April 16, 2026
Toe spacers are everywhere right now—from physiotherapy clinics to fitness influencers promoting “natural foot alignment.” But do toe spacers actually work, or are they just another trend?
The short answer: yes, but with the right expectations. Let’s break down what toe spacers do, who they help, and how to use them effectively.
What Are Toe Spacers?
https://youtu.be/mK4pz6Pmjzo?si=1CWQoSiUZu7xhEpN
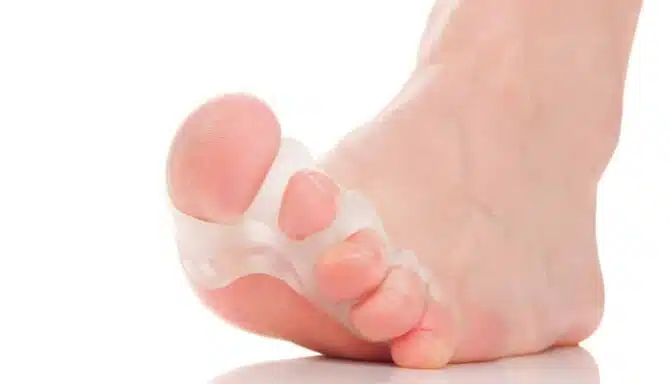
Toe spacers (also called toe separators or toe aligners) are small devices placed between your toes to gently spread them apart. Most are made from silicone or gel and come in various sizes and designs, from simple separators to full forefoot alignment tools.
They’re designed to reverse the effects of:
Tight, narrow footwear
Prolonged standing or walking
Muscle imbalances in the feet
Progressive toe deformities
Over time, these factors can cause your toes to crowd, overlap, or shift out of their natural position.
Do Toe Spacers Actually Work?
Yes—but with realistic expectations.
Toe spacers work by gradually encouraging your toes back toward their natural alignment. This can reduce pressure, improve muscle activation, and enhance overall foot function.
Benefits of Toe Spacers
When used consistently, toe spacers can:
Relieve pressure and painSeparating the toes reduces friction and pressure points, especially between overlapping toes.
Improve toe alignment (to a degree)They can help slow progression and mildly correct early deformities.
Support bunion managementBy spacing the big toe away from the second toe, they reduce stress on the joint.
Enhance foot muscle engagementToe spacers allow intrinsic foot muscles to activate more naturally during movement.
Improve balance and stabilityA wider toe splay increases your base of support.
What Toe Spacers Cannot Do
This is where expectations matter most.
Toe spacers cannot:
Permanently reverse advanced bunions or rigid hammertoes
Replace custom orthotics when biomechanical issues are present
Deliver instant or dramatic structural changes
Think of them as a supportive tool, not a cure.
Conditions That Benefit Most from Toe Spacers
Toe spacers are most effective in early or mild cases of:
Bunions (hallux valgus)
Hammertoes and claw toes
Overlapping or crowded toes
Forefoot pain (metatarsalgia)
Corns and calluses caused by friction
They’re also popular among runners and gym-goers looking to improve foot strength and alignment.
How to Use Toe Spacers for Best Results
Using toe spacers properly makes a big difference in outcomes.
1. Start Gradually
Begin with 10–15 minutes per day, especially if your toes are stiff or sensitive. Increase wear time slowly as your feet adapt.
2. Wear Them in the Right Setting
Barefoot at home
With wide, foot-shaped shoes
Avoid tight footwear, which cancels out the benefit
3. Be Consistent
Like stretching, results come with daily, long-term use—not occasional wear.
4. Combine with Foot Exercises
Toe spacers work best alongside strengthening and mobility work, such as:
Toe splaying exercises
Towel scrunches
Calf and plantar fascia stretches
5. Listen to Your Body
Mild discomfort is normal at first, but pain is not. If something feels off, reduce wear time or reassess fit.
Are Toe Spacers Safe?
For most people, yes. However, there are a few precautions.
