April 30, 2026
Our feet are what hold us up --- every single day! Whether it's at work for 8 hours or more, or during our morning exercise routine, healthy feet are essential for many of our daily activities. Therefore, you should invest in your foot health. Improper footwear can lead to various foot conditions, so you're better off ditching those bad shoes and looking for the perfect fit. Knowing the right shoe for you is important, but narrowing them down based on your specific foot type can be challenging. To help educate you on the differences, we will break down the 2 most common types of footwear. Keep in mind, we're not talking about high heels, sneakers, etc. We're specifically breaking down the 2 types of footwear based on their structural characteristics and how they will compliment your feet.
Importance of Knowing Your Arch Mechanics
It’s important to learn the structure of your feet, specifically your arch, as it provides some hints as to what the best shoe might be for you. A simple test, called the Wet test, can help sometimes determine your arch type. But to know for sure, it's recommended to get a foot assessment by a chiropodist.
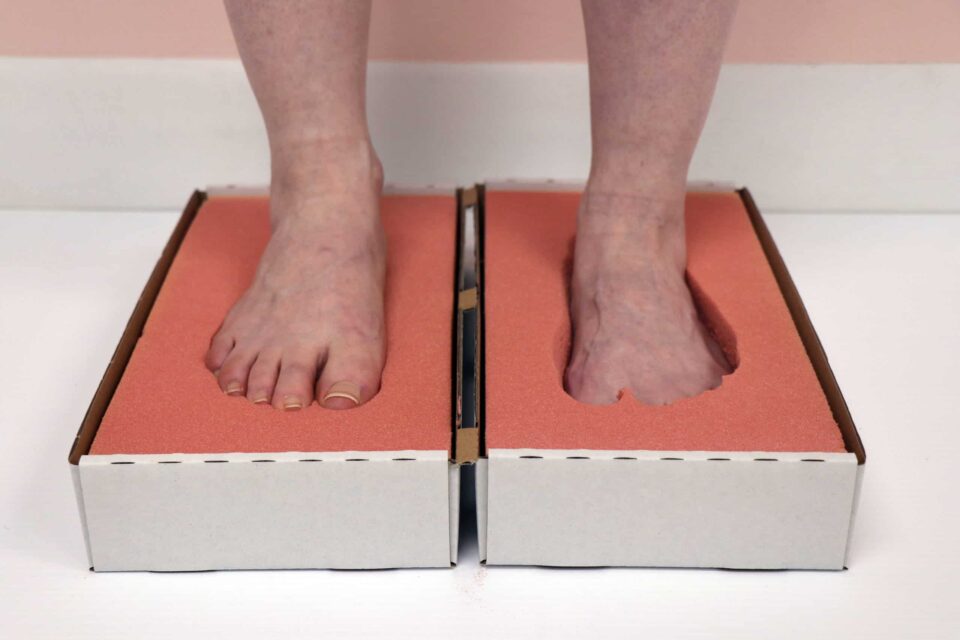
The wet test process:
Dip the soles of your feet into water.
Stand on a piece of paper.
When you step off, you should see an imprint of your foot which will show you your arch type.
Seeing half of your arch (the middle portion of your foot) indicates a normal arch, while seeing the majority of your arch on the paper indicates you have flat feet (or a low arch). Conversely, seeing minimal arch indicates a high arch. Now that we know this, we can look into the 3 types of footwear.
2 Main Types of Footwear are:
Stability
Neutral
Stability
Normal, flat and low arches are best suited for stability footwear. Stability footwear is the most supportive and corrective. Stability essentially prevents excessive pronation (inward movement) of your foot, which reduces strain and pressure on the joints and muscles in the feet. To correct overpronation (when your foot rolls too far inward), these shoes have medial support - called a medial post - built into the midsole.
Stability shoes also feature a firm heel counter for ankle support. The additional ankle support in stability shoes also makes them great for people who don't overpronate but may have ankle instability, such as people with Achilles tendonitis.
Neutral
As the name implies, neutral cushioned shoes do not have medial support or features within the midsole. With neutral shoes, there is simply cushioning, and no wedges or stiff plastic support along the arch. This can prevent any sort of under or overcompensation when walking or running. Overall, the structure of the shoe is relatively symmetrical.
Regular pronators and supinators (when your foot fails to roll inwards and instead applies pressure to your outer foot) should consider using neutral shoes because any stability features would be moot.
