appearance and may have small black dots on the surface, which are thrombosed capillaries. They can occur as solitary lesions or in clusters known as mosaic warts. The body's immune response to the virus varies, and in some cases, the wart may persist for months or even years without treatment.
Plantar warts can sometimes look like other skin conditions, namely corns. Differentiating between them is essential, as their treatments differ. While both can appear as thickened skin on the foot, corns are caused by repeated friction or pressure, leading to a buildup of dead skin cells. Depending on the type, corns have a hard center and are surrounded by inflamed skin. In contrast, plantar warts are viral in origin. Additionally, warts may bleed when the surface is pared down, revealing pinpoint bleeding, whereas corns do not.
Plantar Warts: Risk Factors and Symptoms
In addition to walking barefoot in communal high-risk areas (i.e.: locker rooms, pool decks, etc.), there are other risk factors for plantar warts worth noting.
Risk Factors
Weakened immune system: Individuals with compromised immunity, such as those with HIV or undergoing immunosuppressive therapy, are more prone to infections.
History of plantar warts: Previous occurrences can indicate a higher likelihood of recurrence.
Children and teenagers: Younger individuals are more susceptible due to their developing immune systems, and they may spend more time in communal areas like gyms, pools, and locker rooms.
Excessive foot moisture: Constantly moist or sweaty feet can create an environment conducive to HPV infection.
Symptoms of Plantar Warts
Rough, grainy growths: Small, rough lesions on the bottom of the foot, often on the heel or ball, that may interrupt normal skin lines.
Black pinpoints: Tiny black dots, known as wart seeds, which are small, clotted blood vessels.
Pain or tenderness: Discomfort when walking or standing, especially if the wart is located on a weight-bearing area.
Callus formation: A thickened layer of skin may form over the wart as it grows inward due to pressure.
Why Do My Warts Keep Coming Back?
Plantar warts often recur because the HPV strain can persist beneath the skin even when visible warts seem like they're fading away. This type of virus has developed mechanisms to evade the immune system, allowing it to remain undetected and cause warts to re-form later. That's why it's important to see your chiropodist one final time to verify that your warts are gone.
The immune system plays a crucial role in controlling HPV infections. Individuals with weakened immune responses or those on immunosuppressive therapies are more susceptible to recurrent warts . Additionally, certain HPV strains are more adept at evading immune detection, leading to higher rates of recurrence. Even in immunocompetent individuals, the virus can persist in a latent state and reactivate under certain conditions, which causes warts to come back.
Warts can also come back if you're re-exposed to the virus. For instance, you can get warts again if your feet come into contact with a surface that came into contact with the virus before being disinfected (i.e.: shared showers, locker rooms, gymnasiums, pools, etc.). That's why athletes and people who do barefoot sports (i.e.: swimming or gymnastics) are especially prone to wart reoccurrence. That's why it's important to disinfect footwear, along with high-risk surfaces with moisture buildup (i.e.: tubs and showers) with a 99% disinfectant solution that kills virus. This will kill any residual virus remaining in your belongings and residence and reduce the likelihood of re-exposure.
View this post on Instagram A post shared by Feet First Clinic (@feetfirstclinic_)
How to Stop Warts from Coming Back?
Preventative plantar warts care - both before and after contracting plantar warts - can help you avoid persistent foot warts. Remember, successfully treating warts doesn't make you immune to them in the future:
It's important to keep your feet clean and dry, especially after showers or swimming.
Always wear shower shoes or any suitable protective footwear in communal areas like pools and locker rooms.
Don’t share shoes or socks, and avoid touching or picking at existing warts to reduce the chance of spreading the virus.
Regularly disinfect home surfaces like bathroom floors and tubs if someone in the household has a wart.
Moisturizing cracked heels can also help create a stronger skin barrier.
After your last wart treatment, disinfect any footwear worn while you had the infection with a 99% disinfectant spray that kills viruses (i.e.: Lysol disinfectant spray).
These simple habits can go a long way in preventing warts recurrence.
What to do if my Warts Come Back?
