July 25, 2024
Foot pain can be debilitating, affecting our ability to walk, exercise, and perform daily activities comfortably. One common foot condition that causes discomfort and requires attention is crossover toe.
This blog post delves into crossover toe, its symptoms, and available treatment options. First off, we'll explain exactly what is a crossover toe.
What is a crossover toe?
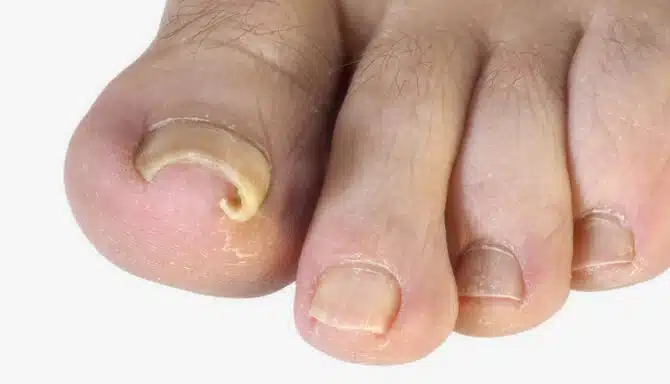
Crossover toe, also known as floating toe or floating fifth toe, is a type of deformity in which the toe drifts out of its normal position and crosses over or under a neighbouring toe. The condition is also known as overlapping toe.
The condition generally affects the fourth and fifth toes, leading to pain, swelling, and difficulty wearing shoes comfortably. However, any combination of toes may become an overlapping toe. Roughly 7% of adults—men and women equally — have overlapping toes of some sort.
Symptoms of crossover toe
Toe pain: Discomfort is often felt at the base of the affected toe, especially when walking or standing for long periods.
Swelling and inflammation: The affected area may become swollen and inflamed due to the abnormal positioning of the toe.
Uncomfortable shoe fit: Shoes may feel tight or uncomfortable, especially in the toe box area where the affected toe rubs against adjacent toes or the shoe itself.
Visual appearance: The affected toe may appear to cross over or under the adjacent toe, giving it a visibly different appearance than the other toes.
Corns: Corns will often form on top of crossover toes due to excessive friction and rubbing on the affected toes.
Causes of crossover toe
Crossover toe can develop due to several factors, including:
Foot injuries: Joint and ligament damage caused by unhealed trauma and foot injuries can change the toes' alignment over time. Additionally, arthritis, including rheumatoid arthritis, can shift the alignment of your toes as it progresses and damages the joints.
Foot structure: People with high arches or flat feet are prone to developing overlapping toes.
Genetics: Overlapping toes may also be inherited. Many conditions that make one prone to developing an overlapping toe, like arthritis and Morton's toe, have genetic contributing factors.
Improper footwear. Wearing shoes that are too short, too narrow or too tight can force the toes into an unnatural position and curl up, which will ultimately lead to the development of a crossover toe.
Treatment options for crossover toe
Footwear adjustments: Proper-fitting footwear is one of the most important ways to manage a crossover toe. Switching to shoes with a wider toe box can ease pressure on the affected toe and reduce discomfort. You should also make sure you have sufficient space at the end of your shoes (typically 1 cm) for your toes to properly splay. If shoes are too short, your toes will curl up. Many companies, like ASICS, APEX and Saucony, offer a wide-width options to give your feet the extra room it needs. Shoes with a mesh or soft upper are also recommended, as this will reduce pressure and friction on the top of the toes.
Orthotics Custom orthotic inserts or pads can help support the arch and redistribute pressure across the foot. This can help promote proper toe alignment and reduce pressure on the crossover toes so that they don't get worse.
Foot and Toe exercises: Performing specific exercises to strengthen the muscles and tendons around the toes can improve flexibility and prevent the condition from progressing.
Splinting or taping: A foot specialist can tape the affected toe to encourage proper alignment and reduce pain. You can also buy a splint or toe spacer to help stabilize and align the toe.
Corn and Callus Treatment: Since crossover toes are extremely prone to corns and calluses, it is very important to see a licensed chiropodist for routine foot care. A chiropodist can safely debride any corns and calluses on your crossover toe, which will reduce pain and irritation.
March 28, 2024
Wondering about top foot moisturizing tips and dry skin remedies? Look no further! Skin-related issues are common at Feet First Clinic, so we know a thing or two about the secrets behind soft feet! Keep reading to master our step-by-step guide on the perfect hydrated skin care routine for your feet.
Foot Moisturizing Tips: A Step-by-Step Guide
Numerous studies support the use of high-quality moisturizing creams on the feet to fight xerosis (the medical term for dry skin).
