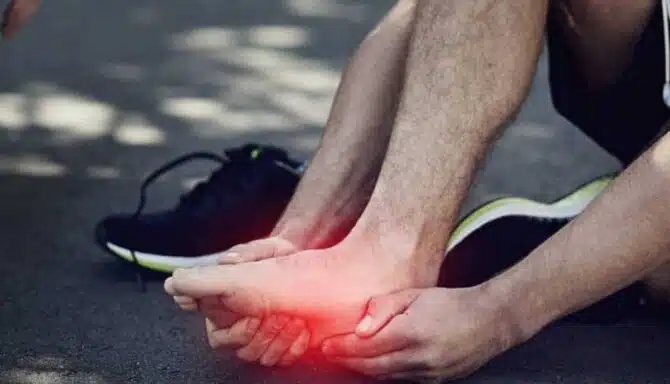
July 8, 2024
Shock absorption sounds like a superpower! But it’s actually a term describing how our shoes provide impact protection from the ground, floors and pavement. This benefits our foot health, but it also begins the upward “chain of command” of protecting the joints, bones and muscles in our knees, back and legs. Shock absorption in shoes typically involves innovative footwear technology and high-quality shoe design. Let’s review everything you need to know about this fascinating topic!
The Science Behind Shock Absorption in Shoes
You may be familiar with how cars have pump-like systems called shock absorbers, which dampen impulses from driving on the pavement. Your shoes are similar, but the physics are a little different!
Shoes with a good amount of shock absorption may include the following components:
Solid shoe cushioning in the insole, often made from gel, foam, etc.
Midsoles made from comfortable and sometimes dense materials, like EVA foam. These midsoles are often able to compress and then return to their original shape during movement.
Durable outsoles, made from materials like rubber.
Extra heel cushioning for heel striking.
These features work together to protect your feet from developing musculoskeletal foot conditions, which include but aren't limited to:
Plantar fasciitis
Heel spurs
Metatarsalgia
Different types of arthritis
Achilles Tendonitis
Think about it this way: nobody wants to walk a mile in flip flops! There would be virtually nothing in between the bottom of your foot and the ground’s surface, and you would feel fatigue, pain and overall discomfort afterwards. The longer you ignore foot support and shock absorption, the more wear and tear you will sustain!
And this affects more than just your feet — your entire body feels the impact. The pain starts at the foundation, your feet, but it will trickle upward to other body parts (knees, back, etc) since your muscles, ligaments, tendons and bones are all connected to ensure our body moves efficiently and with stability.
Who Needs Shock Absorption The Most?
Athletes, especially runners, benefit from shock absorption. With each stride, they are hitting the pavement, trails and floors harder than anyone else. They need high-quality athletic footwear that retains most of its shock absorbing abilities after long-term use.
But it’s not just all-star athletes. Everyday folks enjoying an outdoor walk in downtown Toronto; the longer the walk the more shock absorption you'll need. People with disabilities like severe arthritis or those with foot conditions like bunions or hammertoes, to name a few, should also be mindful of the grounds impact on the feet and body.
A Final Note on Shock Absorption
Shock absorption can be a balancing act. Sometimes “less is more" and you want to be careful of completely eliminating the “ground feel.”
For example, overly cushioned shoes and a very elevated outsole might not be right for people with mobility challenges or those who need walking shoes instead of running shoes. Both can lead to instability and a heightened risk of sustaining a foot injury.
Athletes should also be careful. Sometimes, too soft or too thick soles can affect sensory feedback and lead to a fall.
June 13, 2024
Did you know that the joint at the base of our big toe bears about 40% of our bodyweight when we move? It plays a significant role when we walk and run, and because of the weight it bears (literally), it's prone to arthritis. This condition is called hallux rigidus (often referred to as "stiff big toe") and it causes the joint to lose its range of motion. While a "stiff joint" may seem small, it actually can significantly alter our biomechanics and can cause pain and difficulty walking and running. While non-surgical treatments such as medication, orthotics, and physical therapy can help in the early stages, more severe cases may require surgical intervention.
One such surgical procedure to treat hallux rigidus is a cheilectomy. This article will explore what a cheilectomy is, its benefits, risks, and the recovery process.
What is a cheilectomy
A side-by-side of two feet: on the left is the post-surgical foot with a surgical shoe. On the right is the equivalent surgical reference for where the surgery is done and the incision size.