If your plantar warts won’t go away on their own, wart removal treatment at a foot clinic from a chiropodist or podiatrist should be your next step. Here are some ways foot care professionals remove plantar warts:
Prescription Topical Solutions (Salicylic Acid): This medicated treatment involves applying a high-strength salicylic acid compound directly to the wart over time. It works by gradually breaking down layers of the skin until the wart tissue is removed. Fun fact: salicylic acid can also be used to treat acne!
Cryotherapy: This method uses liquid nitrogen to freeze the wart, causing it to blister and eventually fall away. The extreme cold damages the wart tissue and triggers the body to shed it during the healing process.
Cantharone/Cantharone Plus: A potent topical solution is painted onto the wart to create a blister between the wart and the healthy skin beneath it. This separation allows the wart to be lifted away once the blister dries out and peels off. It may cause more discomfort than other treatments but results may be faster.
Needing: A sterilized needle is used to puncture the wart multiple times after numbing the area. This process helps stimulate your immune system to recognize and fight off the virus that caused the wart.
Excision: In this procedure, the wart is surgically removed under local anesthesia. It’s typically used when other treatments haven’t worked and involves cutting the wart out and sealing the area to reduce the chance of it returning.
Remember that enjoying other routine foot clinic services can be a great preventative step in keeping your feet clean and healthy, and warts at bay. Even a service like callus removal, a medical pedicure or simply your first initial foot assessment can be helpful if your chiropodist or podiatrist spots a plantar wart during the process!
https://www.youtube.com/shorts/LjYyCurn_BM
December 26, 2024
While corns and plantar warts may look alike at first glance, they differ significantly in their causes, symptoms, and treatments. If you’re unsure about whether you have a corn or a plantar wart, visiting a chiropodist can help you receive an accurate diagnosis and appropriate treatment. Whether it’s corn enucleation or wart removal, timely intervention with a podiatrist or chiropodist at a foot clinic will ensure your feet stay healthy and pain-free.
What are Corns?
Corns are small, thickened areas of skin that develop in response to repeated friction, pressure, or irritation. They usually develop on the feet, particularly in weight-bearing areas such as the tops and sides of the toes or on the soles. Foot corns are essentially the skin's way of protecting itself from friction, forming as a shield for the underlying skin. The hardened layer is your body’s method of preventing skin ulceration.
There are different types of foot corns, each with its own characteristics. Hard corns are small, round, and painful, typically found on the bottom of the foot due to abnormal pressure or friction. Soft corns, which are usually located between the toes, are white and rubbery due to moisture. Seed corns are tiny, painless and appear on the sole of the foot.
Corns: Causes, Risk Factors and Symptoms
Generally speaking, corns are caused by inefficient foot mechanics which lead to excessive pressure and friction. They may also be linked to other foot conditions. For example, an abnormal gait pattern due to flat feet can lead to pressure points. This can then cause corn formation in vulnerable areas of your foot. Here are some key risk factors and causes:
Wearing high heels often.
Wearing shoes that are the wrong size.
Wearing uncomfortable shoes.
Not wearing socks with your shoes.
Irregular walking motion / abnormal gait.
Corn Symptoms Include:
Thickened, hardened areas of skin on the toes, sides, or soles of the feet
Rough or waxy texture on the affected area
Localized pain or tenderness, especially when pressure is applied
Yellowish or greyish appearance, sometimes with a central core
Discomfort during walking or wearing tight-fitting shoes
Interference with daily activities in severe cases
What are Plantar Warts?
Plantar warts are localized skin infections caused by certain strains of the human papillomavirus (HPV), specifically types 1, 2, and 4 which target the epidermis—the outermost layer of the skin. The strain of HPV can sometimes determine how painful a plantar wart may be. For example, HPV 1 may cause deeper, more painful warts, while HPV 2 causes more superficial ones.
These warts develop on the plantar surface of the foot, which includes the sole and heel, areas that bear significant weight and endure pressure during standing and walking. Unlike some other HPV-related warts, plantar warts are non-cancerous and are confined to the feet, as the virus is adapted to thrive in the thicker, tougher skin found on the soles. Plantar warts can last anywhere from two months to several years, especially if left untreated.
