Age is just a number, but age starts to catch up with us at a certain point. As much as we want aging to slow, getting older comes with its fair share of aches and pains.
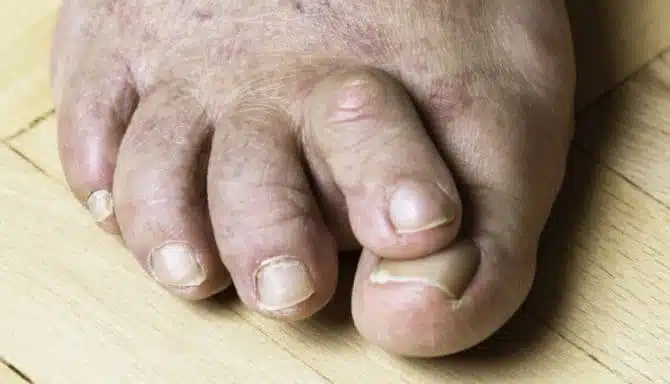
Few people age the same; it is a complex process. Environment, genetics, exercise, and many other factors mould who we become as we enter our elderly years. This also applies our feet. As we age, our feet become more susceptible to various conditions such as arthritis, plantar fasciitis, bunions, foot injuries and chronic pain.
Our latest blog is all about common foot conditions in the elderly and how to treat them.
What happens to our feet as we age?
Did you know that when you turn 70, you’ll be 25,550 days old? That helps put the body’s remarkable ability to withstand constant wear and tear into perspective.
Beyond just a number, there are also physiological changes that occur as we age. Your feet may get bigger. Your feet may widen. Muscles, tendons, and ligaments also wear down, putting you at greater risk of certain foot conditions.
You may notice you experience foot pain and other problems more often. Any number of the following may happen:
- Weakness
- Frailty
- Exhaustion
- Gait alteration
- Balance difficulties
- Increased swaying while walking
- Decreased walking
- Walking speed
As we age, it’s essential to check how you feel regularly. A bonus would be to have your feet checked regularly. Our team of expert foot specialists can help you manage acute and chronic conditions that affect the toes, feet, and ankles.
Most common foot conditions in the elderly
Foot conditions amongst the elderly may include bone injuries, toenail damage, foot deformities, and muscle and tendon damage. It’s important to note that most of these conditions are not specific to the elderly, but age contributes to increased risk.
Below we break down the following common foot conditions in the elderly and how to treat them:
- Bunions
- Osteoarthritis
- Fat Pad Atrophy
- Thickened or Discoloured Toenails
- Gout
- Plantar Fasciitis
- Stress Fractures
1. Bunions
What are bunions?
A bunion is a deformity of the first metatarsophalangeal joint (“MTP” joint for short). The first MTP is the joint of the big toe. (Essentially, the big toe’s “knuckle.) Damage to this joint can cause bone misalignment over time. Eventually, the bone shifts and protrudes at the base of the big toe. Bunions affect approximately one quarter to one third of adults, and women experience the foot condition more often than men.
As we age, bunions worsen. Although there is no “cure” for a progressive foot deformity, you can lessen the effects and pain associated with bunions through several habitual changes.
How can I treat bunions?
You can choose either invasive treatment or non-invasive bunion treatment. In most cases, you can manage bunions with non-invasive treatments, though surgery is the only way to remove the bump altogether.
- Footwear modification: Avoid tight shoes that squeeze the toes and ditch your high heels. You may also find that orthopedic shoes that stretch or come in wide widths effectively accommodate your bunion in your footwear. Shoe stretching is also an effective method for changing the structure of your current footwear.
- Anti-inflammatories: Specific medication like NSAIDs or ibuprofen reduces joint inflammation and relieves pain.
- Splints/aligners: Medical-grade bunion splints and bunion aligners help stabilize the joint. You can choose from medical-grade plastics or a toe sleeve based on your preferred rigidity.
- Taping: A specialist tapes the joint to keep the big toe in place, prevent further misalignment, and manage pain and inflammation.
- Supportive insoles or custom orthotics: Supporting your arches and correcting poor biomechanics can reduce pressure and strain on the first MTP joint.
- Bunion exercises: Basic exercises to strengthen foot muscles can better support and stabilize the joint, thus decreasing pain over time.
The treatments you see above are all available at Feet First Clinic.
2. Osteoarthritis
What is osteoarthritis?
Osteoarthritis is not only the most common variant of arthritis; it is also one of the most common foot conditions in the elderly. Osteoarthritis is the “wear-and-tear” arthritis that causes degeneration of the cartilage in our joints. Reduced cartilage in our joints causes pain and can lead to other foot conditions like bone spurs. Your toes are most susceptible to osteoarthritis.
Age plays a significant role in developing osteoarthritis. Wear and tear of our joints accumulate over time. Also, post-menopausal women risk developing osteoarthritis through osteoporosis (low bone density).
How can I treat osteoarthritis?