A cheilectomy is a surgical procedure that alleviates pain and restores motion in the big toe joint affected by hallux rigidus. This procedure removes bone spurs (osteophytes) and diseased tissue from the top of the metatarsal bone, which reduces pain and allows the joint to move more freely.
Cheilectomy: The procedure
A cheilectomy is usually done under local or general anaesthesia. The surgeon makes an incision over the top of the affected joint and then carefully removes the excess bone and tissue and smooths the joint surface. This frees up more space for joint movement. In some cases, the surgeon may do additional procedures, such as joint capsule release or cartilage repair, to improve the outcome.
Cheilectomy: The benefits
An aerial view of a bone spur above the first MTP joint (left foot, right of image).
Pain relief: A cheilectomy can significantly reduce pain and discomfort associated with hallux rigidus by eliminating bone spurs and diseased tissue.
Improved motion: The procedure frees up space around the big toe joint, which gives it more room to move around and restores the toe's flexibility and range of motion. This makes walking, running, and other activities more comfortable.
Preservation of joint function: Unlike more invasive procedures like joint fusion, a cheilectomy aims to preserve the natural mechanics of the big toe joint, which helps maintain its function and stability.
The same foot with the bone spur above the first MTP joint removed.
Cheilectomy: Risks and considerations
While cheilectomy is generally considered safe and effective, like any surgical procedure, it carries certain risks. These include infection, bleeding and nerve damage. There are also many factors that can affect the outcome, such as the severity of the condition, age, and the patient's overall foot health. If you're considering a cheilectomy, it's important to discuss the risks and the benefits with your healthcare provider so that you can manage your expectations properly assess with a cheilectomy is right for you.
Cheilectomy: What's the recovery?
Following a cheilectomy, it's normal to experience discomfort and swelling. You can manage this with pain medication and elevation. You'll also need to do physiotherapy during the recovery process to restore the strength and flexibility in the toe joint.
Most patients are fully weight-bearing immediately after the surgery, and can usually return to light activities within a few weeks; however full recovery takes several months. Stitches are typically removed 2 weeks after the procedure. It's important to follow post-operative instructions from the surgeon and to attend routine follow-up appointments to monitor the progress.
April 29, 2024
Heel pain is a common complaint affecting individuals of all ages and lifestyles, from athletes to office workers. It can be frustrating and debilitating, whether it's caused by plantar fasciitis, heel spurs, or Achilles tendonitis. Fortunately, you can take steps to prevent heel pain and keep your feet happy and healthy.
This blog post explores practical tips and exercises for preventing heel pain and maintaining optimal foot health.
Causes of heel pain
Before diving into prevention strategies, it's essential to understand the common causes of heel pain. Plantar fasciitis, the inflammation of the band of tissue that runs along the bottom of the foot, is one of the leading causes of heel pain. Other culprits include:
Heel spurs
Bony growths on the heel bone
Achilles tendonitis
Inflammation of the Achilles tendon at the back of the heel
Factors such as improper footwear, overuse, obesity, and poor foot mechanics can contribute to the development of heel pain.
Heel pain prevention tips
Choose supportive footwear. Invest in shoes that provide adequate arch support, cushioning, and stability. Look for options with a slightly elevated heel to reduce strain on the Achilles tendon and plantar fascia.
Maintain a healthy weight. Excess weight can put added pressure on the feet and exacerbate heel pain. Maintain a healthy weight through a balanced diet and regular exercise to reduce the risk of developing heel pain.
Gradually increase activity. Avoid sudden increases in physical activity, such as jumping into a rigorous exercise routine or increasing mileage too quickly. Gradually increase activity levels to allow your feet time to adapt and prevent overuse injuries.
Stretch regularly. Incorporate stretching exercises into your daily routine to improve flexibility and prevent tightness in the calf muscles and Achilles tendon. Focus on stretching the calves, hamstrings, and plantar fascia to alleviate tension and reduce heel strain.
Practice good foot mechanics. Pay attention to your foot mechanics when walking, running, or participating in sports. Avoid overpronation or excessive rolling inward of the feet, as this can strain the plantar fascia and Achilles tendon.
Heel pain exercises
Calf stretch. Stand facing a wall with one foot in front of the other, keeping the back leg straight and the heel on the ground. Lean forward, bending the front knee until you feel a stretch in the calf of the back leg. Hold for 30 seconds, then switch sides.
Plantar fascia stretch. Sit on the floor with one leg extended before you. Loop a towel around the foot and gently pull the toes towards you until you feel a stretch along the bottom of the foot. Hold for 30 seconds, then switch sides.
