Are your feet giving you a hard time? Foot pain can have many causes, including injury, overuse, medical conditions, and poor footwear. The underlying cause will dictate how to treat your foot pain, which can include anything from supportive footwear, to stretching exercises, to rest, to medication.
In this article, we’ll go through six common causes of foot pain and how to treat them:
- Plantar Fasciitis
- Achilles Tendonitis
- Bunions
- Ingrown Toenails
- Osteoarthritis
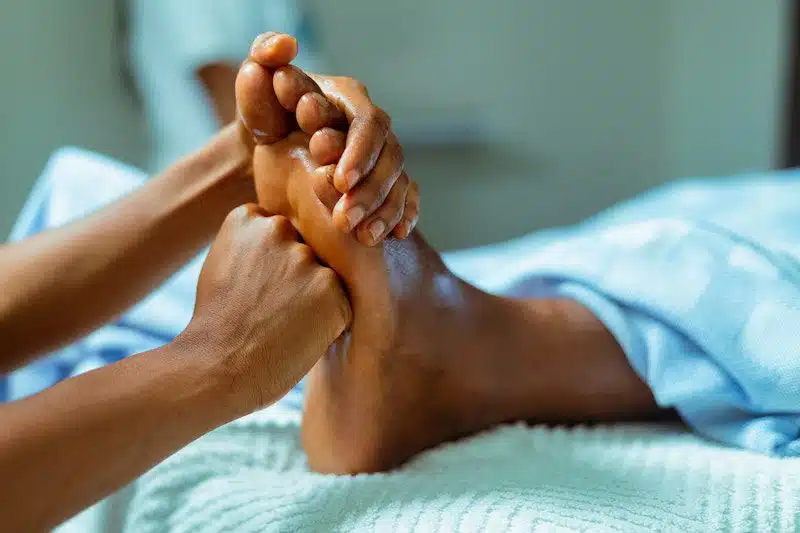
Plantar fasciitis
Causes
Plantar fasciitis occurs when the plantar fascia (the band of tissue that connects the heel bone to the toes) becomes inflamed. It is caused by inadequate arch support or overexerting the plantar fascia. For instance, poorly constructed shoes, obesity and pregnancy, high-impact activity, and long periods of standing (like if you have a standing desk or work in a standing-first occupation) cause strain on the plantar fascia.
Treatment
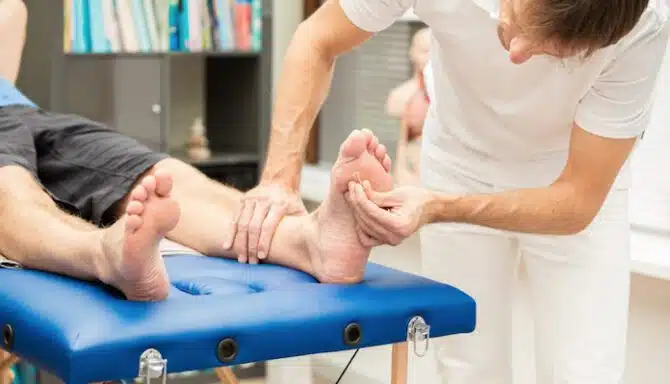
Plantar fasciitis treatment involves rest and recovery, which should be the first course of action. Then physical therapy, like massaging your arch and stretching and strengthening exercises, are effective. Additional treatment methods include shockwave therapy, taping, wearing a splint or boot cast, and custom orthotics designed to provide additional arch support.
Read more: See our complete guide on plantar fasciitis.