Osteoarthritis is a degenerative condition, meaning what’s done cannot reverse. The cartilage in your joints doesn’t re-grow, so treatment aims to slow the effects of osteoarthritis and reduce pain. Effective treatment includes a combination of the following:
- Active rehabilitation: Physiotherapy, massage, and exercise all help reduce the effects of osteoarthritis by promoting solid muscles. Stronger and more balanced muscles and feet reduce the strain on affected areas where you may have osteoarthritis.
- Medication: Anti-inflammatories can help control inflammation.
- Proper footwear: Specialized shoes can accommodate deformities of osteoarthritis (like bunions or hallux rigidus). The right shoes or boots can support your feet, provide balance, and offer cushion.
- Custom orthotics: Orthotics can be customized to add or reduce your reliance on certain parts of your feet. Controlling the impact on affected joints can help prevent further joint damage by distributing the impact and weight elsewhere.
- Limit awkward movements: If you find your joints are sore after a particular activity, consider reducing, modifying, or stopping the activity. For instance, if lunges hurt your foot, consider finding a replacement exercise.
- Surgery: If the joint is damaged extensively, a doctor may recommend surgery. Surgery and removing part of a bony outgrowth can be effective if the sheer volume of bone buildup is the culprit.
If you experience osteoarthritis and are looking for orthotics, a gait analysis, or proper footwear, visit Feet First Clinic for solutions.
3. Fat pad atrophy
What is fat pad atrophy?
The heel fat pad is a cushion to absorb shock and distribute plantar force on impact. As we age, the heel fat pad gets atrophies and gets thinner. This can put you at a greater risk of heel injuries and other foot conditions. The increased pressure on the heel can cause you to overcompensate with other parts of your body, and weight distribution becomes unevenly distributed.
How can I treat fat pad atrophy?
You should reduce the pressure on your heel if you suffer from fat pad atrophy. Custom orthotics are effective as the personalized insoles provide padding and support and help distribute weight across the complex network of foot muscles. Be sure to also wear shoes with lots of padding and cushioning, like the ASICS Gel-Nimbus.
4. Thickened or Discoloured Toenails
What are thick or discoloured toenails?
Thick toenails and discoloured toenails are a byproduct of aging and are one of the most common foot conditions in the elderly.
As we get older, toenail growth declines. As such, nail cells begin to accumulate at a faster rate than nail growth. The accumulation of onychocytes (nail cells) causes thickened toenails. Alternatively, reduced circulation or acute trauma can cause thickened toenails.
Discoloured toenails, on the other hand, indicate damage to the nail or nail bed. Acute trauma to the nail causes discolouration, but so does reduced circulation. At an older age, we’re at a greater risk of diabetes and peripheral vascular disease. Both diabetes and peripheral vascular disease cause reduced circulation in our feet and discoloured toenails.
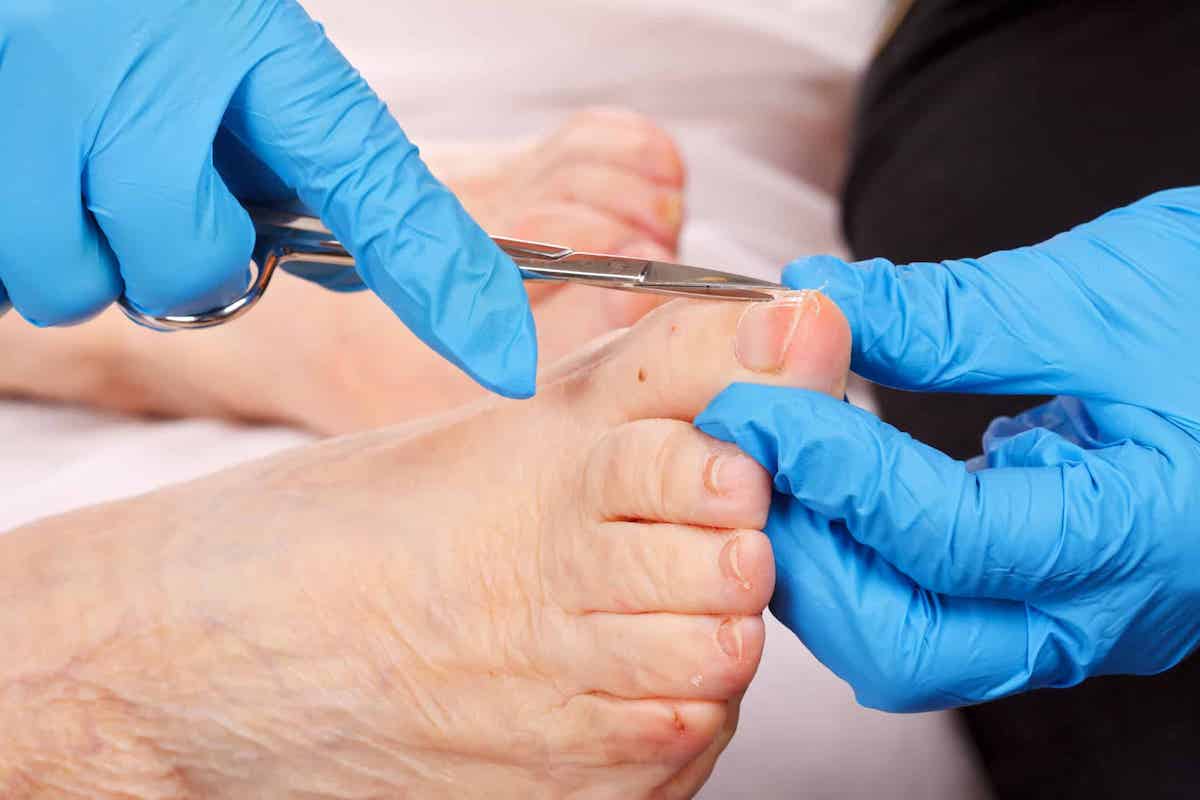
How can I treat thick or discoloured toenails?