Achilles tendon stretch. Stand facing a wall with one foot in front of the other. Place your hands on the wall at shoulder height and lean forward, bending the front knee until you feel a stretch in the back of the lower leg. Hold for 30 seconds, then switch sides.
Heel pain can be debilitating and impact daily activities and quality of life. Incorporating these prevention tips and exercises into your routine can reduce the risk of developing heel pain and keep your feet healthy and pain-free. Remember to listen to your body and seek professional medical attention if you experience persistent or severe heel pain.
September 18, 2023
Although it may sound scary, ankle cracking isn't necessarily a sign to worry about. Often, ankle cracking is normal and, fortunately, harmless.
There's a minor chance ankle popping can signify an underlying condition like a sprain or tendon damage, but that's not generally the case. Ankle cracking or popping when rotating can be a common occurrence for some people.
However, this doesn't mean you should ignore ankle cracking altogether. You should monitor and assess whether you experience pain elsewhere or any other symptoms associated with the ankle popping (for instance, deep pain that could be a sign of a stress fracture). Understanding your recent history also helps - be extra careful if you've experienced a recent injury or trauma.
Whether severe or a non-issue, we recommend brushing up on the possible reasons your ankle cracks when rotating. Read more in our comprehensive guide below.
Gas bubble release
The most common cause of ankle cracks when rotating is cavitation. When you rotate your ankle, the movement can cause tiny gas bubbles to form and collapse within the synovial fluid that lubricates the joint. This sudden collapse of gas bubbles can produce an audible cracking or even popping sound. Ankle cracking in this context is normal and harmless.
Ligament or tendon movement
Ankle cracks when cracking can also be due to the movement of ligaments or tendons over bony structures in the ankle joint. They may produce a popping sensation or sound as they shift during rotation.
Tendon snapping
Why Your Ankle Cracks When Rotating
Sometimes, a tendon can snap over a bony prominence in the ankle, leading to a popping sensation or sound. This typically occurs due to repetitive movements or increased physical activity.
Scar tissue or adhesions
Past injuries or trauma to the ankle may create scar tissue or adhesions around the joint. These tissues may stretch or release during ankle rotation, causing a cracking noise.
Joint instability
Ankle cracking can be associated with joint instability. If the ligaments supporting the ankle are lax or weakened, the bones may move more than usual during rotation, leading to a popping sensation.
Arthritis
Occasionally, arthritis or inflammation in the ankle joint can cause cracking or popping sounds during movement. This is often accompanied by pain and stiffness.
Synovial cysts
Synovial cysts are fluid-filled sacs that can develop within the ankle joint. These cysts may cause cracking or popping sensations when they move or change position during ankle rotation.
Bone-on-bone movement
In rare cases where there is existing significant wear and tear in the ankle joint, bone surfaces may rub against each other during movement. This results in cracking sounds. Be careful with bone-on-bone friction; it's a recipe for developing bone spurs, which are calcium deposits that build up over time into outgrowths.
How do I know when ankle cracking is severe?
In most cases, ankle cracking during rotation is benign and not a cause for concern. However, we recommend seeing a professional if you experience pain, swelling, or instability along with the cracking or other concerning symptoms accompanying the cracking. They can thoroughly evaluate and provide appropriate advice or treatment based on the underlying cause.
How do I prevent or reduce ankle cracking?
To reduce the occurrence of ankle cracking and maintain ankle health, you can consider the following preventive measures:
Regularly perform ankle exercises to strengthen the muscles supporting the joint.
Warm up properly before physical activity to prepare the ankles for movement.
Avoid excessive or forceful rotation of the ankles, especially if it causes pain or discomfort.
Wear appropriate footwear that provides support and cushioning for the ankles.
June 26, 2023
A Heel spur is a bony growth on the heel bone (calcaneus). It is often associated with plantar fasciitis, in which the plantar fascia, a thick band of tissue along the bottom of the foot, becomes inflamed. A heel spur is the most common bone spur.
In minor cases, you may experience discomfort in the heel from time to time. In more severe cases, the bony outgrowth may protrude from the heel and a bump on the underside of the foot. Generally, the larger the outgrowth, the more sensitive your heel becomes to stress, which can exacerbate the condition. However, roughly 15-30% of cases are asymptomatic with no pain.
In this post, we uncover the causes, symptoms, and treatments for heel spurs, so you can kick discomfort to the curb and get back on your feet. Ready to say goodbye to heel pain? Read more below.
