July 22, 2024
Sometimes with aging feet comes the development of toe deformities, particularly hammertoes. Studies show that approximately half of women over 70 have some version of a toe deformity (but they can happen to anyone). Many assume correcting hammertoes always leads to a daunting surgery, but guess what? Surgery is not usually the first option and is generally only considered when the toe becomes rigid, or other complications arise. Read today’s article to discover the best non-surgical solutions for hammertoes and toe alignment techniques that achieve amazing results.
Top Hammertoe Treatment Options
Innovation in foot care and toe straightening methods have lead to plenty of non-surgical solutions for hammertoes and the pain they cause, including:
Splinting, taping and bracing
Custom orthotics and new footwear
Shockwave therapy
At-home exercises
Other treatments
Splinting, Taping and Bracing
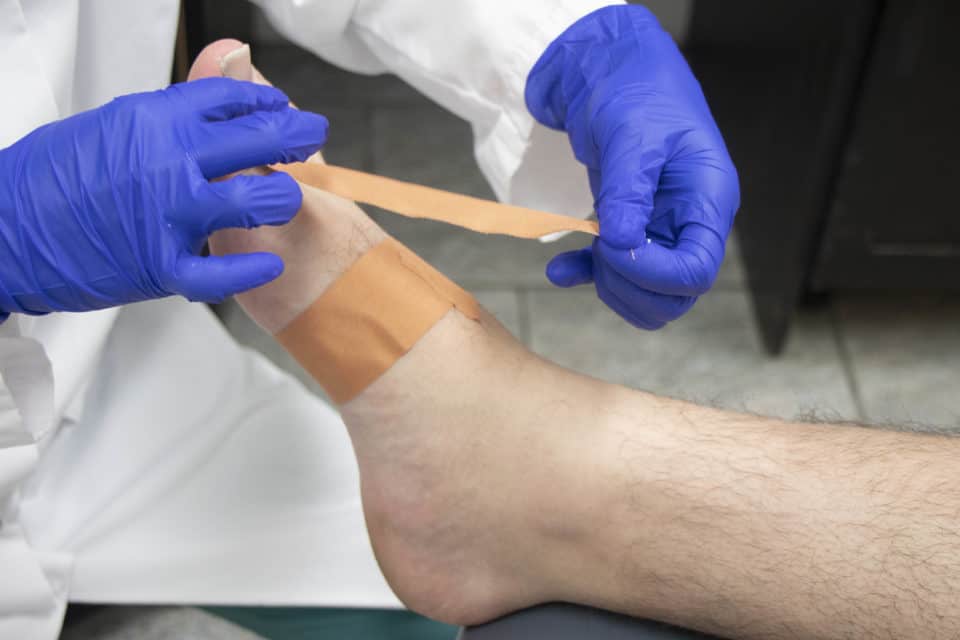
These non-invasive tools are great for dealing with toe curvature. All performed by a licensed Toronto chiropodist, splinting, taping and bracing helps straighten flexible toe deformites, reduces friction and discomfort (corn development is common for people with hammertoes) and provides support and alignment when used daily.
Custom Orthotics And Footwear Changes
Custom orthotics are all about placing each part of your foot where it’s supposed to be, including toes. Wearing orthotics can properly align the joint in your toe and relax the burden on the affected tendons. Most importantly, they'll offset and redistribute pressure away from the toes. This will reduce strain on the hammertoes when you walk, which will help prevent them from getting worse.
As for footwear, avoid high heels if you have any toe deformity; they’re notorious for making hammertoes worse. Wear wide shoes, maybe even orthopedic shoes, that allow your toe abnormalities to exist comfortably and reduce pain as much as possible. Most importantly, make sure your shoes fit: If your shoes are too short, your toes will curl, which will make your hammertoes worse. (In fact, ill-fitting footwear is a major contributing factor to hammertoes.)
Shockwave Therapy
It’s clear that when you have hammertoes, your joints and tendons take a hit. Toe deformities can indirectly cause irritation and inflammation in the surrounding muscles and ligaments due to altered pressure and biomechanics in the feet and joints. If there is associated tightness or inflammation in nearby areas—such as the ball of the foot or arch—shockwave therapy may be beneficial in reducing symptoms and promoting healing.
At-Home Exercises
Check out exercises and stretches that help treat the top of the foot to soothe your hammertoes and strengthen your feet and muscles in general. Many of these target the toes and surrounding area. Strengthening the muscles in your feet ensures that the toes and joints don't get overworked or strained when you walk, which helps manage hammertoes and provides hammertoe pain relief.