For individuals with a healthy immune system, plantar warts are generally not a significant health concern. However, they can make activities like walking, standing, or running very uncomfortable and painful. The pressure exerted on the wart may cause irritation and discomfort, which causes hardened skin to build up over the wart. The latter is also a big reason people confuse them with corns or calluses.
It’s important to seek treatment as soon as you notice any symptoms: Even if it's not interfering with your daily routine, it is still contagious so you can infect others. In addition, addressing these symptoms promptly with a foot specialist like a chiropodist or podiatrist can prevent further complications.
Plantar Warts: Causes, Risk Factors and Symptoms
Plantar warts are contagious and similar to fungal infections like athlete’s foot in that you can contract them by walking barefoot in public, moist spaces. Here are some more details on what activities or risk factors may lead to plantar warts:
You have a weakened immune system. Many people's immune system can recognize and fight off the HPV virus before warts form. However, people with a poorly functioning immune system are more susceptible as their body is less equipped recognize and fight the HPV virus. People who are immunocompromised may take longer to fight the virus, meaning that that the warts will take longer to treat.
You’re 65 or older, or a child or teenager: Plantar warts can be more common in these age brackets. For children, their immune systems are still developing, and they’re more likely to share communal spaces like gyms and locker rooms. For seniors, the immune system may be compromised.
Environment exposure and being barefoot: Frequenting warm, moist environments like swimming pools, locker rooms, and communal showers increases exposure to HPV. These areas are ideal breeding grounds for the virus, making it easy to contract through bare feet. Walking barefoot on abrasive surfaces, like pool decks or gym mats, can also create micro-injuries that allow HPV to enter.
Skin cracks and abrasions: Any break in the skin, including cracks, blisters, or injuries, can act as an entry point for the virus.
Poor foot hygiene practices: Neglecting foot care, such as not cleaning feet thoroughly or allowing them to remain damp for prolonged periods, can create conditions favourable for infection.
Plantar Wart Symptoms Include:
Rough, thick circular patches that have similar colouring and shape to a cauliflower.
Warts that form on the heels, around your toes, or on the ball of the foot.
Other discoloration: brown, pink, yellow or gray.
“Wart seeds” – which look like a small black dot in the wart
Pain, tenderness and general discomfort.
Bleeding.
Both cluster and solitary growth are possible.
Corns and Plantar Warts: Key Differences
While warts and corns can look and feel very similar, the main difference lies what causes them. Corns are caused by the body's response to excessive friction against the skin, whereas plantar warts are caused by strands of the contagious HPV virus.
Here are two additional ways to help distinguish between corns and plantar warts.
Pain type: Plantar warts may cause pain when pinched from the sides, whereas corns are tender when pressure is applied directly to them.
Appearance: Corns have a “waxy” yellowish appearance, whereas plantar warts often have a black dot in the centre. And while difficult to tell, warts go much deeper into the skin than corns.
Location: Corns tend to occur in the non-weight bearing parts of the foot, like between or on top of the toes. Conversely, plantar warts tend to occur on the weight-bearing parts of the foot, like the ball of the foot.
Multiplication and Spreading: Corns are concentrated in pressure-points on the foot and don't typically "spread". Plantar warts, however, can multiply and spread to other parts of the foot if the virus is allowed to grow unchecked.
Corns and Plantar Warts: Treatment and Prevention
https://www.youtube.com/shorts/TDV3Dd98oOM
Many services performed by a chiropodist or podiatrist are available at a foot clinic and can target both conditions.
How to Treat Plantar Warts
Plantar wart treatment requires a specialized approach. As they're caused by a virus, they cannot simply be "removed". Rather, depending on the severity of the warts, the frequency of re-exposure to the virus, and the person's immune system, warts can take multiple treatments spanning over several months.
Here are the different treatment options for plantar warts, in order from most conservative to most aggressive:
Salicylic acid, a common over-the-counter treatment, gradually softens the wart and sheds layers of skin. Although it is not painful, it may take longer to see results. For a faster alternative, a chiropodist can prescribe a higher-strength salicylic acid solution to be applied at home with follow-up visits. The chiropodist will then routinely debride the dead skin covering the wart to allow better penetration of the medication.
Cryotherapy, or freezing, is another standard method where liquid nitrogen is applied to the wart to freeze and destroy the wart tissue. This treatment may cause temporary pain and requires multiple sessions, each 2 -3 weeks apart.