Use caution if you have:
Diabetes
Poor circulation
Nerve damage (neuropathy)
Open wounds or skin irritation
In these cases, it’s best to consult a foot specialist before use.
How Long Does It Take to See Results?
Results vary depending on the individual and condition severity.
Short-term (days to weeks): Pain relief and reduced pressure
Medium-term (weeks to months): Improved flexibility and toe mobility
Long-term (months+): Subtle alignment improvements and better foot function
Consistency is everything—think of it as retraining your feet over time.
Are Toe Spacers Worth It?
If you’re dealing with mild toe misalignment or foot discomfort, toe spacers are a low-risk, affordable, and effective tool.
However, if your condition is more advanced or painful, they should be part of a broader treatment plan that may include:
Custom orthotics
Footwear changes
Professional foot care
In some cases, minor procedures
The Bottom Line
Toe spacers do work—but they work best as part of a consistent foot care routine. They can relieve pain, improve toe positioning, and support healthier foot mechanics over time.
The key is using them properly, staying consistent, and understanding their limitations.
April 2, 2026
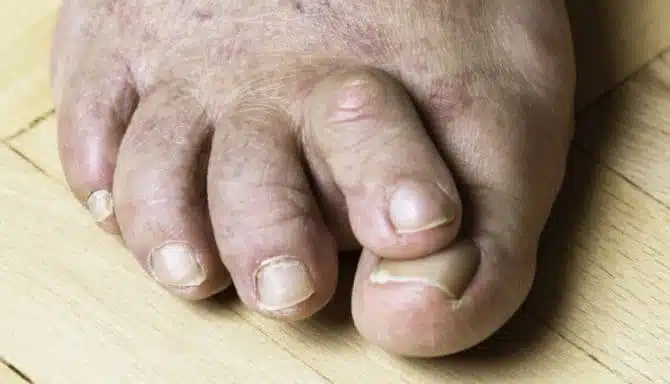
Toe deformities like hammertoes and clawed toes are more than just cosmetic concerns—they can significantly impact your comfort, mobility, and quality of life. Whether it’s difficulty finding shoes that fit, pain while walking, or the development of corns and calluses, these conditions can become increasingly problematic over time. Fortunately, modern foot care offers effective solutions. One such solution is the flexor tenotomy, a procedure designed to correct toe deformities and restore normal function with minimal downtime.
Understanding Hammertoes and Clawed Toes
Hammertoes and clawed toes are common deformities of the toes caused by imbalances in the muscles, tendons, or ligaments that normally keep the toes straight.
Hammertoe: The middle joint of the toe bends downward, creating a hammer-like appearance. It often affects the second, third, or fourth toes.
Clawed Toe: The toe bends at both the middle and end joints, giving it a claw-like appearance. This deformity can be more rigid and uncomfortable.
These conditions can lead to pain, corns, calluses, difficulty walking, and challenges finding comfortable footwear. Risk factors include wearing tight shoes, high heels, muscle imbalance, arthritis, and genetics.
Conservative Treatments
Before surgery, mild hammertoes and clawed toes can sometimes be managed with:
Footwear modifications: Wide-toe box shoes and avoiding high heels.
Toe splints or orthotics: Help realign the toes and reduce pressure.
Exercises: Stretching and strengthening exercises for toe muscles.
However, if the toe becomes rigid or painful, surgical options like flexor tenotomies may be the most effective solution.
What is a Flexor Tenotomy?
A flexor tenotomy is a minimally invasive surgical procedure that releases the flexor tendon causing the toe to bend. It is usually performed under local anesthesia and involves only a tiny incision, allowing the toe to straighten naturally.
This procedure can correct flexible and semi-rigid hammertoes and clawed toes (meaning that the toe can be manually straightened) without the need for more invasive surgery. It is not suitable for hammertoes or clawed toes that cannot be manually straightened (rigid hammertoes).
Benefits of Flexor Tenotomies
Minimally invasive: It involves a tiny incision with low risk of complications.
Fast recovery: Most patients walk immediately and resume daily activities quickly.