Over-the-Counter Products
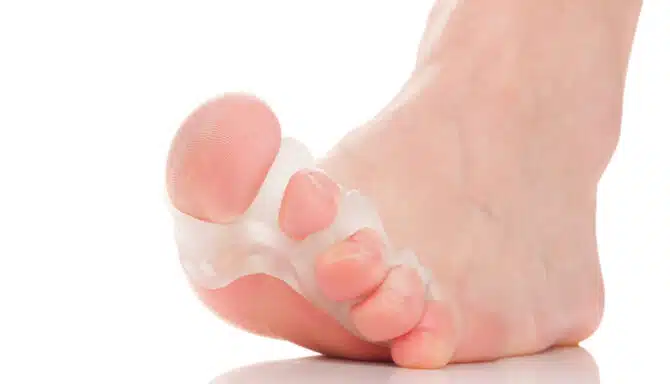
Gel separators, toe spacers, pads, cushions and more can help you take control of your hammertoes without resorting to surgery. Call your local Toronto foot clinic to see what they have in stock!
October 21, 2023
Runner's knee is a condition that causes pain around the front of the knee, particularly near the kneecap. Don't let the name fool you: runner's knee doesn't just affect runners. Individuals who engage in repetitive knee-bending activities, such as cycling, jumping, or squatting, can experience this form of knee pain. The condition is characterized by discomfort or pain often felt during and after physical activities.
Whether you're a seasoned marathoner or lacing up your running shoes for the first time, understanding the ins and outs of this common ailment is helpful for preventing and managing its onset.
In this comprehensive guide, we'll delve into runner's knee – its causes, symptoms, prevention strategies, and rehabilitation techniques – to ensure that you stay pain-free and on your feet.
Runner's knee: What is it?
Runner's knee, formally known as patellofemoral pain syndrome (PFPS), is a condition characterized by pain around the front of the knee. Any activity that repeatedly stresses the knee cap or the areas around the knee cap can aggravate the condition. It is more common in women than men. This is believed to be due to a greater susceptibility to knee misalignment in women.
Runner's knee symptoms include:
Pain around the knee cap, especially during activities that involve bending the knee, such as running, walking downstairs, or squatting.
Pain after prolonged sitting and a stiff feeling in your knee
Cracking or popping sensation
Swelling and inflammation in and around the patella
What cause's runner's knee?
Many causes of runner's knee are not specific to the knee, but rather are abnormalities with the surrounding muscles and joints. Because the knee is a hinge joint, it relies on many different parts of the leg to properly perform its job.
Common causes of runner's knee are:
Misalignment of the patella: Improper tracking of the patella can lead to increased pressure on the joint.
Muscle imbalances: Quad, hip, and knee imbalances can lead to biomechanical deficiencies that overexert the knee.
Overuse: Repeated knee bending and straightening during activities can cause excessive stress on the patellofemoral joint, leading to irritation and pain.
Poor biomechanics: Issues with how the lower extremities function during movement, such as flat feet or overpronation, can contribute to developing a runner's knee.
Inadequate warm-up or stretching: Failing to properly warm up before exercise, or neglecting to stretch, can increase the risk of developing PFPS.
Too much, too soon: A sudden increase in activity level, such as increasing mileage or intensity too quickly, can strain the knee joint and lead to a runner's knee.
Inadequate footwear: Improper footwear that does not provide adequate cushioning and support can contribute to knee pain.
How do I treat runner's knee?
There are several ways of treating a runner's knee. First and foremost, understanding the cause(s) will help you get back to being healthier faster. Common treatments include:
Rest and ice: Give your knees time to rest, and apply ice to reduce inflammation and pain.
Reduce intensity: Reduce or stop the physical activity that could be causing the pain. Alternatively, reduce all activity while you consult a professional to diagnose the exact cause, at which point you can slowly re-introduce physical activity. You can also try low-impact activities such as swimming or cycling to maintain fitness while giving your knees a break.
Physical therapy: Physiotherapy, massage therapy, and a strength program can help strengthen the muscles around the knee and improve biomechanics. Engage in exercises stretching and strengthening the quadriceps, hamstrings, hip, and calf muscles.
Orthotics and proper footwear: Custom orthotic inserts or appropriate footwear can help correct biomechanical issues contributing to the condition. A shoe fitting and video gait analysis can help reveal any biomechanical deficiencies and provide a helpful guide into choosing the right shoe.