Final Advice
It’s important to note that the amount of cushioning is not necessarily an indicator of the type of shoe, but rather it’s a combination of medial features, stiff plastic, and other factors. Cushioning can also be stiff, or soft, depending on the denseness and type of foam.
Ultimately, and as The Mayo Clinic notes, “there is no one best shoe or a particular foot type, and comfort and proper fit should be the main criteria you use when selecting new athletic shoes.”
Now that you're aware of the 3 types of footwear, you can asses your needs and make the right footwear choices!
March 26, 2026
You’re having some problems with your feet. Maybe it’s a painful ingrown toenail or heel pain or even a stubborn wart that won’t go away, and you made an appointment with a Registered Chiropodist at your local foot clinic. The appointment is approaching and you’re feeling a little anxious because of the unknown, unfamiliar territory you will be encountering. What will happen? What do I have to bring? Will it be uncomfortable? Here is a quick read on what to expect at your first appointment at a foot clinic to help you calm those nerves.
Before Your Appointment
Before your visit, we recommend checking your insurance coverage. Chiropody visits are covered under most insurance plans with extended health benefits, and knowing what your covered for ahead of time will ensure a smooth process. In addition to checking your visit coverage, it's a good idea to also check your coverage for orthopaedic devices in case any are recommended.
You'll also be sent an online intake form to fill out before your appointment. Completing the intake form before your appointment will make check-in faster on the day of your appointment. If you're unable to complete the intake form before your appointment, we recommend arriving 10 minutes early to leave enough time for filling out the form at the clinic. For your intake form, you will provide a list of your medications, note any allergies you may have, and document any relevant medical history. Providing as much detail as possible to your health care provider will help build a complete picture, so they can make an informed diagnosis and come up with the best treatment plan.
At Your Appointment
Once you arrive to your initial appointment, you will likely be greeted by the receptionist and checked in. You will then be escorted to a treatment room where a chiropodist will ask you to remove your shoes and socks and voice your concerns with your feet.
After this, the chiropodist will take a look at your feet and carry out the necessary assessments to determine a differential diagnoses. Depending on the reason for your visit, the chiropodist will check for the following:
Circulation or blood flow to your feet
Neurological status
Changes to or concerns with the skin and toenails (if your visit is for foot care)
Biomechanical abnormalities (i.e. limited or excessive range of motion in joints, areas of pain, overpronation, flat feet, etc) - if your visit is for foot pain.
After the assessment, the chiropodist will explain his or her findings and propose a treatment plan. Treatment will only commence with your consent. In general, treatment is usually painless. In fact, more often than not, if you enter the appointment with pain or discomfort, you will leave relieved of that pain.
Finally, although it may seem unusual to you to have someone look at or touch your feet, know that it is second nature to the Chiropodist.
Your chiropodist would have seen numerous amounts of feet, all of different shapes, colours, and sizes, and encountered a variety of foot concerns.
So don’t be embarrassed, and don’t be afraid to receive the care you need.
After Your Appointment
After your appointment, the receptionist will book your next visit and cash you out. You may also wish to purchase any recommended foot products or devices to help maintain your feet between visits. This can range from footwear, to foot cream, to toe devices. Whatever you need, our staff can help you find the right product for you that aligns with the chiropodist's recommendations.
After that, it's then important to follow through on the chiropodist's recommended treatment plan. Whether it's stretches, moisturizing daily, or wearing the right shoes, taking care of your feet between appointments is super important to keeping your feet healthy.
And that's it! We look forward to seeing you again soon!
February 19, 2026
Sometimes our shoes need that extra layer of comfort and resiliency to protect us from foot pain. For those already experiencing foot pain, you should take the time to invest in proper foot care right away. You may think Custom Orthotics are the only way to go, which can be true at times. That being said, Superfeet insoles are another option that can help with a wide range of Foot conditions. With this in mind, Feet First Clinic is proud to offer Superfeet insoles, which provide comfort and stability to anyone who needs them.
Superfeet offers a wide array of insoles that all provide relief and support. Not only suitable for foot pain, high-quality insoles have also been credited with helping conditions like back pain. They're also favourable for those with flat feet or a high arch. Some are more tailored for different needs and activities, some for different shoes. The Superfeet insole you choose will ultimately depend on your needs and the shoes you wear them with (which is why you should always try them with the shoes you want to wear them with before purchasing).