Pain relief: Reduces pressure on joints, corns, and calluses.
Prevention of future complications: Especially important for diabetic patients at risk for foot ulcers.
Who is a Candidate?
Flexor tenotomies are best suited for patients with:
Flexible or semi-rigid hammertoes and clawed toes
Pain, discomfort, or skin irritation caused by toe deformities
No severe arthritis or joint damage in the affected toes
A chiropodist or foot specialist can evaluate the severity of the deformity and recommend the most appropriate treatment.
The Procedure
During the procedure:
A tiny incision is made at the base of the affected toe.
The flexor tendon is carefully released.
The toe is gently straightened and bandaged.
Post-procedure, most patients are allowed to walk immediately, sometimes using protective padding or special footwear.
Recovery and Aftercare
While a flexor tenotomy will help loosen the affected tendon and straighten the toe, it will not correct the underlying cause of the deformity. Flexor tenotomies are thus best used in conjunction with custom orthotics to correct any biomechanical issues, as well as proper fitting, supportive shoes.
Conclusion
If you have hammertoes or clawed toes, a flexor tenotomy offers a safe, minimally invasive solution that can relieve pain, restore toe alignment, and improve your ability to walk comfortably. Early intervention can prevent corns, calluses, and other complications, especially in patients with diabetes or mobility issues.
March 5, 2026
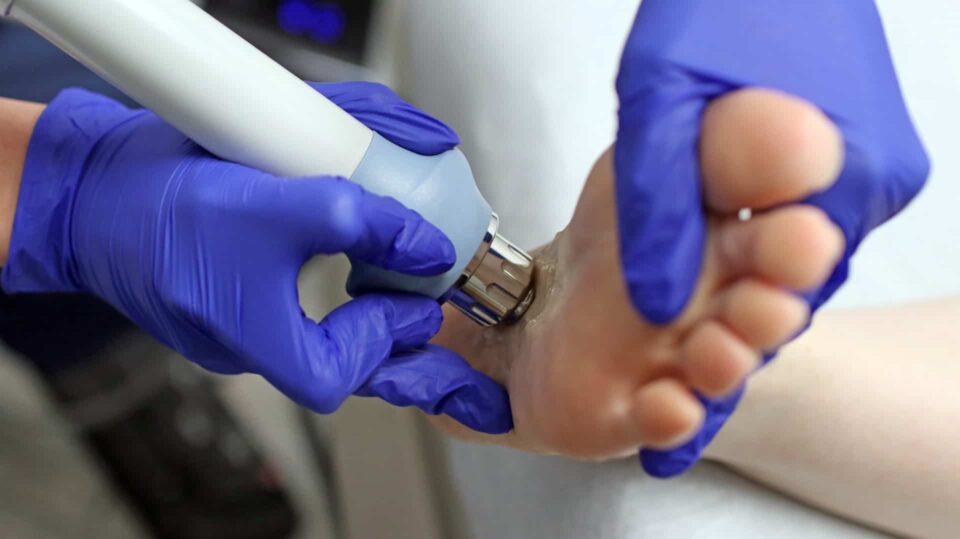
What Are Ultrasound-Guided Steroid Injections?
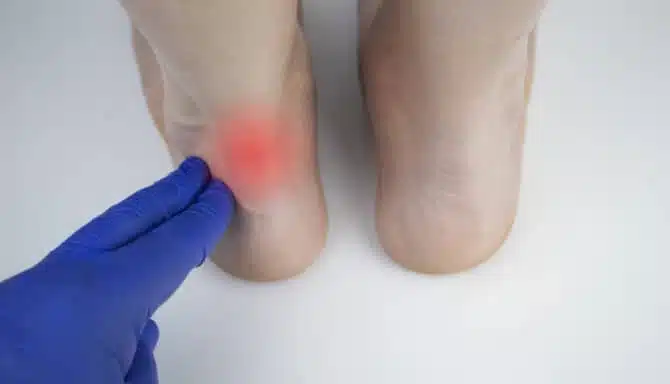
Ultrasound-guided cortisone injections are a precise, minimally invasive way to treat chronic foot and ankle pain. They combine corticosteroid medication—commonly called cortisone—with ultrasound imaging to target the exact area of inflammation.