Dry skin acts as a foundation for common foot problems, like pain and soreness, bleeding, cracked heels, peeling skin, and more, so moisturization not only makes your feet feel smooth to the touch, but it also gives you protection against future troubles. Moisturizing can also help you manage more serious concerns, like diabetes and psoriatic arthritis.
Below are the steps you should follow to guarantee you are lathering your feet up the right way:
Step 1: Get the right products
Step 2: Cleanse and exfoliate your feet
Step 3: Moisturize your feet
Step 4: Protect and maintain
https://youtube.com/shorts/JkHzT9z8fiU?si=g5qXU7pCjCjNixPS
Step 1: Get the Right Products
For the best results, choose medicinal moisturizing creams (for example the brand Gehwol). These focus on hydration, are fragrance-free and made without harsh chemicals. Some factors to look out for:
Creams that contain Urea. This gently exfoliates while also softens the skin.
Glycerin which relieves dryness and retains moisture
Emollient. If the cream states that it is an emollient that means it has to penetrate further into the skin rather than just the top layer
Balms. These are thicker and are specially designed to penetrate the skin more thoroughly. They are useful for people prone to cracked heels.
Step 2: Cleanse and Exfoliate Your Feet
Before moisturizing comes foot hygiene! You should always start with a clean base. Within your bathing routine clean your feet in warm water with fragrance-free, gentle soaps, and thoroughly dry, especially in between the toes (vulnerable area for fungal infections). To go the extra mile, exfoliate your feet with a scrub product and finish off with a foot file on the bottom of the feet. This eliminates dead skin cells, making your moisturizer more effective!
Be careful though. Dry skin can be surrounded by good skin so you don't want to rub your dry skin too much. Separate cleansing of your feet can actually dry your feet out. So a regular bath/ shower is ample.
Step 3: Moisturize Your Feet
Moisturizing itself is pretty simple. Use a generous dollop (but not too much) of moisturizer and focus on dry areas, if you have any. Massage the moisturizer into your feet using circular motions, ensuring full coverage. Avoid the area in between the toes if you’re prone to infections or wounds (if you have diabetes). Moisture can build in the between the toes more easily than other areas.
Step 4: Protect and Maintain
Repeat this process regularly, ideally daily or at least a few times a week, to keep your feet soft, smooth, and well-hydrated. If your skin is especially vulnerable and sensitive, like for those with psoriasis and psoriatic arthritis, a regular routine is extra important to help you manage painful flare- ups.
October 5, 2023
When it comes to toenail anatomy, certain factors can affect structure and growth pattern. Case in point: curly toenails. They don't look quite right and the truth is, there are several potential culprits. Sometimes it can be an underlying health condition presenting symptoms via your nails, and other times it is a direct toenail condition. As a side note, it's also wise to ensure curling toenails don't co-exist with/turn into ingrown toenails, which may become infected.
Let's take a look at what might be causing your curling toenails, and what you can do about it!
Causes of Curly Toenails
Onychauxis
Onychauxis is the general term for abnormal toenail thickening. It is usually caused by trauma. The toenails thicken excessively, eventually causing the nails to curl and turn white or yellow. They can be more prone to fungal infection once the toenail is traumatized. The nail plate may also separate from the nail bed. Diabetes patients in particular should be on the lookout for diabetes-related onychomycosis and onychauxis, or “ram horn,” and other severe abnormalities caused by toenail thickening and curling.
Onychomycosis
This is a fungal toenail infection in the nail unit (the nail plate, surrounding soft tissues and nail folds). It usually results in nail thickening and the formation of pincer nails (curly toenails).
Autoimmune Illnesses and Deficiencies
Lupus, psoriasis, psoriatic arthritis and thyroid disorders can all cause thickened toenails that eventually degrade and curl. Severe iron deficiency can also cause curly toenails since iron is so critical for maintaining our nail and foot health.
Ill-Fitting Footwear
Perhaps the most common cause of curly toenails is also the most avoidable — simply neglecting foot care and failing to buy shoes that fit well. Wearing shoes that are far too tight for years (perhaps because you’re procrastinating a proper shoe fitting) is a mistake. When you wear shoes with minimal space in the toe box, the shoe will squeeze both sides of the toe, disrupting normal nail growth and bending the nail root or matrix.
Medications
Drug-induced nail disease is a very real concern for those taking necessary medicines. Some examples of medications that cause curly toenails and other nail growth disruptions include chemotherapy drugs, lithium, and Retinoids.
Genetics
Sometimes your gene pool is responsible for your curly toenails. Your mom and dad can pass down hereditary characteristics like the shape and thickness of your toenails, as well as how much skin you have surrounding the toenails. But don’t worry if you feel like you have no control over genetic traits - proper foot care can still help you manage curly toenails.