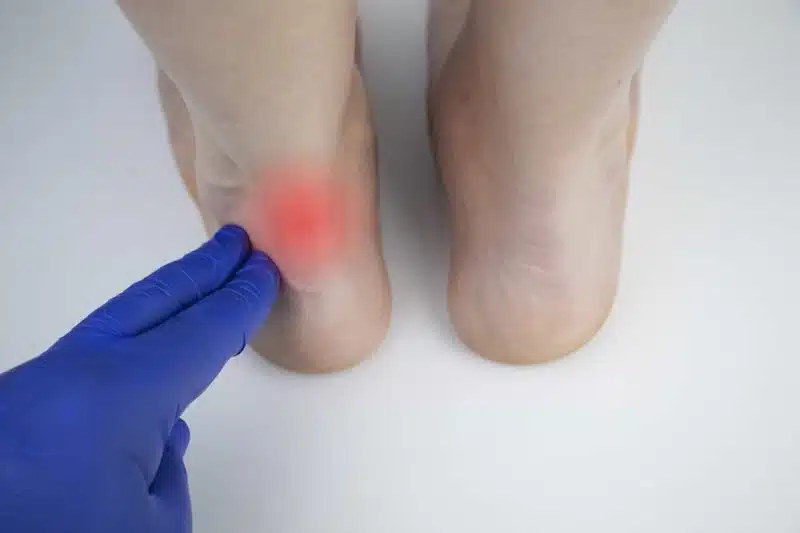
Achilles tendonitis
Causes
Achilles tendonitis is an injury to the Achilles tendon, the part of the leg that connects the calf to the heel bone. It is usually caused by overuse. Overworking the Achilles heel is done through various avenues. The most common causes include overexercising, weight gain, joint disorders like rheumatoid or psoriatic arthritis, bursitis, a sudden fall or past trauma, and biomechanical abnormalities.
Treatment
Within 72 hours of injury, the first form of treatment you should pursue is rest and recovery. Good R&R prevents aggravation and stops the condition from worsening at its most vulnerable. Once you remove the cause, effective treatment methods include shockwave therapy, strengthening and stretching exercises (see our how-to), custom orthotics, and anti-inflammatories.
Read more: See our complete guide on Achilles tendonitis.
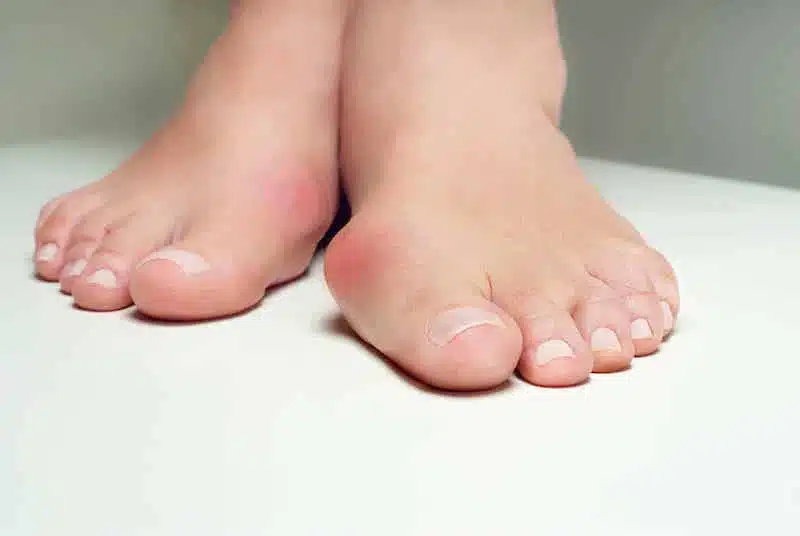
Bunions
Causes
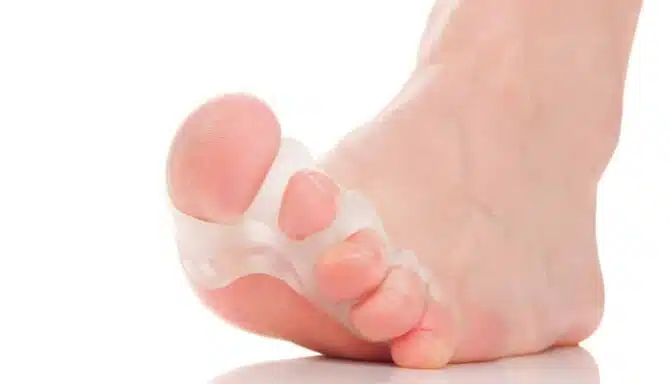
Bunions are a type of joint deformity where the base of the big toe shifts outwards. There is a combination of factors that can either cause, directly or indirectly, bunions. Genetics (namely foot shape or joint-related), tight footwear or high heels, flat arches, and activities that stress the toe base (like running or ballet) can lead to bunions.
Treatment
Treatment options include footwear modification, anti-inflammatories, bunion splints, bunion aligners, taping, shoe stretching, orthotics, shockwave therapy, and surgery. Note that bunions are progressive, meaning non-invasive treatment focuses on preservation rather than reversing damage already done. Surgery is an option if you’d like to remove the bunion.
Read more: See our complete guide on bunions.