Unlike “blind” injections, which rely on anatomical landmarks and the clinician’s feel, ultrasound guidance allows a podiatrist or chiropodist to see the tissues in real time. This ensures the cortisone reaches the injured tendon, ligament, joint, or nerve exactly where it’s needed.
This combination of precision and anti-inflammatory medication makes the treatment highly effective for conditions like:
Plantar fasciitis
Achilles tendonitis
Ankle arthritis
Neuromas (i.e.: Morton's Neuroma) or nerve irritation
How Cortisone Works
Cortisone is a synthetic steroid that mimics hormones naturally produced by your adrenal glands. Its main job in foot and ankle injections is to reduce inflammation.
Here’s what happens on a cellular level:
Cortisone suppresses inflammatory chemicals called cytokines that cause swelling and pain.
It stabilizes cell membranes in the injured tissue, preventing further irritation.
Cortisone can also reduce nerve sensitivity in the area, which helps decrease pain perception.
By directly targeting the source of inflammation, cortisone helps speed up healing and relieve chronic pain without the need for surgery.
The Role of Ultrasound in the Injection
Ultrasound guidance takes steroid injections to the next level. Using high-frequency sound waves, the clinician can see:
Tendons and ligaments
Inflamed soft tissue
Nerves
Joint spaces
This allows the injection to be delivered exactly where it’s needed, which:
Improves the effectiveness of the medication
Minimizes risk of hitting nerves, blood vessels, or healthy tissue
Reduces discomfort during the procedure
For example:
In plantar fasciitis, the cortisone is placed at the point where the plantar fascia attaches to the heel bone.
In Achilles tendonitis, the cortisone is delivered around the tendon sheath rather than the tendon itself, preventing damage to healthy tissue.
In neuromas, it targets the inflamed nerve sheath precisely, reducing pain without affecting surrounding nerves.
Why It Works: The Science
The combination of corticosteroids and its precise placement is what makes this treatment so effective.
Targeted anti-inflammatory action – By delivering cortisone directly to the inflamed tissue, the body’s natural healing process can work more efficiently.
Reduced tissue trauma – Ultrasound guidance avoids unnecessary needle trauma to surrounding tissue, allowing faster recovery.
Pain modulation – Cortisone temporarily decreases nerve irritation, which lowers pain signals sent to the brain.
Support for chronic injuries – Chronic tendon or ligament injuries often involve persistent inflammation and microtears. Cortisone helps calm inflammation so the tissue can repair itself.
In short, the science is all about precision + anti-inflammatory power: delivering cortisone exactly where it’s needed to calm inflammation, reduce pain, and support healing.
Who Can Benefit from Ultrasound-Guided Cortisone Injections?
This treatment is ideal for people with chronic foot or ankle pain that hasn’t improved with other treatments like:
Rest and activity modification
Custom orthotics or supportive shoes
Physical therapy
Anti-inflammatory medications
It’s especially helpful for plantar fasciitis, Achilles tendonitis, ankle arthritis, or nerve-related foot pain.
Ultrasound guided injections alone won't address any underlying biomechanical issues that caused the pain in the first place. Therefore, it's most effective when combined with other treatments, like custom orthotics, supportive shoes that match your foot type and gait pattern, and physiotherapy.
Bottom Line
Ultrasound-guided steroid injections are a safe, precise, and scientifically backed way to treat chronic foot and ankle pain. By combining the anti-inflammatory power of cortisone with the accuracy of real-time imaging, patients often experience faster relief and better outcomes than with traditional injections.
Feature image by nts01 from Pixabay
November 27, 2025
Your feet are essential to your mobility and independence, yet they’re commonly overlooked in everyday health routines. Proper foot care is about more than aesthetics; it helps prevent discomfort, reduce the risk of injury, and support your overall well-being.