Here are some of the best treatments for curly toenails:
Medical Pedicures: Chiropodists can properly clean and trim the nails to promote healthy growth.
Antifungal Medicines: These can help with onychomycosis.
OnyFix: Modern, non-invasive treatment that involves using a special paste to correct nail growth.
At-home foot care: Remember to keep your feet and nails clean, but don’t try to trim them on your own if they're severely curled or ingrown. If your toenails look like this, it's best to contact a chiropodist.
Diabetic foot care from a Toronto foot clinic.
September 28, 2023
There’s nothing quite as annoying as an itch that just won’t let up. And when it’s a tough-to-reach area like our feet, it’s even worse. But luckily, with the help of your local Toronto chiropodist and a little foot care, itchy feet are achievable! Your first step is understanding what foot condition might be causing your itchy feet and then learning about top treatment methods.
Causes of Itchy Feet
Athlete's foot
Psoriasis and psoriatic arthritis
Contact dermatitis
Atopic dermatitis
Additional causes
Athlete’s Foot
Athlete’s foot is causes itchiness on top of the feet, often on and between the toes. Both adults and kids can contract it by walking on contaminated floors without shoes (locker rooms, public showers, etc) or sharing towels and other items. The excessive itching will eventually produce a scaly rash.
Psoriasis and Psoriatic Arthritis
Both conditions cause dry, itchy patches of skin to form on the feet, with psoriatic arthritis producing additional, painful arthritic symptoms. Medical News Today notes that psoriasis can also lead to pus-filled blisters on the soles of the feet.
Contact Dermatitis
This is an allergic reaction to a product that touches your feet. New fragrant lotions, fabrics or detergents you’ve never tried may be the offender. The itchy rash forms along the area that touched the allergen.
Atopic Dermatitis
Atopic dermatitis is a medical term for eczema. It is a chronic, non-contagious condition that often develops during childhood and lingers into adulthood. In addition to extreme itchiness, it can cause inflamed red skin, swelling, cracking and may produce a clear fluid if you keep scratching.
Additional Causes of Itchy Feet
Keep in mind that itchy feet can have numerous other causes — here are some more you may recognize:
Diseases like liver disease, kidney disease and cancer
Bug bites (check to see if you have bites in other areas too)
Scarring
General dry skin
Diabetes-related neuropathy. Read about the connection between neuropathy and diabetic ulcers.
Chilblains (reaction to cold temperatures)
Treatments for Itchy Feet
General Self Care
Morning and evening foot care routines can soothe the nagging itch from many conditions. This includes moisturizing, exfoliating, and enjoying warm foot baths. Try medicinal products from companies like Gehwol; they use ingredients that promote foot health and steer clear of harmful chemicals and fragrances.
Medical Pedicures
When a chiropodist performs a medical pedicure, you also get the added benefit of a thorough cleaning and moisturizing season that relieves itchy feet and may protect you from future flare-ups. Skipping cosmetic pedicures and opting for medical ones can also help you avoid further contamination from nail salons.
Medications and Anti-Fungal Products
If you have athlete’s foot, it might not respond to self-care and nonprescription products. In this case, you may need to try an anti-fungal ointment, cream or spray recommended by a chiropodist. Serious infections may warrant oral anti-fungal pills.
Furthermore, those with contact dermatitis can try over-the-counter antihistamines like Benadryl, Claritin and Allegra.
March 20, 2023
Are you experiencing foot arch pain? You’re not alone.
The arches of our feet support our weight when we're upright, providing a critical function for the body. Your arch also influences how you move, making it essential to keep them healthy and supported. But, sometimes, pain can creep up.
We're here to help. This blog post outlines how foot arch pain develops and how to nip foot arch discomfort early to prevent long-term effects.
What is foot arch pain?
Foot arch pain can be a subtle or intense discomfort in the curved, raised area along the bottom of the foot (the arch). The arch is the midpoint of the foot between the ball and the heel of the foot. It comprises bones, ligaments, and tendons in the foot, which support the body's weight and help absorb shock during walking and other activities.
A person's arch is unique. The height and shape of the arch vary from person to person. Genetics, age, and the type of shoes a person wears all play a role in the arch's shape. Foot arch pain is a common source of discomfort and may occur for various reasons. You may experience pain in different parts of the arch: the medial arch (inside edge), the lateral arch (outer edge), and the transverse arch (middle).
Next, we get into the causes of foot arch pain.
What causes foot arch pain?