Superfeet Insoles: Classic Features
Superfeet insoles are made with high-quality materials and features that support foot health, including:
High-density foam: One of the best materials for insoles, it offers a firm foundation, comfort and sufficient shock absorption.
Heel cup: This can help stabilize the foot for those who need it. It also helps properly align the foot.
Odour control: Some Superfeet insoles feature an odour-control coating that helps prevent bacteria growth and keeps the insoles smelling fresh.
Contoured shape: All Superfeet insoles come with a shape that accommodates various foot types.
How to Choose Over-the-Counter Insoles
When shopping for over-the-counter insoles, it's important to consider the following:
Arch Height: High, medium, or low/flat
Primary Use: Running, walking, work boots, slim footwear, or all-day casual use
Cushion vs. Support: Do you want plush softness, firm structure, or a balance?
Shoe Fit: Roomy vs. snug-fitting shoes
Available Superfeet Options
We'll discuss the following Superfeet insoles with the hope that you can find the right one for you:
All-Purpose Support High Arch (formerly Green)
All-Purpose Support Medium Arch (formerly Blue)
All-Purpose Support Low Arch (formerly Black)
All-Purpose Women's High Impact Support (formerly Berry)
All-Purpose High Impact Support (formerly Orange)
All-Purpose Memory Foam Support (formerly Copper)
Carbon
Run Cushion High Arch
Work Cushion
Work Slim-Fit Cushion
Best Insoles for High Arches
All-Purpose Support High Arch (Green)
Choosing insoles with high arches can seem like a lost cause, but Superfeet Green is great for this foot type. In fact, Superfeet Green is Superfeet’s flagship product, and its most popular. One of the reasons why is its high arch support, which differentiates it from the Blue and Orange insoles. This high arch support helps alleviate foot, ankle, back, and knee pain by properly distributing pressure along the foot. Superfeet Green also provides the most support and stability among all Superfeet’s insoles. It's beneficial for a variety of other foot conditions too, such as plantar fasciitis and even flat feet (albeit with a break-in period).
If you have high arches, but need extra cushioning and flexibility, you may also want to consider the Run Cushion High Arch or Work Cushion:
Run Cushion High Arch
This insole has all the supportive features of the Green, but with extra cushioning and flexibility. It's a great option for people who love the support of Green, but not the firmness. It's also great for sports and high-impact activities.
Work Cushion
This insole is designed especially for safety shoes and safety boots, but they go great with all footwear. They're designed for people who are on their feet all day and feature extra cushioning and shock absorption in the weight bearing parts of the foot (under the ball of the foot and the heel). It also has extra support around the heel, which makes it great for people who overpronate and need extra stability in their shoes.
All Purpose Memory Foam Support (formerly Copper)
Cushioning is one of the most important features to look for in an insole if you have high arches. That's because less of your foot contacts the ground, which concentrates more shock and force onto a smaller area. This means your feet can't properly absorb shock when you move. Cushioning provides that shock absorption for you. While the arch profile on the Copper insole is lower than the others listed above, it has abundant memory foam cushioning to soften each step you take.
Thin Insoles - Dress/Slim Fitting Shoes
Black
The Superfeet Black insole is thinner, which makes it very adaptable. It fits snugly inside a wide range of footwear types, provides shock absorption and has an odour-control coating.
Carbon
The Superfeet Carbon insole is designed specifically for those interested in optimal performance enhancement. While still being lightweight, the Superfeet Carbon insole stands out with its "carbon fibre-reinforced stabilizer cap with a durable, ultralight foam layer." Superfeet notes that the Carbon insole is especially suitable for running shoes and cleats. The trademark Superfeet features, such as foam cushioning, the resilient shape and the heel cup, are also present.
It's super-thin profile also makes it perfect for dress shoes and shoes that don't have removable insoles.
Best Insoles for Flat Feet
All Purpose Support Medium Arch (formerly Blue)
Some of the best insoles for flat feet are Superfeet’s Blue inserts. The deep heel cups stabilizes the flat foot and prevents it from rolling inward, also known as overpronation. Individuals with this foot type often experience plantar fasciitis over time, and wearing Superfeet Blue can be preventative and, according to Mayo Clinic, reduce symptoms like foot pain.