At Feet First Clinic in Toronto, our chiropodists treat everything from nail and skin concerns to pain and mobility issues. Here are the top five ways to take care of your feet to keep them healthy and strong all year round.
1. Keep Your Feet Clean and Dry
Healthy feet start with good hygiene. Wash your feet daily with warm water and mild soap, and don’t forget to clean between the toes. After washing, dry your feet thoroughly (especially between the toes) to help prevent fungal infections like athlete’s foot.
If your feet tend to sweat a lot, moisture-wicking socks or antibacterial foot deodorant powder can help keep them dry and fresh.
2. Moisturize to Prevent Cracked Heels and Dry Skin
Dry, flaky, or cracked skin on the feet can be uncomfortable and, if left untreated, may lead to infection. Applying a foot cream or urea-based moisturizer daily helps lock in moisture and keeps the skin soft and supple.
Focus on the heels and soles, but avoid putting lotion between the toes as excess moisture there can increase the risk of fungal infections.
If you have thick, rough skin or painful calluses, a chiropodist at Feet First Clinic can safely debride (shave down) the skin and recommend medical-grade moisturizers to help prevent recurrence.
3. Trim Your Toenails Properly
Toenail care is more important than it might seem. Cutting nails too short or rounding the corners can cause ingrown toenails, which are painful and can become infected. Trim your nails straight across and gently file any sharp edges.
If your nails are thick, discoloured, or difficult to trim, don’t force it. Our chiropodists have specialized tools to safely and comfortably trim thick toenails, and we can check for signs of fungal infections or other nail concerns.
Feet First Tip: The best time to trim your toenails is after a shower when they’re softer and easier to cut.
4. Choose Proper Footwear
Your shoes play a huge role in your foot health. Wearing shoes that are too tight, narrow, or unsupportive can lead to corns, calluses, bunions, or heel pain.
When buying new shoes, make sure:
There’s about a finger’s width of space between your longest toe and the front of the shoe.
The heel fits snugly without rubbing or pressure.
You can wiggle your toes freely.
If you have foot pain, flat feet, or high arches, custom orthotics may be a game-changer. At Feet First Clinic, our chiropodists assess your gait and foot structure to design orthotics that support your body from the ground up.
5. Schedule Regular Foot Checkups
Even if your feet feel fine, regular checkups can help prevent problems before they start. Chiropodists are trained to detect and treat a wide range of foot and nail conditions, including:
Ingrown and fungal toenails
Corns, calluses, and cracked heels
Plantar fasciitis and heel pain
Diabetic foot complications
At Feet First Clinic, we believe prevention is the best medicine. Routine foot care helps maintain comfort, mobility, and confidence — especially as we age or if we spend long hours on our feet.
Feet First Tip: If you notice pain, swelling, or changes in your toenails or skin that don’t go away, it’s time to book an appointment. Small issues can quickly become big problems if ignored.
October 30, 2025
Extensor tendonitis is a common foot condition that affects the tendons running along the top of your foot. These tendons connect your muscles to your toes and help lift your toes and foot during walking and other activities. When these tendons become inflamed or irritated, it can lead to pain and difficulty moving your foot comfortably.
What Is Extensor Tendonitis?
Extensor tendonitis refers to inflammation or irritation of the extensor tendons on the top of the foot. This condition often results from overuse, repetitive strain, or injury. People who are active in sports, wear tight footwear, or have certain foot structures may be more prone to developing extensor tendonitis.
Causes of Extensor Tendonitis
Overuse: Repetitive activities such as running, jumping, or walking long distances.
Improper Footwear: Shoes that are too tight or have insufficient space on the top can compress the tendons.
Foot Mechanics: Flat feet, high arches, or gait abnormalities can put extra strain on the tendons.
Injury: Trauma or sudden impact to the foot.
Underlying Conditions: Arthritis or inflammatory diseases may contribute to tendon irritation.