Patellar taping: Taping techniques can help reposition the patella and reduce pain during activity.
When to see a chiropodist for a runner's knee?
If the pain persists despite conservative treatments, consult a healthcare professional like a chiropodist for a proper diagnosis and personalized treatment plan. Addressing the runner's knee early is essential to prevent further complications and ensure a timely recovery.
April 20, 2023
Since women are more likely to experience foot pain and conditions, a significant focus of women's health should always be foot health. According to Foot Health Facts, narrow footwear that cramps the forefoot and squeezes the toes is the primary reason women are prime targets for foot health issues. Furthermore, common foot problems in women can arise after years of wearing shoes with little arch support and unstable heels. Today's article will discuss the most common foot problems women struggle with and prevention and treatment options.
Common Foot Problems in Women
Bunions
Plantar fasciitis
Arthritis
Hammertoes
Plantar Fasciitis
Medical News Today notes women risk developing plantar fasciitis more than men. This may be due to post-pregnancy foot changes and the effects of wearing unsupportive footwear for years; both can lead to plantar fascia strain and subsequent stabbing heel pain. The best way for women to prevent and treat this painful condition is to only wear high heels on special occasions and choose comfortable heels with cushioning and a stable heel. For daily activities, opt for shoes with sufficient arch and heel support (most important) and thick soles and cushioning. But it's also important to find shoes with that create a healthy environment for your feet (i.e.: enough room in the toe box, breathability, etc.) to prevent other conditions.
Maintaining a healthy weight can also prevent too much pressure on the plantar fascia. To help, women can stretch their feet and perform daily exercises that work the plantar fascia and calf muscles (see an example below!). And lastly, orthotics with arch support can distribute the pressure on your feet more evenly.
Bunions
Low-quality footwear is a contributing factor in the development of bunions in women, but genetics can also play a significant role. One of the main structural contributors is low arches or flat feet. This foot type often leads to improper alignment—specifically overpronation—which places excessive pressure on the big toe joint. Over time, this added stress can cause damage and lead to the formation of a bunion at the base of the big toe. Bunions may also be at their worst during menopause or pregnancy.
Some women may require surgical intervention to correct severe bunions, but many can manage their symptoms with non-invasive treatments. Options such as bunion pads, supportive inserts, custom orthotics, and regular rest combined with compression and ice can help reduce discomfort. Orthotics are especially important, as they address underlying biomechanical issues that place excess strain on the joint at the base of the big toe, helping to redistribute pressure more evenly. This can go a long way in slowing the progression of a bunion. Another key preventative measure is choosing proper footwear—shoes should provide adequate support and have a wide toe box to avoid crowding. Since cramped toes are a major risk factor, avoiding narrow or tight-fitting shoes is essential for long-term foot health.
Arthritis
Research suggests post-menopausal women suffer more from osteoarthritis than men because of estrogen fluctuations. There may be a connection between pre-menopausal estrogen levels and joint and cartilage health.
Targeted exercises are one of the best ways to prevent and treat most types of arthritis (not just osteoarthritis!). Moreover, Feet First Clinic's beginner's guide to exercises for arthritis Part 1 and Part 2 outline beneficial exercises, the steps involved and why they're so useful. These routines also consider that arthritis can be very limiting and ensures all movements are manageable. Other forms of treatment include braces or canes (in severe cases), anti-inflammatory pain relievers, orthotics that support the ankle and the foot (also good for prevention), physiotherapy and orthopedic footwear.
Hammertoes
Like bunions, hammertoes affect women because they are more likely to wear excessively tight and unsupportive shoes, causing the toes' middle joints to bend more and more over time.
To avoid and manage pre-existing hammertoes, ensure your shoes have at least half an inch of room between the toes and the end of the shoe. Additionally, women should avoid high heels on most days and only wear them if the heel is a "reasonable" height. It may also be wise to buy shoes with stretchy fabrics and avoid excessive fabric layers. They can force your toes into uncomfortable positions and make it difficult to accommodate pre-existing hammertoes. Inserts and pads can also be helpful for women by positioning the toes and feet more favourably. Furthermore, a chiropodist or podiatrist can use a splint or some tape to fix your toe in the proper, straight position.
If the hammertoe is flexible, meaning that it can be straightened manually, a flexor tenotomy may also be an option. This is a non-invasive surgical procedure whereby a chiropodist loosens the tendon that is causing the toe to curl.