Foot arch pain can be acute or chronic, typically stemming from inflammation. Pain can also range from a dull soreness to an intense sensation. Below, we outline the various causes of foot arch pain.
Overuse or repetitive stress
Foot arch pain can be simply the result of doing too much in too short a period. Repeated stress or overuse of the feet can lead to inflammation and pain in the arches. Overuse is especially prevalent in sports, with running, jumping, or even standing for long periods (like at work or if you stand at your desk while working from home).
Flat feet
Flat feet occur when the arch comes in complete contact with the ground due to weakened tendons and ligaments that can no longer hold up the arch. While flat feet may not always cause problems, individuals with fallen arches may require treatment such as supportive shoes or custom orthotics to alleviate symptoms and prevent further damage.
Plantar fasciitis
Plantar fasciitis affects the bottom of the foot and causes heel pain. This foot condition occurs when the band of tissue between your heel and toes becomes irritated. Plantar fasciitis can happen for various reasons, such as overuse, repetitive strain, or injury to the foot.
People who are overweight, have flat feet or high arches, or engage in activities that stress the feet, such as running or standing for long periods, are more likely to develop plantar fasciitis. You may experience pain and stiffness in the heel or arch of the foot, especially in the morning or after walking, running, or standing.
Arthritis
Arthritis describes conditions that cause inflammation and damage to the joints. Various forms of arthritis can lead to arch pain. Types of arthritis that cause arch pain include osteoarthritis, rheumatoid arthritis, and psoriatic arthritis.
Injury
You may experience foot arch pain because of past trauma or injury. Conditions like sprains, strains, or falls can cause arch pain due to acute muscle damage, ligament, and tendon damage.
Now that you know the various causes of arch pain, let's get into treatment methods.
How can foot arch pain be treated?
Foot arch pain treatment can sometimes be frustrating due to our reliance on our arch. Staying off our feet to reduce stress on the arch can be challenging, but fortunately, there are several effective treatment options for foot arch pain. Depending on the intensity of the pain, you may choose a DIY treatment method. If your arch pain is persistent or severe, we recommend seeing a foot specialist to discuss treatment options and create a treatment plan.
Rest and ice
A mix of rest and ice is an effective treatment method for foot arch pain. First, temporarily reduce impactful activities and allow your feet to rest. Supplement rest with icing to keep swelling and inflammation down. (You can even use a frozen water bottle as an icy massage tool by rolling your feet on the bottle.) Then, when you feel like you're on the upswing, ease slowly back into physical activity. Avoid returning to strenuous activity to allow your body to readjust from rest to being active.
Stretching
Stretching exercises can help improve flexibility and relieve tension in the arches. Here are a few effective stretching and strengthening exercises for arch pain:
Place a towel on the floor, and grab the towel with your toes pulling it towards you.
Grasp your toes (while seated), and scrunch them towards you to feel a stretch in your arch.
Lean against a wall with your arms extended, and move your hips forward to stretch your calves.
Shockwave Therapy
This non-invasive innovative treatment delivers high-energy sound wave pulses to the affected area. Shockwave therapy triggers your body’s natural healing response to repair the damaged tissue in the arch area and reduce pain. Shockwave therapy is scientifically proven to be a highly effective treatment for chronic arch pain caused by plantar fasciitis. It is an excellent supplement to other treatments like orthotics and supportive footwear.
Orthotics
Custom-made orthotics can provide additional support and cushioning to the arches, which can help reduce pain and discomfort. Orthotics work to correct or accommodate biomechanical abnormalities, foot deformities, and other conditions to improve your gait and manage pain. The purpose of orthotics is to redistribute the force and pressure placed on our muscles and joints when we move. Equal distribution across your feet means fewer aches and pains as your muscles work better in tandem instead of select groups overworking.
Supportive footwear
Shoes with good arch support can alleviate arch pain, much like orthotics can. Wearing the proper footwear for your feet and the purpose is the least we can do for our feet. Supportive footwear acts to provide both the correct cushioning and
Physical therapy
Physical therapy can help improve strength, flexibility, and range of motion in the feet and ankles. Keeping your feet strong and balanced is vital to proper arch support. Over time, the tendons and ligaments of the arch tend to weaken. Physical therapy can help combat age and fallen arches.
Medications
You may supplement the above treatment methods with over-the-counter medication like ibuprofen or acetaminophen to reduce inflammation. Consult a doctor if you have intense pain or have questions about dosage or the recommended medication.
January 23, 2023
Have you ever noticed horizontal lines or grooves lengthwise across your nails? The nail abnormality is called Beau's lines. You may develop Beau's lines after trauma to the nail, or it may be a sign of an underlying medical condition.