Causes of Heel Spurs
The primary cause of heel spurs is repetitive stress to the foot, which can lead to the formation of bony growth on the heel bone. Microtears typically cause the initial onset of heel spurs due to the repetitive stress associated with standing upright and weight-bearing. These microtears can be caused by the following:
Plantar fasciitis
Plantar fasciitis is the top contributor to heel spurs. The condition involves inflammation and irritation of the plantar fascia, leading to pain and swelling in the heel.
Flat feet or high arches
Flat feet or high arches are two foot conditions that can stress the heel more, leading to heel spur formation.
Excessive weight or obesity
Being overweight puts additional stress on the feet and can increase the risk of developing heel spurs.
High-impact sports
High-impact activities like running, ballet, or jumping can put added stress on the feet. Over time, repeated impact to the foot and heel can lead to heel spur formation.
Inadequate footwear
Improper footwear can stress the heel and lead to heel spurs over time. For instance, wearing worn-out shoes, using footwear for which it's not designed, or wearing footwear unsuitable for your foot type.
Symptoms of Heel Spurs
There are a few telltale signs of heel spurs with symptoms entirely isolated to the heel of the foot. Symptoms include:
Pain in the heel, especially with walking or running
Tenderness and swelling in the heel area
Redness or warmth in the heel area
A bony protrusion on the heel bone, which may feel like a bump or be visible through X-rays
You may experience numerous symptoms or just a single symptom of heel spurs, depending on how long you've experienced discomfort. The treatment method should match the level of symptoms you experience.
How to Treat Heel Spurs?
Heel spur treatment addresses the condition's underlying cause and may include rest, stretching exercises, footwear changes, orthotic devices, medications, physical therapy, or surgery. If you are experiencing heel spur symptoms, seeking medical attention for proper diagnosis and treatment is essential.
Learn more about some of the more common treatment options for heel spurs below:
Rest and ice
The number one treatment method for heel spurs is resting and icing in the initial stages. Resting the affected foot and applying ice can help to reduce inflammation and pain.
Stretching exercises
Stretching exercises can help to loosen the plantar fascia and reduce stress on the heel. You may find relief in stretching the calf muscle, which reduces the load and stress on the foot and heel. Specifically, tight gastrocnemius, soleus, and other posterior leg muscles are common in plantar fasciitis patients. Here are eight practical heel spur stretching exercises you can perform at home.
Footwear changes
Proper footwear can help reduce heel stress. Wear shoes with good arch support and adequate cushioning. It would help if you also chose your footwear according to how you use them. For instance, buy and use running shoes for running. Buy and use work boots for the job. Footwear should meet the demands of the activity, which can help protect your feet and keep them healthy.
Custom orthotics
Custom orthotics can help to support the foot and reduce stress on the heel. The goal of orthotics is to redistribute weight and load away from the heel specifically.
Physical therapy
Physical therapy focuses on strengthening the muscles and tissues in the heel and the foot. A more balanced foot allows muscles to work together in unison without overstressing the heel.
Surgery
As with bone spurs, the only removal method is surgery. As such, once all conservative measures above are exhausted then surgery may be an option in more severe cases of heel spurs to remove the bony outgrowth entirely, which can help repair damage to the surrounding tissues. This would require a referral from a family doctor.
March 13, 2023
Arch pain is among the most common forms of foot discomfort. It can be particularly uncomfortable because of how critical the arch and heel are to the foot. The arch is the supporting foundation of our feet and appropriately resembles the shape of an aqueduct. Given the daily demands of life, it's easy to see how these structures can become overworked and damaged. The most common cause of arch pain and heel pain is a condition called plantar fasciitis.
Keep reading to learn about the most effective plantar fasciitis treatments, including shockwave therapy, custom orthotics, and pain management solutions, to help you conquer the pain of plantar fasciitis for good.
What is plantar fasciitis?
Plantar fasciitis is when you experience pain or discomfort in the heel and underside of the foot - including the arch. Inflammation or irritation of the plantar fascia, a thick band of tissue that extends between the heel bone and the arch, triggers plantar fasciitis.
Symptoms of plantar fasciitis may include:
Pain in the heel or underside of the foot. Pain may peak in the morning or after prolonged periods of standing or walking.
Stiffness and tenderness in the foot.
Swelling or redness in the foot.
Difficulty walking or standing for long periods.
What causes plantar fasciitis?
Plantar fasciitis is a common condition, especially among athletes and people who spend long periods on their feet. Understanding the source of your plantar fasciitis can help determine the best plantar fasciitis treatments for you. Causes of plantar fasciitis include:
Overuse: Repetitive activities that stress the plantar fascia, such as running, jumping, or standing for long periods, can overwork the plantar fascia, leading to inflammation and pain.