Cantharone (canthacur) is an acid applied by a chiropodist that causes a blister to form and the wart to lift off the skin, typically within a few days. Although this treatment is more effective and doesn't take as long as cryotherapy, the resulting blister may be uncomfortable. This is the most common treatment used by chiropodists. It requires multiple treatments, each 2 - 3 weeks apart (though typically not as many as cryotherapy).
Wart needling is a surgical procedure. It involves puncturing the wart multiple times with a sterile needle to trigger the body's immune response. It is a good option for multiple or resistant warts.
Finally, excision involves surgical removal of the wart. It is reserved for stubborn warts that don't respond to other treatments, and has a risk of scarring. It is seldom used.
How to Treat Corns
A chiropodist or podiatrist can treat corns by gently shaving down the thickened skin with sterilized tools. The treatment is effective, safe, typically painless, and will discomfort without risking infection.
Inserts and custom orthotics can also play a significant role in managing and preventing recurrent corns. Custom orthotics are specially designed to provide support and distribute pressure evenly across the foot. This reduces the friction and pressure points that can lead to corns. Over-the-counter insoles and inserts can also provide extra cushioning and improve the fit of shoes, offering relief and preventing further irritation.
Self care can also go a long way. Soaking corns in warm water softens them, making it easier to reduce its size. It's also important to moisturize your feet regularly to make the skin stronger and more flexible, which will reduce its sensitivity to friction and hardened skin buildup. Toe pads or non-medicated patches can also protect corns from further irritation and promote healing.
Lastly, but equally important, you must find the right shoes to wear for each season and choose shoes with a proper fit. This can help prevent the pressure and friction that causes foot corns. A complimentary shoe fitting at a foot clinic can help!
https://www.youtube.com/shorts/R7GV0GbKhvQ
February 5, 2024
For runners, the feet are not just the point of contact with the ground; they are the foundation of every stride, absorbing the impact of countless steps. Our feet are like a car's wheels, enabling us to move forward. And shoes are our body's tires. That's why proper foot care for runners is paramount to ensure a smooth and injury-free running journey. This guide explores our top 10 foot care tips tailored specifically for runners so you can go the distance comfortably and confidently.
Tip #1: Choose the right running shoes
The foundation of good foot care starts with the right pair of running shoes. When selecting running shoes, consider factors such as:
Arch support,
Cushioning, and
The terrain you'll be running on.
Rotate your running shoes, if your budget allows it, to let them decompress and maintain their cushioning. You can visit a specialty store like Feet First Clinic to get footwear advice and fitted.
Read our complete guide on types of running shoes and how to choose your perfect pair.
Tip #2: Prioritize sock selection
Investing in quality moisture-wicking socks can make a significant difference in preventing blisters and discomfort. Choose socks with proper padding and avoid cotton, as it tends to retain moisture, increasing the risk of blisters.
Tip #3: Maintain proper hygiene
Regular foot hygiene is crucial for runners. Wash your feet daily and thoroughly dry them. And remember to get between the toes. Keep your toenails trimmed to prevent ingrown nails and potential discomfort during your runs. Adopting a regular foot care hygiene routine and following a post-sports routine is essential, especially for runners.
https://youtube.com/shorts/I65eFhvnPhw?si=UsB_TanLDKhrfu0P
Tip #4: Warm-up and stretch
Before hitting the pavement, take the time to warm up your feet and stretch your calf muscles. Gentle foot and ankle exercises can improve flexibility and reduce the risk of strains or plantar fasciitis.
Tip #5: Gradual progression and cross-training
Avoid overtraining by gradually increasing your mileage and intensity. Incorporate cross-training activities like cycling or swimming to give your feet a break while maintaining cardiovascular fitness.
Tip #6: Listen to your feet
Paying attention to any signs of discomfort or pain is crucial for preventing injuries. Don't run through pain. If you notice persistent pain, swelling, or changes in your foot structure, consult a healthcare professional or a podiatrist promptly.