Superfeet Blue also hasa medium arch shape. This allows you to get the arch support you need, without being too aggressive and putting too much pressure along the arch. It’s also important to note that despite their thin appearance, Superfeet Blues are firm and highly durable. The thinness lets you use them in various footwear, making them one of the most popular over-the-counter insoles and a great option if the insoles with higher arch support (i.e.: Green, Run Cushion High Arch) don't fit into your shoes.
All Purpose Women's High Impact Support (formerly Berry)
If you like the arch and support of blue, but want a little extra cushioning, Berry could be a great option. The Berry is designed to accommodate the female foot, which characteristically has a slimmer heel. The arch length is also catered to support women. If you're a busy woman who spends long hours on her feet, whether it be for work or physical activity, this may be the insole for you.
Superfeet Berry also comes with foam cushioning, allowing all of your footwear to feel exceptionally comfortable and preventing foot pain. The odour-control coating also fights bacteria from causing unpleasant foot odour. Lastly, like any good insole, the Superfeet Berry provides excellent shock absorption while running, with extra padding underneath the metatarsal (forefoot) area.
Insoles for Normal Arches / High-Impact Activities: Superfeet Orange
Superfeet Orange is a good choice for people with a normal to slightly pronounced arch. However, whether its brisk walking or playing sports, Superfeet Orange is great for physically active individuals. The heel cup perfectly cradles the foot during exercise, providing maximum control and optimal positioning of the soft tissue beneath the heel. Superfeet Orange also stands out with its extra high-impact foam on the forefoot, where the ball of the foot generally withstands the most pressure.
It’s important to note that many Superfeet varieties complement a normal arch. Furthermore, flatter and more pronounced arches may also be able to mix and match different insole types. These are simply some of our best sellers. To learn about the various types of Superfeet insoles, click here.
January 22, 2026
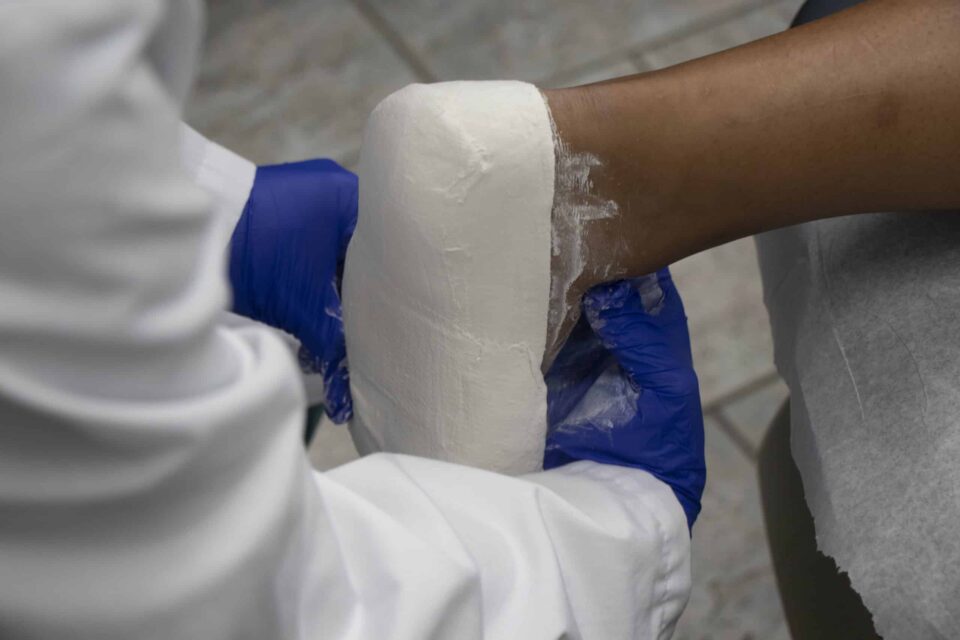
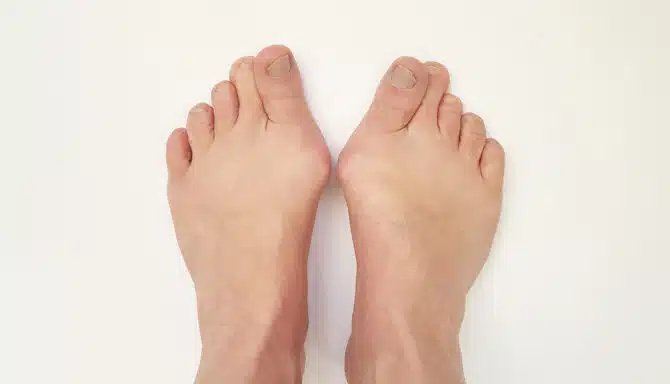
A bunion, medically known as hallux abducto valgus, is an angular bony protrusion that forms at the base of the joint that connects your big toe to your foot.