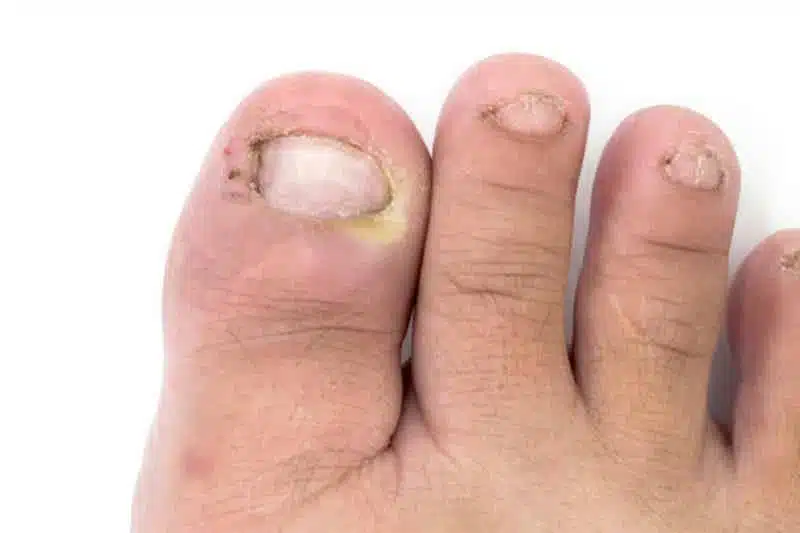
Ingrown toenails
Causes
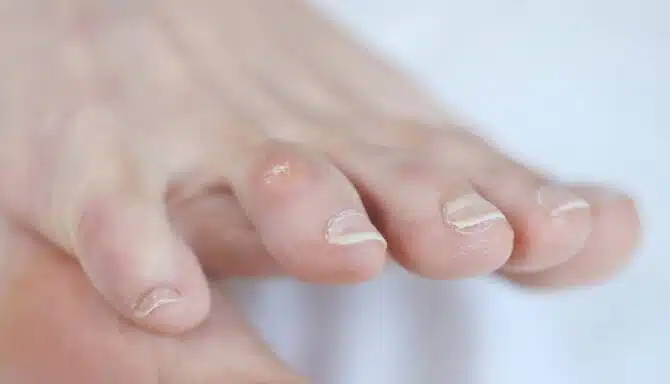
Ingrown toenails occur when the edges of the toenail grow into the skin, causing pain and swelling. Ingrown toenails can be caused by:
- Cutting the nail too short or too far down along the edges
- Poorly fitted shoes.
- Injury to the nail bed.
- A genetic disposition to ingrown toenails.
Treatment
In some cases, you can treat ingrown toenails at home; otherwise a foot specialist can treat the condition. To treat your ingrown toenail at home, soak your foot daily in warm water with Epson salts, massage the skin at the edges of the nail, wear shoes with a wide toe box, and let the toenail grow out. When it does, cut the nail straight across. Never try to cut out your own ingrown toenail as this can lead to infection.
If the toenail doesn’t improve within 3–5 days, it’s time to call the foot specialist. A foot specialist can safely treat ingrown toenails at any stage. In-office ingrown toenail treatment includes antibiotics, softening the skin around the nail, removing or cutting open the area to drain pus, Onyfix nail correction system, partial or complete nail avulsion, phenol, or surgery.
Read more: See our complete guide on ingrown toenails.
Osteoarthritis
Causes
Osteoarthritis is the most common form of arthritis and is caused by wear-and-tear of the cartilage between the joints. Getting old is the most common cause of osteoarthritis. Our joints get more mileage as we age and eventually wear down. Low bone density (for instance, in post-menopausal women) can also lead to osteoporosis, contributing to osteoarthritis (it would be like having defective brake pads). Additionally, unhealed trauma or injury, weakened deconditioned muscles, sudden weight gain, and biomechanical abnormalities like hammer toes or bunions can all lead to osteoarthritis.
Treatment
Treatment of osteoarthritis focuses on management, as it’s a progressive condition. Physiotherapy, stretching, and light exercise to strengthen the muscles in the lower body is vital for managing osteoarthritis symptoms and preventing the condition from worsening. This can be done in conjunction with proper footwear and medication like anti-inflammatories. Custom orthotics can also help by effectively rebalance the weight distribution across your feet while adding support.
Read more: See our complete guide on osteoarthritis.