Tip #7: Ice and elevation
After a long run, treat your feet to some post-run care. Wrapped cold compression any sore areas to reduce inflammation, and consider elevating your feet to minimize swelling. This simple routine can aid in faster recovery. Rest, ice, compression, and elevation (RICE) are methods for treating inflammation after trauma, such as acute ankle sprain. Inflammation causes pain, edema, hyperalgesia, and erythema, limiting one’s ability to perform the rehabilitation required for proper healing. But always have them check ed by a health professional.
Tip #8: Invest in insoles or orthotics (if needed)
Custom orthotics or over-the-counter insoles can provide additional support and stability if you have specific foot conditions or excessive pronation issues.
https://youtube.com/shorts/IBXAXoUouFY?si=5ZaUavzHKhMxgmiu
Consult a chiropodist to determine the best option for your individual needs.
Tip #9: Foot-strengthening exercises
Incorporate foot-strengthening exercises into your routine to improve stability and reduce the risk of injuries. Exercises like toe taps, marble pickups, and resistance band exercises can enhance the strength of the muscles supporting your feet.
https://youtube.com/shorts/gOwgyrmU6hM?si=1CVzRnpERTgb_jPo
Tip #10: Regular check-ups
Make regular foot check-ups a part of your routine. Addressing early signs of symptoms can keep them from escalating into significant problems. All foot pain treatment services at our foot clinic start with an assessment by one of our skilled chiropodists. Our chiropodists conduct foot assessments for:
Foot pain;
Footwear recommendations;
General foot check-ups;
Diagnostic Purposes; or
Any foot-related concern or condition.
November 16, 2023
When it comes to self-care and pampering, we often focus on treating ourselves to facials, massages, or spa days while neglecting one of our body's hardest working and overlooked parts: our feet.
Enter the world of medical pedicures, a rejuvenating and therapeutic experience that goes beyond the typical nail salon visit. In this blog post, we look at medical pedicures and uncover the many benefits they offer for the health of your feet.
Whether seeking relief from foot-related ailments or well-deserved self-care, a medical pedicure might be the secret to the happy and healthy feet you've been waiting for.
What's a medical pedicure?
A medical pedicure, also known as a medi-pedi, is a specialized foot treatment performed by a trained medical professional, typically a podiatrist or chiropodist.
Unlike a cosmetic pedicure you might receive at a spa or nail salon, a medical pedicure focuses on the medical aspects of foot care - there is no nail polish or foot soaking. It ususally involves the following:
Examination and consultation. Before the procedure, a chiropodist assesses your feet, discusses any concerns or foot-related issues you may have, and creates a treatment plan tailored to your needs.
Nail and callus care. A chiropodist trims and shapes your toenails, carefully avoiding ingrown toenails. They will also remove calluses and corns to relieve discomfort and prevent further complications.
Hygiene. A medical pedicure places a strong emphasis on hygiene. The instruments used are sterilized (or disposable) to prevent the risk of infection.
Skin and cuticle care. Your provider will moisturize and care for the skin on your feet, paying particular attention to dry or cracked areas. They will also address overgrown or problematic cuticles.
Why should I get a medical pedicure?
Only you can decide whether you need a medical pedicure, but we want to lay out the benefits to help you make an informed decision. There are several reasons why you may need one:
Treatment of Specific Foot Conditions
Medical pedicures are not just about pampering but about addressing specific foot conditions. Whether you're dealing with fungal infections, plantar warts, ingrown toenails, or thickened and discoloured nails, your healthcare specialist can offer treatments and recommendations for future care.
Proper Nail Care
While traditional pedicures focus primarily on nail aesthetics, medical pedicures focus on nail health. Sure, they will properly trim and file your toenails, but they'll also go the extra mile in preventing ingrown toenails and addressing any nail conditions like toenail fungus.
Healthy Skin
The skincare aspect of a medical pedicure involves moisturizing and nurturing the skin on your feet. Dry, cracked, or rough skin patches will be taken care of. Plus, we can provide product recommendations to help you maintain healthy, soft feet between appointments.
Education and Guidance
A significant part of a medical pedicure is education. You'll receive valuable guidance on proper foot care practices. In addition, with conditions like recurring calluses or ingrown toenails, the chiropodist can determine whether there could be any biomechanical factors at play. These insights empower you to take better care of your feet daily, reducing the likelihood of future issues.