Lower leg biomechanics: Some foot structures can stress the plantar fascia and increase the risk of plantar fasciitis. Flat feet or high arches, for instance, may cause plantar fasciitis by adding stress to the muscle group.
Footwear: Improper footwear that (1) doesn't provide enough arch support, (2) doesn't have enough support or cushioning, or (3) doesn't fit properly can all contribute to plantar fasciitis.
Age: Plantar fasciitis is common in people over 40, as the plantar fascia loses elasticity and becomes more prone to injury with age.
Medical conditions: Obesity, diabetes, and osteoarthritis can increase the risk of plantar fasciitis.
Tight or weak muscles: Tight muscles in the calf or foot can put extra stress on the plantar fascia, leading to inflammation and pain.
Weight: Sudden weight gain can add stress to the plantar fascia before your body acclimatizes to the high support requirement.
The causes of plantar fasciitis can vary from person to person, and a combination of factors may contribute to the development of the condition. Consulting with a healthcare professional, such as a chiropodist or podiatrist, can help identify the underlying causes of your plantar fasciitis and guide appropriate treatment.
What are the effective treatment methods for plantar fasciitis?
There are many effective treatments for plantar fasciitis. Depending on the severity of the condition, you can treat the pain and discomfort yourself or be better off seeing a foot specialist. We recommend the following treatments for plantar fasciitis:
Rest
In the short term, reducing activities that aggravate heel pain—such as prolonged standing, running, or walking on hard surfaces—can help reduce irritation and prevent symptoms from worsening. So yes, rest can be useful in the early stages.
That said, too much rest may actually slow recovery. Plantar fasciitis is typically related to strain and tightness in the foot and calf structures, so the goal is not complete inactivity, but rather load management while gradually restoring normal function.
Ice
In the short-term, when symptoms first appear, applying ice to the affected area can help reduce pain and swelling. You can freeze a water bottle, and rest your foot on top of it while sitting. The cold therapy reduces inflammation.
Footwear modifications
Wearing supportive shoes or inserts can help reduce stress on the plantar fascia and improve foot biomechanics. You should also remove ill-fitting footwear from your closet. Instead, choose one of our best shoes for plantar fasciitis relief.
Physical therapy
Physiotherapy and massage therapy effectively treats plantar fasciitis if you prefer not to DIY. At home, you can self-massage by rolling a tennis ball or frozen water bottle under the foot. Self-message strengthens the foot arch muscles and relieves tension in the inflamed plantar fascia.
Stretching and strengthening are also critical parts of plantar fasciitis treatment. Towel stretches, calf stretches, tennis ball rolls, and marble pickups can help strengthen the arch and heel. Find out how to effectively do plantar fasciitis exercises here.
Shockwave therapy
This non-invasive innovative treatment delivers high-energy sound wave pulses to the affected area. It triggers your body's natural healing response to repair the plantar fascia and reduce pain. Shockwave therapy is scientifically proven to be a highly effective treatment for plantar fasciitis pain persisting longer than six months.
Custom orthotics
Custom orthotics and orthopedic shoes support the arches of your feet and reduce stress on the plantar fascia. Both also encourage proper heel-to-toe gait, which, combined with arch support, can prevent a recurrence.
Taping
Taping isn't just for sports. Elastic therapeutic taping techniques may prevent unwanted movements that increase strain on the plantar fascia. For example, research finds that “in the short-term, taping is beneficial in treating plantar fasciitis. The best evidence exists for low dye taping and calcaneal taping.” Behind-the-scenes, taping provides stability and structure to the muscle group. Our chiropodists at Feet First Clinic can skillfully and therapeutically tape the feet and toes to treat and prevent a variety of foot conditions and deformities.
Support Slippers
Supportive slippers are helpful for Plantar fasciitis because they reduce strain on the plantar fascia during everyday activities at home, where many people often walk barefoot on hard surfaces without realizing the impact. They provide arch support and cushioning, which helps decrease the pulling force on the plantar fascia with each step, especially during the morning or after periods of rest when the tissue is typically more stiff and sensitive. Supportive slippers also help distribute pressure more evenly across the foot, reducing stress on the heel, while their shock-absorbing properties protect against the impact of hard indoor flooring like tile or hardwood. Overall, they help keep the foot in a more supported, biomechanically stable position throughout the day, which can reduce pain flare-ups and support recovery over time.