This joint, called the first metatarsophalangeal joint (or MTP joint for short), is a critical junction of bones, tendons, and ligaments that bear much of our weight when we’re on our feet. With bunions, the joint deviates its proper alignment, which causes the big toe to slowly and gradually turns towards the smaller toes.
This foot deformity occurs in about 10-30% of the population, affecting twice as many females as males. Bunions are caused or contributed to by wearing poor-fitting shoes, faulty foot mechanics, muscle imbalances, lax ligaments, inflammatory arthritic conditions, and genetics.
Bunions can be asymptomatic, although some people may experience pain, redness, and swelling at the joint, especially with tight footwear and extended periods of standing or walking. Symptoms may lessen with rest, biomechanical correction, and improved footwear choices.
Unfortunately, a bunion is a progressive deformity and is irreversible without surgical intervention. This means they will slowly get worse over time. However, addressing underlying biomechanical factors may help slow its progression and reduce symptoms.
Stages of Bunions
Bunions are categorized in stages to determine the severity of the deformity.
Without treatment, there is a greater risk a bunion will progress from one stage to the next.
Stage 1
Visually, a bunion at this stage is considered mild. There may be a small “bump” at the side of the 1st MTP joint and the big toe will be slightly turned towards the second toe, although not touching it.
Stage 2
The big toe further deviates from the MTP joint. At this stage, the first toe may be touching the second toe beside it.
Stage 3
At this stage, the base of the first toe develops a bone spur. This makes the bony protrusion more significant. The first toe also starts to rotate on its axis away from the mid-line of the body.
Stage 4
At stage 4, the first MTP joint has dislocated and the first toe will cross over or under toe. At this stage, the second toe will also present with a hammer toe deformity.
Managing Bunions
Although the only way to reverse a bunion is by surgery, it is only recommended if symptoms are not manageable by conservative measures and if function is severely compromised. Regardless of whether or not surgery is done, non-surgical treatment must be done, otherwise the bunion will reoccur.
Conservative treatments help to slow down the progression of a bunion as well as manage pain. It includes custom foot orthotics, splints, bunions guards, toe separators, and foot exercises.
Talk to your Chiropodist about the stage of your bunions and which conservative treatment options would be best for you!
January 8, 2026
Hiking is a great form of exercise and a fun way to get outdoors during the colder months of the year. However, if you’re planning on going for a hike, you need to know how to keep your feet warm and safe. Not only will this keep you comfortable during your journey, but it will also minimize the chances of you getting frostbite or another cold-related issue. That is why we are highlighting our top winter hiking tips, with a focus on proper footwear and keeping your feet protected in icy and snowy conditions. Continue reading to learn more about how you can protect your feet while hiking in the winter.
Wear Boots That Fit Properly
Before going on a hike, you need to assess the quality of your footwear. Preferably, you have a pair of warm boots that you can wear. By wearing boots, you’ll be able to walk in deep snowdrifts without worrying about getting your feet wet. Look for boots that are waterproof and insulated. If your boots are not insulated, be sure to wear them with a wool sock (more on that below).
However, it doesn't matter how warm your boots are if they don't fit. Tight-fitting boots will restrict circulation, which will make your feet feel cold no matter what you do. That's why boots should fit properly: When purchasing boots, try them on in-store with a warm, thick sock. When in doubt, it's better to go too big than too small.
Wear The Right Pair Of Socks
Everybody knows that you should never go on a winter hiking trip without a warm pair of socks. Look for thermal socks with thermoregulating materials like merino wool. Materials will not only keep your feet warm; they're also breathable, meaning you won't need to worry about foot sweat (moisture buildup from foot sweat will make your feet cold).
Whatever you do, do not double-layer socks; the increased thickness can make your shoes too tight, which will restrict circulation and make your feet colder.