March 9, 2023
Plantar warts and sports are an "iconic" duo of foot conditions and risk factors. Many athletes are looking for a quick fix for their plantar wart woes. But the truth is, switching your mindset towards prevention and medical foot care is just as important.
Let's look at our plantar wart guide for athletes and gym-goers! We'll answer some of your most pressing questions and dive into the following:
What are plantar warts?
Why are athletes prone to plantar warts?
Preventing plantar warts: foot hygiene and foot care
Prevention plantar warts: shoe choices
What are Plantar Warts?
Plantar warts are viral skin infections caused by the Human Papilloma Virus(HPV) that appear on the bottom of the feet.
Many people assume that HPV is solely a sexually transmitted infection, but there are over 200 strains, some causing warts and others causing cancer. People usually contract this virus strain by walking or running barefoot on an infected surface, which enters the skin via contact or through small cracks in the skin.
Warts appear round and look deceptively like corns, calluses and blisters. They result from the body's failure to fight off the HPV, which can sometimes disappear on its own depending on the strain. Symptoms and signs of plantar warts include:
A hard and "grainy" growth on the bottom of the foot, often on the ball of the foot or base of the toes
On dark skin, it may appear lighter than the surrounding skin
Calluses surrounding the wart if it has started to grow inward
"Wart seeds" - which look like a small black dot in the wart
Pain when walking or touching the wart
Mosaic warts or a cluster of warts
Treatment options from a foot clinic include cryotherapy and needling. You can read about treatments in more detail here.
Why are Athletes Prone to Plantar Warts?
Plantar warts have the potential to debilitate athletes and gym-goers and severely impact their physical progress. But why are the physically fit more likely to contract them in the first place?
HPV loves warm, moist environments. These include communal showers and locker rooms where sports teams typically congregate without shoes or socks. So without adequate foot protection, members of the same team can unknowingly pass on this troublesome skin infection to each other.
Competitive swimmers are also at risk since the walking area surrounding the swimming pools is also communal with heavy, barefoot traffic. Furthermore, the rough surfaces of pool decks may cause micro-trauma to the bottom of the feet, increasing the risk of viral contraction.
Athletes and fitness lovers are also more likely to experience hyperhidrosis, or excessive sweating of the feet, which can increase the risk. Athletes often also share infected gym equipment, such as mats, without thorough cleaning.
Photo by Anna Shvets from Pexels
Plantar Wart Prevention: Foot Hygiene and Foot Care
The best way to prevent plantar warts is to strictly monitor your foot health and keep your feet clean. If you already have plantar warts, these practices can help prevent the condition from worsening.
Here are some practices to abide by:
Follow a daily foot care routine, being careful not to miss days when you play sports or go to the gym. It should include cleaning, exfoliation, moisturizing, and more. Here is an excellent one to follow!
Lightly dust your feet with baby powder. This can also help with foot odour! You can also try Gehwol Foot Powder.
Wear moisture-wicking socks, foot pads or other protective products.
Never go barefoot in a communal area like a locker room, shower or pool deck. Always wear protective footwear like sandals or shower shoes while in these spaces.
Don't scratch or pick at any pre-existing plantar warts.
Air out your shoes after using them.
Always wash your hands if you touch one of your plantar warts.
Don't share shoes, socks, towels and other products with other people.
Plantar Wart Prevention: Shoe Choices
Athletes can't avoid keeping their feet cooped up in runners all day. What they can do, however, is make shoe choices that help to prevent the growth of plantar warts.
Shoes should be breathable and waterproof. You know how some runners have those mini holes in the upper that let air enter and escape? Those are the ones you should be on the hunt for! The ventilation keeps your foot environment fresh and healthy while you spend the day exerting energy. When shopping for shoes or attending a shoe fitting, stress the importance of finding shoes like these by asking for breathable options.
You can also look for shoes made with GORE-TEX fabric, which repels moisture while letting water vapour from sweat exit the shoe.
Looking For More Info on Plantar Warts?
We know that athletes are at risk of developing plantar warts, but did you know children are also vulnerable? If you're a concerned parent, check out this blog on managing plantar warts in children.