Today's blog article explores Beau's lines, potential causes, and treatment methods. Keep read to learn more about Beau's lines and how to keep your nails healthy and strong.
What are Beau's lines?
Beau's lines are a type of nail abnormality. They are indentations, grooves, or lines that run horizontally across the nails. The condition can affect any number of fingernails or toenails. Amongst your toenails, the big toe is the most common culprit. Curious as to why they're referred to as Beau's lines? French physician Joseph Honoré Simon Beau first discovered the condition, hence the name.
What causes Beau's lines on nails?
A temporary disruption in the growth of the nail matrix causes Beau's lines. They are symptoms of an underlying illness, medical, or skin condition. They appear when average nail growth is interrupted, and the blemishes appear due to irregular keratin (skin cells) development. Once you can identify and treat the underlying cause, normal nail growth may resume.
Identifying Beau's lines can be delayed because of the nail growth rate. Toenails grow at ~1.60 mm per month, so nail growth delays Beau's lines' arrival. The lines appear roughly 2-3 weeks after damage or cause sets in.
The number and distinctiveness of Beau's lines can provide insights and clues into possible causes. For instance:
One Beau's line on a single toenail may indicate a less severe injury.
Beau's lines on multiple nails may indicate higher stress levels or a more severe injury/illness.
Several rows of Beau's lines on each toenail with a gap in between may indicate multiple traumas over time, but not at once.
Fewer but thicker Beau's lines may signify a chronic injury or illness.
Beau's lines may occur for several reasons. Possible causes include:
Illness or severe stress. Being ill or stressed can divert your body's resources and nutrients away from nail growth. Blood flow interference due to an illness or infection is the culprit. Certain illnesses or infections can cause Beau's lines, including:
Viral infections
Heart attack
High fever
Measles
Mumps
Pneumonia
Strep infections
Raynaud's disease
COVID-19. A study published in the National Library of Medicine noted that COVID-19 might cause Beau's lines. The coronavirus is by no means the sole cause of Beau's lines but can be a trigger. As such, Beau's lines are sometimes known as "COVID nails."
Nail trauma. Acute or chronic trauma to your toenails can interrupt nail growth and cause Beau's lines. For example, you may stub your toe, drop an item on your foot, or wear ill-fitting shoes that add undue pressure to your toes and toenails. Damage to the nail matrix—the part of the nail where growth starts—is notably correlated with Beau's lines as growth is interrupted at the root.
Skin conditions. Skin conditions, including eczema and psoriasis, can damage your nail matrix.
Vitamin or nutrient deficiencies. Particular vitamin and nutrient deficiencies can interrupt nail growth. For instance, biotin deficiency is known to cause brittle nails and affect nail growth. Zinc deficiency is also linked to the nail condition.
Chemotherapy side effects. Approximately 23% of anti-cancer therapy patients report nail changes. Changes to the nail may include Beau's lines.
Paronychia. Inflammation of the skin around the nails (known as paronychia) can cause Beau's lines.
How do I treat Beau's lines?
Moisturizing dry, itchy skin, both the byproducts of skin conditions, can help reduce the damage to the nail fold.
There is no one-size-fits-all treatment for Beau's lines, nor is there a specific treatment for the condition per se. The key is to address the underlying cause - whether it be a medical condition or acute trauma - rather than the symptom (i.e.: what you see on your nails).
Below are several possible treatment methods you can try, depending on the underlying condition:
Allow the nail to grow out. Nail growth is approximately 1 mm every 6-10 days. Letting the nail grow and slowly trimming the tips reduce the appearance of lines on the toenail. The entire toenail should grow out within 6-8 months.
Apply creams or moisturizers for eczema or psoriasis. Moisturizing dry, itchy skin, both the byproducts of skin conditions, can help reduce the damage to the nail fold.
Avoid salon manicures, artificial nails or harsh nail products. Avoiding harsh chemicals and products can help reduce the trauma of the nail matrix.
Mask the ridges with nail polish. Nail polish is a cosmetic treatment to hide the grooves from Beau's lines. However, some nail polishes can weaken the nail, so be cautious about your product.
Get a medical pedicure from a licensed chiropodist to encourage proper nail growth, perform a thorough examination, and eliminate onychophosis (the buildup of skin cells in the nail folds, nail plate and cuticles).
Take biotin supplements. Some studies suggest that taking biotin can increase nail plate thickness by 25%. Generally, adults 19+ should be consuming 30-35 mg of biotin per day.
Biotin and Zinc supplements are believed to help nail growth.
If you find Beau's lines persisting, or worsening, it's recommended to contact a healthcare professional for a proper diagnosis and treatment plan.