If you have poor circulation or suffer from conditions like Peripheral neuropathy (nerve damage caused by diabetes), you may want to wear a pair of compression stockings. Compression stockings are high-quality garments that are made to stimulate the blood flow in your feet and lower body. These garments can help prevent pain in several ways. Some benefits include:
Boosting circulation to your lower extremities to help keep them warm
Decreased swelling in your ankles and knees
Minimizing aching and overall discomfort
Reducing leg and foot fatigue
If you don’t currently suffer from any of the issues mentioned above, you can still benefit from wearing compression stockings! They can help prevent issues like:
Blood clots
Varicose veins
Complications due to venous disorders
Keep Your Feet Dry
Keeping your feet dry is just as important as keeping them warm during winter hikes. Moisture from snow, slush, or sweat can quickly lower foot temperature and increase the risk of blisters, irritation, and cold related injuries. Choose waterproof or water resistant boots whenever possible, and consider wearing moisture wicking socks to help pull sweat away from the skin. Packing an extra pair of socks in your backpack is also a smart idea, as changing into a dry pair during or after your hike can significantly improve comfort and help protect your feet from the cold.
Wear Shoes with Good Tread
Winter can make for slippery conditions. Whether it's slush, snow or ice, it's easy to lose your footing on winter trails. That's why it's important to look for shoes with a good tread and traction. The outsole should be rubber or a high-abrasion rubber compound. Tread depth and tread pattern is also very important. Ideally, the tread depth should be at least 5 mm, and the pattern should have many small shapes. A waterproof hiking shoe or hiking boot usually will do the trick!
July 10, 2025
What is an Ankle Foot Orthotic (AFO)?
An ankle foot orthotic (AFO) is a medical-grade brace that supports the foot and ankle. It often extends partway up the calf. Unlike regular foot orthotics—which fit inside shoes to support the arch and heel. AFOs offer external stabilization of both the foot and ankle joints.
AFOs are commonly made of lightweight plastic or carbon fiber and may be custom-made or prefabricated. They assist walking, correct alignment, reduce pain, and help prevent further injury.
Who Needs an AFO?
Image from https://braceworks.ca/ and the Washington Post
AFO's received mainstream attention a few years ago when NFL quarterback Alex Smith returned to the football field after a catastrophic leg injury. The key to his return: an ankle foot orthotic. Due to a post-surgical infection, the nerve that helps flex the right foot was severed. This meant he couldn't lift his foot. So he got an AFO to help and made a brief comeback (with the help of an extensive rehab team).
So who exactly needs an AFO? Since AFOs are heftier than regular orthotics, they're typically recommended for patients with more complex conditions than those addressed by traditional foot orthotics. You might benefit from an AFO brace if you have:
Foot drop (difficulty lifting the front of the foot)
Cerebral palsy or neuromuscular disorders
Stroke-related gait issues
Multiple sclerosis (MS)
Post-surgical ankle instability
Tendon or ligament injuries
Severe arthritis affecting ankle mechanics
Ankle foot orthotics are most commonly indicated for neuromuscular disorders and foot drop.
AFOs v Regular Orthotics: What's the Difference?
FeatureRegular OrthoticsAnkle Foot Orthotics (AFOs)ScopeFoot support onlyFoot and ankle supportPlacementInside the shoe (underneath the foot)Worn underneath and around the foot, and around the ankleConditions TreatedArch pain, plantar fasciitis, overpronation, high arches, other biomechanical irregularitiesNeurological and structural gait disorders, severe instabilityCustomizationOften custom-fit or prefabOften custom-molded to leg shapeMobility SupportModerateHigh—can aid in walking and balance
While regular orthotics focus on redistributing pressure and correcting foot mechanics inside the shoe, AFOs provide external control for more complex biomechanical or neurological issues. Think of it as the difference between cushioning a sore spot and physically guiding your limb’s motion.
How Are AFOs Made and Fitted?
https://www.youtube.com/watch?v=nA_QklH7AWY
AFOs are usually prescribed by a foot specialist or chiropodist after a full assessment. The process may include:
Biomechanical Assessment
Gait analysis
Casting or 3D scanning
Custom fabrication
Fitting and adjustments
Some patients may only need short-term use post-injury or surgery, while others may rely on AFOs for long-term mobility support.
Final Thoughts
If you’ve been told you need more than just arch support or if your walking pattern has changed due to injury or illness, an ankle foot orthotic could be a game-changer. At our clinic, we assess your full biomechanics and work with you to find the right support—whether that’s a custom orthotic, AFO, or a combination of both.