Several medical devices can help with toe conditions
February 9, 2023
Toe pain can be mysterious. There are numerous causes, and sometimes you can live your life assuming you know why it's there, only to be completely wrong! Case in point: a lesser-known toe condition called capsulitis.
Capsulitis is an overuse injury that mainly targets the second toe and the surrounding area. Today we'll thoroughly dive into the topic by addressing the following:
What is capsulitis?
Symptoms of capsulitis
Causes of capsulitis
Treatment and prevention
Complications
What is Capsulitis?
Capsulitis, also known as frozen toe, hallux rigidus or turf toe, is a foot condition characterized by joint inflammation in the area where the base of the toe meets the ball of the foot. The specific area affected is called a "capsule" and is technically a dense ligament structure found at the base of the joint. According to the American Academy of Orthopaedic Surgeons, capsulitis in the feet usually targets the second toe. However, it can sometimes affect the big toe and the third and fourth toes. Another technical term for capsulitis in the toe is metatarsophalangeal synovitis (MTP joint pain).
Healthline also notes that capsulitis is often confused with Morton's Neuroma since pain radiates toward the ball of the foot in both conditions. However, Morton's Neuroma results from compressed nerves and capsulitis from inflammation. A chiropodist can help you tell the difference between the two conditions.
Symptoms of Capsulitis
Capsulitis often worsens as time progresses. This means that symptoms can vary depending on the stages of development. It's important to be in tune with your foot health and seek help if you notice the following:
Pain in the ball of the foot.
A persistent feeling that something is "bunched up" in your shoe or the feeling that you're walking on a pebble or marble.
Swelling in the base of the affected toe.
Discomfort while wearing shoes.
Pain that worsens when you're barefoot.
Crossover toe: as degradation of the ligament progresses, the joint in the second toe can fail to stabilize (stay in the right position). This can cause your second toe to move towards the big toe and lay on top of it.
What are Some Causes of Capsulitis?
Capsulitis is technically an overuse injury that targets the ball of the foot. And as with many foot conditions, one issue can often be a risk factor in developing another.
The following may lead to capsulitis development:
There is a connection between severe bunions and capsulitis. Other prominent foot deformities like hammertoes can also be a risk factor. Both conditions can lead to too much pressure on the ball of the foot and subsequent inflammation.
Abnormal foot mechanics can put you at risk. It's important to note that this is not the same as a severe foot deformity. It simply means any mild structural factors that lead to excessive weight-bearing pressure in the ball of the foot underneath the toe.
If your second toe is longer than your big toe, you may experience capsulitis.
An unstable foot arch, like high arches and flat feet, can contribute to capsulitis.
Excessive bending of the toes. This can happen if you wear poorly designed shoes or high heels.
Capsulitis Treatment and Prevention
It's relatively easy to tackle early-stage toe capsulitis. You can purchase many items from a pharmacy, general store or foot clinic that can relieve the pain. A chiropodist can also use their unique expertise to ensure the condition improves.
Here are some effective treatment methods:
Ice or heat packs. Compression can help reduce swelling, and applying heat or ice (while resting with your foot elevated) can help with pain management.
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen.
Supportive footwear with proper arch support and strong soles. Rocker bottom-sole shoes can be especially helpful as they offset pressure away from the ball of your foot.
Custom orthotics can lessen excessive pressure on the weight-bearing foot areas.
Toe taping can align the second toe and prevent crossover toe.
Complications
Unfortunately, if crossover toe is present, it usually means that the second toe will never revert to its natural position without intervention. If this is the case, you may need surgery from a foot and ankle surgeon.
November 10, 2022
Your plantar plate plays a critical part in the anatomy and makeup of our feet. The plantar connects your feet with the joints in your toes.
Given the constant wear and tear of your feet, the joints and muscles can often become overworked or strained. The plantar plate is particularly susceptible to injury because of its location on the foot. This also makes it especially vulnerable to several other foot conditions. For example, having bunions or a hammer toe may increase the risk of a plantar plate tear.
But worry not. In this article, learn more about the plantar plate as a body part, plantar plate tear symptoms, causes, and treatment methods for the foot condition.
First, let's explore the physiology of the plantar plate itself.
What's your plantar plate?