Symptoms of Extensor Tendonitis
Pain and tenderness on the top of the foot, especially over the affected tendon.
Swelling or redness along the top of the foot.
Difficulty lifting the toes or foot.
Pain worsens with activity and improves with rest.
Occasionally, a burning or tingling sensation.
Treatment Options
Rest and Activity Modification
Avoid activities that aggravate the pain and allow the tendon to heal.
Proper Footwear
Wear shoes with adequate space in the toe box and good support to reduce pressure on the top of the foot.
Ice Therapy
Apply ice packs to reduce inflammation and pain.
Physical Therapy
Stretching and strengthening exercises can improve tendon flexibility and foot mechanics.
Orthotics
Custom orthotics may help correct biomechanical issues that are causing excess strain on the extensor tendon and muscles on top of the foot.
Medication
Non-steroidal anti-inflammatory drugs (NSAIDs) can reduce pain and inflammation.
When to See a Specialist
If pain persists beyond a few weeks or worsens, consult a chiropodist or foot specialist for a biomechanical assessment and personalized treatment plan.
October 2, 2025
The Achilles tendon is the strongest tendon in the body. It connects your calf muscles to your heel bone and enables activities like walking, running, and jumping. However, it is also prone to injury -particularly from overuse. Two common conditions affecting the Achilles tendon are Achilles tendonitis and Achilles tendinosis. Although their names sound similar, they differ in causes, symptoms, and treatment approaches. Understanding these differences is crucial for effective recovery and prevention.
What Is Achilles Tendonitis?
Achilles tendonitis is an acute inflammation of the Achilles tendon, typically caused by sudden increased activity or repetitive strain. It results in swelling, pain, and irritation along the tendon.
Typical pain in a male jogger`s achilles tendon. XXL size image.
Causes of Achilles Tendonitis:
Sudden increase in physical activity or intensity
Overuse during running or jumping sports
Poor footwear
Training on hard surfaces
Tight calf muscles
Poor biomechanics
Symptoms of Achilles Tendonitis:
Sharp or burning pain along the back of the heel or lower calf
Swelling and tenderness over the tendon
Stiffness, especially in the morning or after rest
Pain worsens with activity
What Is Achilles Tendinosis?
Achilles tendinosis is a chronic condition characterized by degeneration of the tendon’s collagen fibers without significant inflammation. It often develops after untreated or recurrent Achilles tendonitis and results in thickening and weakening of the tendon. It's essentially what can happen if Achilles tendonitis goes untreated.
Causes of Achilles Tendinosis:
Repeated micro-tears and poor healing
Chronic overuse without adequate rest
Aging and reduced blood supply to the tendon
Biomechanical abnormalities
Symptoms of Achilles Tendinosis:
Dull, persistent pain along the tendon
Thickened or nodular tendon
Decreased strength and flexibility in the calf and ankle
Pain may improve with warm-up but worsen with prolonged activity
Key Differences Between Tendonitis and Tendinosis
FeatureAchilles TendonitisAchilles TendInosisNatureInflammatoryDegenerative (non-inflammatory)DurationAcute or subacuteChronic, long-termTissue ConditionInflamed tendon fibersDegenerated, disorganized fibersPainSharp, localizedDull, diffuseTreatment FocusReduce inflammation, restPromote tendon healing, strengthen
Treatment Options
For Achilles Tendonitis:
Rest and activity modification
Ice and anti-inflammatory medications
Physical therapy focusing on stretching and strengthening
Proper footwear and orthotics
Gradual return to activity
For Achilles Tendinosis:
Eccentric strengthening exercises to stimulate tendon repair
Physical therapy and stretching
Shockwave therapy or ultrasound treatments
Possible use of platelet-rich plasma (PRP) injections
Surgery in severe, unresponsive cases
Prevention Tips
Warm up properly before exercise
Gradually increase activity intensity and duration
Wear supportive, well-fitting shoes
Maintain calf flexibility and strength
Avoid running on hard or uneven surfaces when possible