Toenail treatment for thickening and discolouration varies. To properly diagnose your feet and nails, book an appointment with a specialist at Feet First Clinic. Our nail care services involve proper trimming and filing of the toenails, addressing any pain or discomfort, and educating patients on proper hygiene and care.
For more information, visit our nail care and treatment page.
5. Gout
What is gout?
Gout is a form of inflammatory arthritis targeting the foot’s joints. You may experience intermittent bouts of severe pain, including inflammation and hypersensitivity. During these episodes, any kind of activity becomes challenging, leaving you less mobile.
The prevalence of gout increases in older people. Elderly people are susceptible to gout for a few reasons: Renal function declines with age, there can be dietary changes, you may experience sudden weight gain, and certain medications for age-related conditions have indirect side effects that may lead to gout (i.e.: water pills, blood pressure medication).
How can I treat gout?
Before any treatment, the first step is to see a family doctor and a rheumatologist. Once diagnosed, you may be prescribed the following treatments, all of which aim to prevent future attacks, reduce pain, and improve quality of life:
- Change your diet: Ditch food containing excessive purines. Avoid foods like red meat, certain types of seafood like sardines and mussels, alcohol, high fructose beverages, and yeast. Diet also impacts your weight. Maintaining a healthy and consistent diet can help reduce sudden weight gain and keep inflammation at bay.
- NSAIDs: Non-steroidal anti-inflammatory drugs reduce joint inflammation. Alternatively, corticosteroids are an option if one doesn’t react to NSAIDs.
- Stay or become active: Light-strengthening exercises, relaxing physical activity, and physiotherapy can improve quality of life and mobility in people with gout. Keeping your muscles strong also makes them less susceptible to inflammation build-up, which can trigger gout attacks.
- Supportive footwear: Proper footwear can help you deal with any pain associated with gout as it reduces the impact on the joints.
6. Plantar fasciitis
What is plantar fasciitis?
Plantar fasciitis is a condition of the heel. The band of tissue on the underside of the foot gets inflamed and causes pain. Often, plantar fasciitis develops gradually over time. Changes in our body as we age can make this condition more common in the elderly.
How can I treat plantar fasciitis?
With proper care and treatment, most cases of plantar fasciitis heal with time. A foot specialist can guide you through the healing process and provide options for preventing it from recurring in the future.
There are several treatment methods available for plantar fasciitis.
- Rest: Take a break, and let your heel recover by staying off your feet.
- Supportive footwear: Wearing supportive footwear with strong arch support and a good heel counter is essential for managing and even preventing plantar fasciitis. Stability shoes are particularly helpful. Check out this article for our top recommended shoes for plantar fasciitis.
- Rolling: Gently massage your heel using a tennis ball or frozen water bottle under the foot. Rolling helps massage and relieve the plantar fascia and encourages faster recovery.
- Add stretching and strengthening exercises to your routine.
- Shockwave therapy: Shockwave therapy delivers sound wave pulses to the injured fascia. This triggers your body’s the healing process, making for a natural recovery. Shockwave therapy is extremely effective for cases of plantar fasciitis persisting more than 6 months.
- Taping: Taping the heel engages other muscles and tendons of the foot, reducing the load on the plantar fascia.
- Wear a splint: A splint helps keep your foot stable while you sleep.
- Supportive Insoles or Custom Orthotics: A good supportive insole, like Superfeet Green, is tried, tested and true for helping with plantar fasciitis. If that doesn’t work, or if there are biomechanical factors contributing to your plantar fasciitis, you can look into custom orthotics.
7. Stress fractures
What are stress fractures?
Stress fractures are micro-breaks of bones are another common foot condition in the elderly. When we age, bone growth slows, losing more bone than we generate. Our bone density also reduces. If your bone density drops too much, you develop osteoporosis. Weaker bones put the elderly at greater risk of stress fractures, whether acute, like when you fall or by too much repetition, like walking.
How can I treat a stress fracture?
The RICE method is critical to treating a stress fracture. Rest, ice, compression, and elevation. Untreated stress fractures can lead to bone shift, permanently altering the foot’s biomechanics.