The plantar plate is rigid fibrocartilage (a dense, whitish tissue with a distinct fibrous texture) which connects the phalanges to the metatarsal head. In other words, the plantar plate joins the toes (phalanx bones) with the forefoot (metatarsal bones). As the mediator, the plantar plate stabilizes the toes and prevents them from shifting side-to-side or overextending.
Next, let's look at the why of plantar plate tears.
Plantar plate tear: Causes
Overloading the metatarsophalangeal (MTP) joint is the most common cause of plantar plate issues. Overloading the MTP joint leads to strains and tears. The result? Pain and instability of the plantar plate.
In most cases, plantar plate damage occurs incrementally over time. However, you can acutely injure the plantar plate.
Plantar plate tear causes include:
Bunions: Bunions - a deformity affecting the joint that connects the big toe to the foot - put pressure on the plantar plate by forcing the big toe to push against the 2nd toe.
Biomechanical abnormalities (metatarsal length): If your 2nd metatarsal is longer than your 1st (which it often is), you're at a greater risk of a plantar plate tear at that site. This is because your 2nd metatarsal bears more weight than the "big" toe (1st metatarsal) when it's longer; however, the second toe was not designed to absorb this extra weight, which makes the surrounding region more injury prone.
Biomechanical abnormalities (overpronation): When you overpronate, your foot bears much impact when running or walking. Typically, flat feet are a leading contributor to overpronation.
Cortisone injection: Cortisone shots can have the side effect of thinning and weakening the plantar plate ligament.
Specific activities/sports: Sports or movements that put excessive pressure on the toes and ball of the foot increase your chances of developing a plantar plate tear. Be cautious when dancing, running, jumping, or climbing stairs, especially if the balls of the foot are regularly sore or sensitive.
Hammertoes: A hammertoe deformity occurs when the toe's middle joint bends abnormally a toe deformity in which the middle joint in the toe bends abnormally.
In the next section, you'll learn how to recognize plantar plate tears.
Symptoms
Wonder what are the signs of a plantar plate tear? Well, look out for these symptoms commonly associated with plantar plate tears:
Toe alignment changes: The toe changing position, which occurs gradually as the tear increases, usually to the side or upwards
Pain: Discomfort usually stems from the ball of the foot, either as severe pain or a dull ache. If you find you're walking with very little cushioning under your toes, it may be because of a plantar plate tear.
Swelling: You may notice swelling underneath the ball of the foot extending between the start and end of one of the multiple toes.
Plantar plate tear: Diagnosis
You have a few options in terms of diagnosis:
Treat the pain yourself if it's not severe and the discomfort has just begun
X-rays
MRIs
Finally, in the last section, you'll learn more about how to treat plantar plate tears.
Plantar plate tear: Treatment
Pinpointing a plantar plate tear as the source of discomfort can be challenging. The foot is a complex network of muscles, tendons, and bones that are so intertwined that isolating the condition can be difficult. However, it's not a hopeless task.
Several DIY treatment methods exist for mild symptoms, as well as options for severe cases of plantar plate tears.
Visit a chiropodist or podiastrist
Our team of licensed chiropodists is committed to providing quality care and services for all your foot and ankle needs. They can diagnose, treat and help manage various foot conditions, from callus removal to ingrown toenails to bunions. Most importantly, through a biomechanical assessment, they can determine the underlying cause of your plantar plate tear and then make recommendations to reduce pressure on the area and correct any faulty biomechanics that are putting extra strain on the plantar plate.
PEACE & LOVE
The PEACE & LOVE recovery method is a modern approach to managing soft tissue injuries that balances early protection with a gradual return to movement. PEACE focuses on the first phase after injury: Protection (avoiding aggravating activities), Elevation (reducing swelling), Avoid anti-inflammatory modalities that may interfere with natural healing, Compression (to control swelling), and Education (understanding the injury and avoiding over-treatment). After the early phase, LOVE guides recovery: Load (gradually reintroducing movement and exercise), Optimism (supporting a positive mindset, which can influence outcomes), Vascularization (light aerobic activity to promote blood flow), and Exercise (progressive strengthening and mobility work). Together, this approach encourages appropriate early care while promoting active recovery rather than prolonged rest.
Taping
Taping, the wrapping of a joint for added stability, can help hold your toes in position. Stabilizing the joint with tape can help correct any worsening abnormalities associated with plantar plate tears. It also prevents your toes from moving too far side-to-side, which can help encourage plantar healing and to avoid re-aggravation. A chiropodist or podiatrist can perform splinting, bracing, or taping for you.
Orthotics
Orthotics are a treatment method for the underlying causes of plantar plate tears. Custom foot orthotics are effective for bunions, hammertoes, and flat feet. You can also use shoe inserts with hardened plastic under particular toes for extra support.
NSAIDs
Anti-inflammatories like ibuprofen or Advil can combat pain associated with plantar plate tears.
Surgery
Surgery is a last resort option for plantar tears. There are two standard surgical procedures for plantar tears. The hat-trick procedure helps realign the metatarsal bone, while other surgeries are available for associated conditions like hammertoes, bunions, or other ancillary operations to balance the toe.
October 17, 2022
Everybody has foot pain from time to time, right? Surely it must be normal to experience foot pain that comes and goes? Especially at the end of a long day or whilst walking?
Actually no. The main causes of foot pain that comes and goes has to do with inflammation and ultimately: Your body is trying to tell you that there is something wrong.
Here's some of the facts and fiction that you might have heard about foot pain that comes and goes:
Walking through pain does not make things better or "loosen up" the area
Foot pain that comes and goes is called acute pain. It is not with you all the time. Sometimes it can be at the start or end of the day. Sometimes it can be with certain exercises or work environments.
Because the pain disappears most people will carry on doing the same activity. Then all of a sudden that pain quickly comes back, maybe a little worse. Then it subsides again...but it then comes back.
Foot pain, therefore, is not normal. If you were free from foot conditions, you wouldn't be experiencing nagging pain that subsides only to flare up later.
Whether it's a pain in the top of the foot, heel pain, or ball of the foot pain, some common sites of foot pain can interrupt your day by reappearing when you thought you were feeling better. And even though they may not be as severe as conditions that cause constant discomfort and foot pain, you'll be glad you sought treatment in the long run.
Furthermore, many foot issues get worse if you choose to ignore them. So pain that comes and goes now may stick around all day long in the future.
Let's look at the common causes of foot pain to fade and return.
The 5 Common Causes Of Foot Pain That Comes and Goes
Plantar Fasciitis
Metatarsalgia
Morton's Neuroma
Injuries
Tendonitis
Plantar Fasciitis
https://youtube.com/shorts/rSKd2ztKWa8?si=wX4eVJ_3pEpBscds
Plantar fasciitis is somewhat notorious among foot conditions. It ranks as one of the top causes of heel and arch pain and targets people with varying lifestyles. It is also one of the prime suspects for causes of foot pain that comes and goes. You can read more about it here. It is a very common condition and when caught early it can be calmed down quickly. Some of the main causes are:
Foot shape
Floor materials
Tight muscles
Excessive weight
Inappropriate footwear
Overuse
The heel pain stems from the inflammation of the plantar fascia, which is a band of tissue that runs along the arch and connects the heel bone to the toes. Constant pulling (of the fascia on its insertion point at the heel bone or toes) and contact trauma (when your heel comes into contact with the floor) cause inflammation and pain.
Why does the pain come and go?
Inflammation chemicals are created when the fascia is under strain or is being traumatized. This why it becomes sore. When you are at rest you obviously don't get the pain. But, those inflammation chemicals are still being generated and they build up. When you put your foot down to start to walk again (like those first few steps of the day) the foot can be quite painful. It is only when you then walk some more that those chemicals start to dissipate.
Of course, it's important to seek treatment even if the pain fades for several intervals during the day; if you don't, it can get much worse and become chronic.
Metatarsalgia
Do you have pain in the ball of the foot that comes and goes? Metatarsalgia may be the culprit.
Like plantar fasciitis, inflammation of the metatarsal area (the area between the toes and arch) causes metatarsalgia. Not only is this condition difficult to pronounce, but it can make walking downright unbearable. The same risk factors of plantar fasciitis apply, in addition to wearing ill-fitting footwear and performing physical activity that involves running and jumping.
Why does the pain come and go?
Metatarsalgia feels worse when you flex your foot, walk, run or simply stand (especially barefoot). The foot pain will then fade during rest periods.
Again, when inflammation is the reason behind intermittent pain, it will not bother you 24/7. Metatarsalgia is no different, but if you ignore it, the condition may worsen, causing radiating pain to other parts of the foot, the hips and the lower back. This is caused by your body attempting to accommodate the pain by walking differently, which then strains other body parts.
Morton's Neuroma
Sometimes nerve problems are a main cause of foot pain. Your feet are full of these tiny yet very important structures.
Morton's Neuroma affects the ball of the foot, specifically the area between the 3rd and 4th toes. The pain is accompanied by a burning sensation and a nagging pressure, and it can feel like you have an invisible pebble in your shoe. But it's also known to radiate to the top of the foot, causing intermittent stabbing pain.
Your toe nerves run between the balls of your feet. If the foot becomes compressed, those bones press upon the nerves even more. As the nerves becomes irritated and traumatized they give off pain signals. The most common reasons for nerve irritations are:
High heels
Narrow footwear
Foot deformities like hammertoes and bunions.
Why does the pain come and go?
Morton's Neuroma pain is generally intermittent, but when you irritate the nerves, you'll notice the pain is back in full force.
The symptoms will flare up if you continue to walk in the same tight shoes that triggered the problem in the first place. Likewise, if you spend a long day on your feet, the pain will be much more challenging than on a day of lounging and relaxation. Over time, the nerves start to thicken and then the pain can be quite bad. With Morton's (or any nerve compression) it is wise to seek treatment early to reduce the risk of nerve trauma.
Injuries
A foot injury is a broad term for many scenarios, from dropping a heavy object on the top of the foot to a full-blown ankle sprain or stress fracture. Technically, many foot conditions can be considered injuries - even plantar fasciitis. But for simplicity, let's discuss more sudden traumatic injuries instead of those that cause inflammation or degradation over time.
Why does the pain come and go?
When you first suffer from an injury, the pain will likely be acute and bother you consistently, even while resting. You might see the area become bruised and swollen
But foot pain from an injury can transform into a pain that comes and goes when you start to heal. Even though most moderate injuries heal within a month, light activity will trigger pain as you slowly get back to normal. Generally, you must stop any activity if you experience sudden, sharp pain while healing from an injury.
There are many different foot injuries that can cause foot pain that comes and goes:
Some of these traumas can be fractures
Some can be cuts to the skin after it has been traumatized that you might not be able to feel
Infection signs can also come and go and not be constant
It is therefore important to speak with a foot specialist and your family doctor first about managing intermittent pain after an injury.
Tendonitis
Achilles tendonitis causes a dull ache directly above the heel or on the back of the leg, and extensor tendonitis causes the same feeling on the top of the foot. They both result from inflammation and overuse of their respective tendons: the Achilles tendon (the tendon that connects the back of the calf to the heel bone) and the extensor tendons (the tendons that run along the top of the foot).
Athletes are the most vulnerable, as these are repetitive strain injuries that arise after vigorous physical activity. When you bear weight on your toes and feet, you're putting these tendons to work, making them more susceptible to strain.
It is also wise to check with your Doctor or foot specialist to assess whether tendonitis is causing your foot pain before you start any treatment. Why? Some conditions can look like a tendon issue but they are not. Pain on the back of the leg can be serious. And as we said before, fractures can also be a strong cause of foot pain. This is especially so in high trauma and repetitive trauma jobs and sporting activities. In some sports, tearing and even splitting of the Achilles is not that uncommon.
Why does the pain come and go?
Naturally, the pain will be worse when you use these tendons in any capacity or when you first start to move during the day. But tendonitis can also cause stiffness at the end of the night or first thing in the morning without movement.
Fun fact: the Achilles tendon is not only crucial for performance enhancement, but it's also the biggest and strongest tendon in the human body! So be sure to protect it from additional harm by seeking treatment.
What Can I do About The Causes Of Foot Pain That Comes and Goes?
First, don't let rest periods trick you into thinking your foot pain is gone. Whether it's inflammation, a pinched nerve or any other trigger for the pain, seeking treatment at the start is always the best option. As we have seen, assessing and treating foot pain early is essential to reduce the risk of that pain becoming chronic or creating further foot pain.
Furthermore, a common mistake is assuming that chiropodists are only for severe cases. But several services from a foot clinic are medically proven to provide foot pain relief for those with intermittent discomfort.
Some of the most effective treatment options include:
Custom orthotics
Footwear recommendations and fittings
Superfeet insoles
Shockwave therapy
Exercises and stretching routines
Therapeutic taping
Splints and boot casts
Apart from treating your foot pain, Chiropodists can also show you how to prevent and manage your foot pain so that you can enjoy the activities that you love. And if you have chronic foot pain, the Chiropodist can help:
https://youtube.com/shorts/nt1SgT9xrUM?si=pYtpckRgufkumDV2